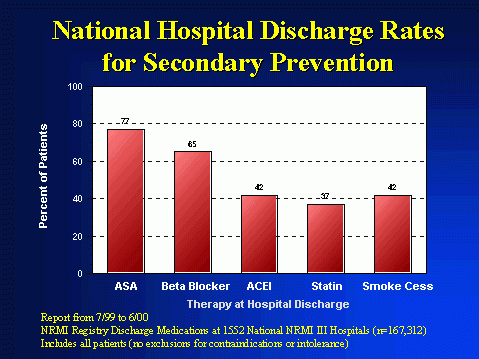
National Registry of Myocardial Infarction Treatment Rates
Data from the National Registry of Myocardial Infarction provides information on the current treatment rates at hospitals across the country for patient being discharged after myocardial infarction. It involves over 1500 hospitals of all types and from all regions. More than 5% of the total AMI patients hospitalized in the US are entered into the registry. The treatment rates in this patient population likely reflects patterns in other patients hospitalized with coronary heart disease. This registry allows hospitals to compare their own treatment rates to this national data set. It is however clear that a substantial opportunity exists to improve treatments rates at each hospital across the country.
From the most recent data set involving over 160,000 patients discharged after myocardial infarction, only 77% of patients were discharged on aspirin, only 65% of patients were discharged on beta blockers, only 42% of patients were discharged on ACE inhibitors, and only 37% of patients were discharged on lipid lowering medication. In patients who currently smoke only 40% were documented to have received advice to stop smoking.
CHAMP demonstrates that it is possible to dramatically improve these treatment rates though the use of a focused hospital based treatment program. Image the impact if similar programs were to implemented at hospitals across the country.