News

Spotlight on the UCLA Physiology Outreach Program
March 15, 2024
For nearly 15 years, the UCLA Physiology Outreach Program, co-founded by Dr. Tom Vondriska, has helped high school students experience scientific discovery.

A Tribute to Leonard F. Walts, MD (1929 - 2024)
March 15, 2024
Leonard Walts, MD, who passed away in January 2024, is remembered not just for his tremendous contributions to the UCLA Department of Anesthesiology & Perioperative Medicine (DAPM) and the field of anesthesiology, but also for his warmth, integrity, and kindness. Many current and former department members have shared their memories of Dr. Walts and his professional legacy.

SEA-HVO Traveling Fellowship in Vietnam
March 15, 2024
The experience left Dr. Francke with a deep sense of humility and gratitude, along with new friends across the Pacific.

Complex surgery heralds a happy new year for patient and child

DAPM Research Retreat 2024
March 15, 2024
Sixty members of UCLA Department of Anesthesiology & Perioperative Medicine (DAPM) gathered at the Annenberg Community Beach House in Santa Monica.

Informatics Update: A Visit to the Consumer Electronics Show
March 15, 2024
Dr. Cheng represented UCLA Health at the Consumer Electronics Show in Las Vegas, Nevada, in January 2024.

Physician Anesthesiologists Week 2024
January 28 - February 3, 2024
For this Physician Anesthesiologists Week, we are proud to celebrate the dedicated and skilled anesthesiologists that make up DAPM! Physician anesthesiologists are the guardians of patient safety before, during, and after surgery. To all our physicians: thank you for all that you do and have a wonderful Physician Anesthesiologists Week!

Our team of over 50 CRNAs play a vital role in providing safe and effective anesthesia care to our patients, as well as participate in policy development, quality improvement, education, and more. We at UCLA wish our amazing nurse anesthestists a happy National CRNA Week!


Soban Umar, MD, PhD, Named Thomas M. Grove Endowed Chair in Anesthesiology
DAPM members gathered on January 5 to celebrate Dr. Umar's new appointment.

Westwood ASC Named 2nd Best Ambulatory Surgery Center in U.S.

Congratulations to the Westwood Surgery Center for achieving the second highest survey score in Newsweek’s list of America’s Best Ambulatory Surgery Centers for 2024!
Grand Opening of Eugene & Maxine Rosenfeld Hall

Dr. Yue Ming Huang, Executive Director of the UCLA Simulation Center, and other DGSOM leaders celebrated the opening of the center's new home.

Many DAPM members traveled to San Francisco for the American Society of Anesthesiologists (ASA) Annual Meeting.

Resident physicians enjoyed amazing food, music, and ocean views during their annual retreat.

We created this brief Q&A to help us get the word out about the Informatics Division and to help people access clinical data for research or quality purposes.
APSF 2023 Stoelting Conference

November 1, 2023
The Stoelting Conference on “Emerging Medical Technologies” was held in Las Vegas from September 6-7.

Which Fellowship is Right for Me? Part 2
October 26, 2023
Faculty physicians share their insights on how they chose their respective subspecialties.

October 24, 2023
The 34th Annual Extracorporeal Life Support Organization (ELSO) Conference was the largest ELSO event ever conducted.

Launch of the DAPM Global Health Pathway
September 10, 2023
The UCLA DAPM is excited to have created an educational global health pathway for its residents. As of July 2023, seven residents have joined the pathway and have already received their first lecture titled "Introduction to Global Health Equity in Anesthesia."

Summer Research with Dr. Canales and Dr. Singh
September 8, 2023
Six medical students from schools across the country converged in the Department of Anesthesiology & Perioperative Medicine at UCLA to embark on a summer research experience.

CRNA Kern River Rafting Trip
August 23, 2023
With 2 full days of rafting and camping overnight on the shores of the river, there was a lot of teambuilding as well as some peaceful downtime away from busy Los Angeles.

2023 DAPM Residency Graduation
July 12, 2023
DAPM friends, family, and colleagues celebrated the graduation of the DAPM Residency Class of 2023 at Covel Commons on June 17.

DAPM at LA Pride Parade and Dodgers Pride Night
July 11, 2023
DAPM had a strong showing at the LA Pride Parade and Pride Night at Dodgers Stadium.

The First Friends of Oliver Fundraiser
July 10, 2023
The inaugural Friends of Oliver fundraiser, held at Topgolf El Segundo on June 13, was a huge success!

Inaugural CRNA Skills Day
July 5, 2023
UCLA CRNAs, PSSTs, and faculty physicians had a fun and productive day of learning on May 20.

UCLA's La Comunidad Hosts Leadership Event
June 29, 2023
La Comunidad hosted a leadership panel and networking event on June 29, 2023 in the Neuroscience Building Auditorium at UCLA.

Olivia Vallejo Receives UCLA 2023 Outstanding Staff Award
June 21, 2023
Olivia Vallejo, DAPM JEDI Manager, received the prestigious Kevin McCauley Memorial Outstanding Staff Award at the 2023 UCLA Staff Assembly Awards Ceremony on June 21.

DAPM Faculty Social 2023
June 28, 2023
DAPM faculty gathered for delightful food and company on June 28.

DAPM at Euroanaesthesia 2023 in Scotland
June 16, 2023
Dr. Wingert, Dr. Cannesson, and Dr. Joosten participated in the Euroanaesthesia Congress in Glasgow, Scotland in early June.

DAPM Excellence at the SCA 2023 Annual Meeting
June 15, 2023
The Department of Anesthesiology & Perioperative Medicine (DAPM) at UCLA had a phenomenal showing at the Society of Cardiovascular Anesthesiologists (SCA) 2023 Annual Meeting on May 6-9 in Portland, OR. Several faculty, fellow, and resident physicians participated in the conference by presenting various topics or case reports, moderating sessions, helping lead workshops or problem-based learning discussions (PBLDs), and attending committee or governance meetings.
SOAP 2023 Annual Meeting

June 15, 2023
Resident physicians Brittany Burton, MD, MHS, MAS, CA-2, and Jordan Francke, MD, MPH, CA-2, and faculty anesthesiologists Catherine Cha, MD, Richard Hong, MD, and Cristianna Vallera, MD, represented the UCLA Department of Anesthesiology & Perioperative Medicine (DAPM) at the Society of Obstetric Anesthesia and Perinatology (SOAP) Annual Meeting in New Orleans, LA, on May 3-7, 2023.
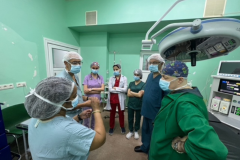
Pediatric Anesthesiologists Begin Collaboration in Armenia
June 12, 2023
Dr. Ayad, Dr. Wilson, and Dr. Salazar traveled to Armenia to establish relationships with children's hospitals there.

DAPM Pride Brunch 2023
June 12, 2023
The DAPM Handoff interviewed K. Elliott Higgins, MD, DAPM Director for Health and Well-Being, about Pride Month and the DAPM Venice Pride Brunch on June 3, 2023.
DAPM Shines at the CSA 2023 Annual Meeting

June 6, 2023
For the past several decades, the Department of Anesthesiology & Perioperative Medicine (DAPM) at UCLA has had a strong presence within the California Society of Anesthesiologists (CSA). DAPM physicians had another impressive showing at the CSA 2023 Annual Meeting in San Diego, CA, from April 27 to 30 this year.

Bioinformatics Annual Retreat 2023
May 10, 2023
The Division of Bioinformatics 2023 Annual Retreat brought the Informatics Team together in-person for a day of team bonding, recognition, and growth.

Brittany Burton, MD, MHS, MAS, and Cristianna Vallera, MD, Awarded 2023 SOAP Diversity & Inclusivity Mentored Grant
April 30, 2023
Congratulations to CA-3 resident physician Brittany Burton, MD, MAS, MHS, and mentor Cristianna Vallera, MD, on receiving the 2023 SOAP Diversity & Inclusivity Mentored Grant for their proposal, “Machine Learning Approaches to Predict Postpartum Hemorrhage for Cesarean Delivery!"

Dr. Selma Calmes, Polio Survivor, Shares Her Story at IARS 2023
April 26, 2023
Dr. Calmes, Retired Clinical Professor of the Department of Anesthesiology and Perioperative Medicine at UCLA and Retired Chief of Anesthesiology of Olive View-UCLA Medical Center, gave a moving account of her own experience with childhood polio and adult post-polio syndrome during the IARS 2023 Annual Meeting.

Administrative Professionals Day 2023
April 26, 2023
The contributions of our administrative staff ensure that our department runs efficiently, that our faculty and staff receive the support they need, and that we are able to excel in all of our core missions — education, research, community engagement, and clinical care. We thank them for their tireless efforts and commitment to excellence.

ASRA Pain Medicine Meeting 2023
April 20-22, 2023
Several trainees and faculty members from the Acute Pain and Regional Anesthesiology Division presented their research and case reports at the 48th Annual Regional Anesthesiology and Acute Pain Medicine Meeting in Hollywood, Florida.

Jordan Francke, MD, MPH, Participates in California Medical Association Legislative Advocacy Day
April 19, 2023
CA-2 resident physician Jordan Francke, MD, MPH, met with several California legislators on priority health care issues in anesthesiology at California Medical Association's 9th annual Legislative Advocacy Day.

DAPM Administrative Managers Attend Engagement and Retention Workshop
April 18, 2023
DAPM Administrative Managers Olivia Vallejo, Carla Gonzalez, Elizabeth Paray, and Lucelva Mendez, as well as Chief Administrative Officer Stephanie Fisher, MA, learned about new tools, resources, and research-based best practices for enhancing departmental onboarding practices at the Engagement and Retention Workshop.

Jordan Francke, MD, MPH, Awarded SEA-HVO Fellowship
April 16, 2023
CA-2 resident physician Jordan Francke, MD, MPH, was awarded the SEA-HVO Traveling Fellowship for international medical education at the Society for Education in Anesthesia (SEA) Spring Meeting in Seattle.

SOCCA, SATA, and IARS Annual Meetings 2023
April 14-15, 2023
Resident, fellow, and attending physicians of the Department of Anesthesiology & Perioperative Medicine (DAPM) at UCLA traveled to Denver, Colorado, to attend the 2023 Society of Critical Care Anesthesiologists (SOCCA), Society for the Advancement of Transplant Anesthesia (SATA), and International Anesthesia Research Society (IARS) Annual Meetings.

Brent Ershoff, MD, MS: Intraoperative hydromorphone decreases postoperative pain: an instrumental variable analysis
April 12, 2023
Using an instrumental variable analysis treating hydromorphone presentation dose (i.e. 2mg versus 1mg vial) as the instrumental variable, Brent Ershoff, MD, MS, shows that increased intraoperative hydromorphone administration causes decreased postoperative pain.

2023 AMG Leadership Conference
April 10, 2023
Quenesha Caballero and Carla Gonzalez participated in professional development workshops and watched keynote speeches from UCLA leaders at the 2023 UCLA Administrative Management Group (AMG) Leadership Conference.

Judi Turner, MD, PhD, Appointed Assistant Designated Institutional Official, UCLA Graduate Medical Education
April 6, 2023
As Assistant DIO, Dr. Turner will develop and cultivate an inclusive culture of teaching excellence and professional development within the community of GME trainees and faculty at UCLA. Congratulations Dr. Turner!

The 2023 DAPM Annual Womxn’s Symposium: Womxn as Educators
April 3, 2023
Jennifer Lucero, MD, MA, DAPM Vice Chair for Justice, Equity, Diversity, and Inclusion (JEDI), and Olivia Vallejo, JEDI Administrative Manager, co-hosted this year's DAPM Womxn's Panel featuring many DAPM leaders in education. The discussion focused on the central roles that women play in education—as both teachers and students in academic medicine, and as members of families and our society at large.

SPA-AAP Pediatric Anesthesiology 2023 Meeting
March 31 – April 2, 2023
At this year’s Society for Pediatric Anesthesia and American Academy of Pediatrics Annual Meeting, DAPM members learned about cutting-edge research within the field of pediatric anesthesiology while also exploring the city of in Austin, Texas.
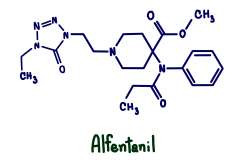
Alfentanil (1976-2023)
April 2, 2023
Mansi Sheth, MD, composed this obituary as a heartfelt farewell to the discontinued medication Alfentanil.

Johnathan Pregler, MD, FASA: The Revenue Sky Is Falling – Are Hospitals the Safety Net?
April 2023
This ASA Monitor article by Johnathan Pregler, MD, FASA, & others covers the recent evolution of economic forces within anesthesiology.

Anesthesia Tech Day 2023
March 31, 2023
Today is Anesthesia Tech Day! We celebrate our Patient Specialty Services Techs as integral members of the anesthesia patient care team. Your contributions are invaluable to the success of DAPM and the overall care of patients at UCLA Health.
Study by Park, Liang, and Umar Using Electronic Remodeling Featured in Pulmonary Hypertension News
March 27, 2023
A study by John Park, MD, PhD, Justine Liang, MD, MS, and Soban Umar, MD, PhD on "Electrical Remodeling in Right Ventricular Failure Due to Pulmonary Hypertension: Unraveling Novel Therapeutic Targets" was covered in Pulmonary Hypertension News and highlighted in ASA Monitor TODAY.

UCLA Anesthesiology Resident Physicians Run 2023 LA Marathon
March 19, 2023
Congratulations to Daniella Goñi, MD, Michael LoBasso, MD, Oliver Drewry, MD, and Adela Perez, MD, on conquering the 2023 LA Marathon!

The 15th Annual DAPM Scientific Evening
March 14, 2023
Our research & clinical trainees showcased research posters and oral presentations at the 2023 DAPM Scientific Evening. Congratulations to all the presenters on your research accomplishments and thank you to our organizers and judges for supporting this event!

2023-2024 DAPM Chief Residents Selected
March 10, 2023
We are pleased to introduce our 2023-2024 Chief Residents: Sara Arastoo, MD, Chase Barker, MD, Mariana Gomez, MD, MBA, and Jennifer Nam, MD, MBA. Congratulations, and we look forward to your leadership!

J. Shin, Grogan, Lee, Liew, Umar, D. Shin, Hoftman: A novel negative pressure isolation device reduces aerosol exposure: A randomized controlled trial
March 6, 2023
The SLACC device protects physicians from infection during airway management. The design for the device was developed by a UCLA team including John Shin, MD, Tristan Grogan, MS, Jason Lee, MD, Elaine Liew, MD, Soban Umar, MD, PhD, Dong Ho Shin, & Nir Hoftman, MD, and will be available for open access.

Catherine Cha, MD, Appointed Interim Chief, Division of Obstetric Anesthesiology
March 6, 2023
Congratulations to Dr. Cha on her new role as Interim Chief, Division of Obstetric Anesthesiology!

"The UCLA Beat" Features Photo and Poem by Zhuang Fang, MD, MPH
March 3, 2023
Artwork by Zhuang Fang, MD, MPH, was selected to be featured in the 2022-2023 edition of The UCLA Beat, the UCLA DGSOM journal of literary and artistic expression. Dr. Fang's photograph (depicted to the right) is entitled "Good Morning, Matterhorn," and his poem is called "Rhythm."

Resident Physicians Conquer Fitness Challenge
February 28, 2023
The UCLA DAPM Resident Wellness Committee hosted a Fitness Challenge over the month of February. From snowboarding at Big Bear Mountain to lifting weights while on 24-hour call, the challenge was a major success in promoting wellness and building connections amongst the resident physicians.

John Park, MD, PhD, Justine Liang, MD, MS, and Soban Umar, MD, PhD: Electrical Remodeling in Right Ventricular Failure Due to Pulmonary Hypertension: Unraveling Novel Therapeutic Targets
February 27, 2023
In this paper from the International Journal of Molecular Sciences, Drs. Park, Liang, and Umar explore the underlying mechanism of electrical remodeling in right ventricular failure due to pulmonary hypertension.
First EXIT Procedure at UCLA
February 26, 2023
In January 2023, a large multidisciplinary team performed the first full-scale ex-utero intrapartum treatment (EXIT) procedure in the Main Operating Room (OR) of the Ronald Reagan UCLA Medical Center.

Belle Benanzea-Fontem, MD Selected as SCA DEI Junior Resident Scholar
February 22, 2023
Belle Benanzea-Fontem, MD, CA-1 Resident Physician, was awarded the 2023 Diversity Equity and Inclusion (DEI) Junior Resident Scholar Grant by the Society for Cardiovascular Anesthesiologists (SCA). Congratulations Dr. Benanzea-Fontem!

Ultrasound exams in the high school library: Project Lead the Way inspires tomorrow’s medical students
February 21, 2023
UCLA Health featured DAPM's collaboration with Project Lead the Way, directed by Sophia Poorsattar, MD, in bringing biomedical curriculum to Los Angeles-area high schools.

Rajesh Kumar, PhD, Awarded New R21 Grant
February 6, 2023
Rajesh Kumar, PhD, has been awarded a new NIH/NINDS R21 Grant entitled, "Brain Metabolites, Brain Antioxidant, and Cerebral Blood Flow Deficits in Single Ventricle Heart Disease."

Emily Methangkool, MD, MPH: Women Physicians Day, 2023 — We Have More Work To Do, but Also a Lot To Celebrate!
February 3, 2023
For Women Physicians Day, we celebrate the trailblazing women in medicine that make up DAPM! Check out this piece by Emily Methangkool, MD, MPH, about celebrating progress for women physicians in anesthesia while recognizing the work that is still needed.

ECMO Symposium 2023
January 28, 2023
The inaugural UCLA ECMO Symposium was a huge success! Dr. Vadim Gudzenko and Dr. Marisa Hernandez-Morgan co-directed the event with cardiac surgeon Dr. Peyman Benharash and ECMO Coordinator Weiting Chen.

Physician Anesthesiologists Week 2023
January 29 - February 4, 2023
For this Physician Anesthesiologists Week, we are proud to celebrate the dedicated and skilled anesthesiologists that make up DAPM! Physician anesthesiologists are the guardians of patient safety before, during, and after surgery. To all our physicians: thank you for all that you do and have a wonderful Physician Anesthesiologists Week!

Jennifer Lucero, MD, MA: Diversity, Inclusion & Equity Efforts in Anesthesiology
January 27, 2023
Jennifer Lucero, MD, MA, DAPM Vice Chair for JEDI, is featured in the ASA "Pathways to Anesthesiology" series. In her video, Dr. Lucero discusses Diversity, Inclusion & Equity Efforts in Anesthesiology.

Beti Asnake, MD: Global Health Equity Ask the Expert
January 26, 2023
In this Open Anesthesia podcast, Beti Anake, MD, MS, DAPM Director of Global Health Initiatives, sits down with Dr. Tirunesh Busha, one of three pediatric anesthesiologists in Ethiopia.

National CRNA Week 2023
January 22 - 28, 2023
Our team of over 50 CRNAs play a vital role in providing safe and effective anesthesia care to our patients, as well as participate in policy development, quality improvement, education, and more. We at UCLA wish our amazing nurse anesthestists a happy National CRNA Week!

Zachary Paquette, MD: Ulnar-Distribution Phantom Limb Pain After Interscalene Brachial Plexus Block
January 16, 2023
Phantom limb pain has historically been a major barrier to recovery for patients after amputation. Here, Zachary Paquette, MD, CA-2 Resident Physician, analyzes "a case of ulnar-distribution phantom limb pain following an upper-extremity amputation despite the use of interscalene blockade."

Maggy Riad, MD, Appointed Expert Reviewer for Medical Board of California
January 13, 2023
Congratulations to Dr. Riad on joining the Medical Board of California as an Expert Reviewer!

Emily Methangkool, MD, MPH, Discusses Considerations Around Non-OR Anesthesia on MedPage Today
January 13, 2023
In MedPage Today, Emily Methangkool, MD, MPH, was quoted in an article on patient safety concerns with the growing use of anesthesia care outside the operating room.

Sungsoo (Danny) Kim, MD, MS: STA 2023
January 11-14, 2023
Danny Kim, MD, MS, PhD candidate, and Maxime Cannesson, MD, PhD, presented two oral and poster presentations at the Society for Technology in Anesthesia (STA) 2023 Annual Meeting in Las Vegas, NV.

Dane Saksa, MD, MBA: Variability in Resource Utilization in the Evaluation and Management of Simple Febrile Seizures Inpatients in US Children’s Hospitals
January 1, 2023
In the January 2023 issue of the Journal of Neurosurgical Anesthesiology, Dane Saksa, MD, MBA conducted a study to characterize resource utilization in the treatment of hospitalized patients with simple febrile seizure in US children's hospitals.