Research Projects

The following are all current UCLA Brain SPORE research projects.
Project 1
Targeting Immunotherapy-induced Resistance with DC Vaccination and Immune Modulation
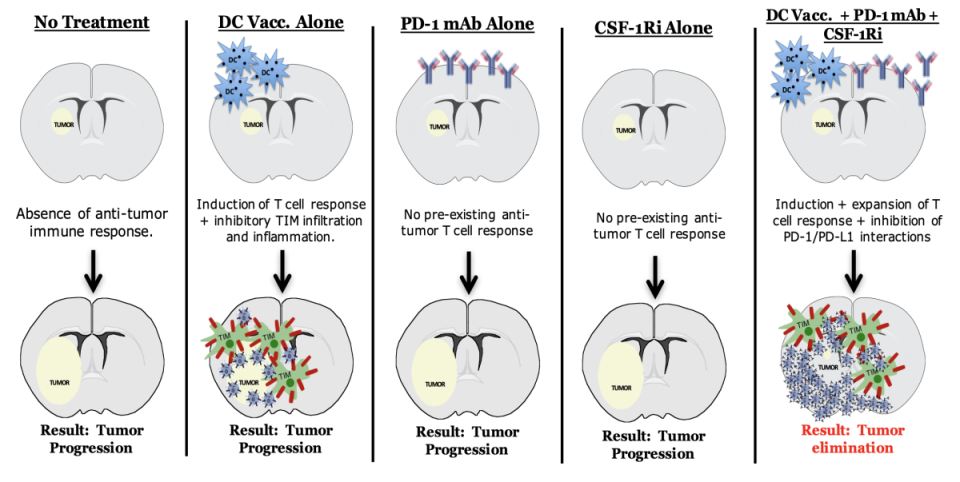
The overall goals of this project are to investigate mechanisms of immune evasion following treatment with dendritic cell (DC) vaccines, and to develop rational combinations of immunotherapeutic strategies to overcome the immunosuppressive milieu of the brain tumor microenvironment.
We previously found that, in addition to inducing T-cell infiltration into brain tumors, DC vaccination + anti-PD1 blockade may also create a pro-inflammatory environment within the tumor that induces the immigration of immunosuppressive myeloid cells (TIM). TIM are phenotypically similar to the myeloid cells that attenuate the T-cell response to chronic viral infections, and may counteract the anti-tumor T-cell responses induced by DC vaccination. Therapies that target myeloid cells within the tumor microenvironment represent a promising new strategy. As such, inhibition of these myeloid cells using a CSF-1R inhibitor, in conjunction with autologous tumor lysate-pulsed DC vaccination (ATL-DC) and PD-1 mAb blockade, resulted in significantly prolonged survival in tumor-bearing animals with large, well-established intracranial gliomas.
Our hypothesis is that myeloid cells mediate adaptive immune resistance in response to T-cell activation induced by immunotherapy. We have planned a series of novel pre-clinical studies to re-polarize myeloid cells, to optimize how the timing and sequence of immunotherapy can influence ant-tumor immunity, and a new clinical trial to test the first-in-human combination of a new brain penetrant CSF-1R inhibitor (CSF-1Ri; PLX3397, Daiichi-Sankyo) with DC vaccination and PD-1 mAb blockade (Pembrolizumab, Merck) in patients with newly diagnosed GBM. A better understanding of the biology of these cellular interactions will provide insight into more effective ways to induce therapeutic anti-tumor immune responses for this deadly type of brain tumor.
- Aim 1: To identify the optimal timing and sequence by which immunotherapy alters the local tumor-infiltrating immune response in syngeneic murine glioma models and in recurrent glioblastoma patients.
- Aim 2: To conduct a new first-in-human Phase I clinical trial of ATL-DC vaccination in conjunction with CSF-1R inhibitor (PLX3397) and PD-1 mAb (Pembrolizumab) blockade, and develop predictive immunological and imaging biomarkers.
- Aim 3: To elucidate the immunotherapy-induced resistance mechanisms by which immuno-suppressive myeloid cells inhibit anti-tumor immune responses in pre-clinical animal models and in newly diagnosed glioblastoma patients.
Project 2
Overcoming Drug-induced Resistance to Intrinsic Apoptosis in Glioblastoma
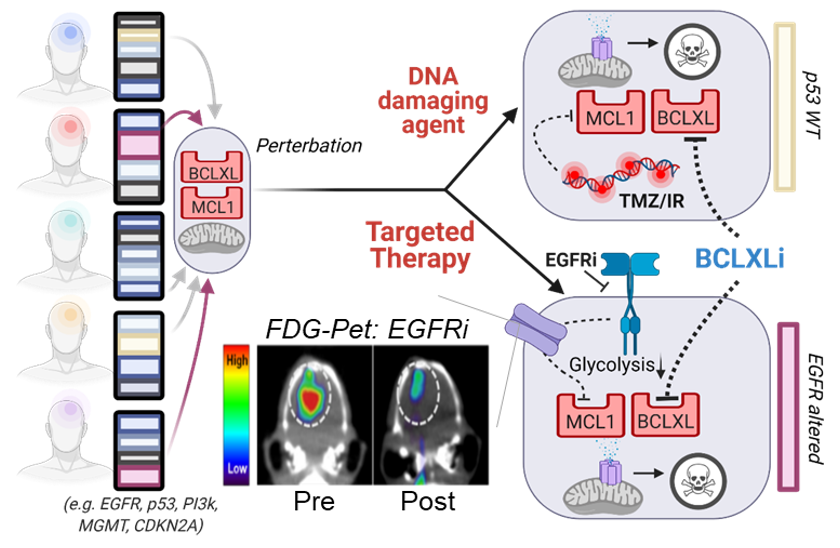
Glioblastoma (GBM) tumors are defined by high resistance to therapy-induced cell death. Through a combination of molecular and functional profiling of the intrinsic apoptotic machinery, we have identified that all GBM are comprised of two molecular intrinsic apoptotic blocks – MCL-1 and BCL-xL – to prevent tumor cell death. The goal of Project 2 is to translate rationally-designed drug combinations, consisting of new and pre-existing clinical agents, that selectively ablate the GBM dual apoptotic barrier to promote tumor cell death and induce durable clinical responses in patients.
- Aim 1: To investigate whether a novel, antibody drug conjugate with a potent warhead against an essential apoptotic block has anti-tumor effects when combined with TMZ/radiation or a new, clinical brain penetrant EGFR TKI in pre-clinical GBM models.
- Aim 2: To conduct a “window of opportunity” clinical trial to explore whether these new clinical drugs can ablate the two intrinsic apoptotic blocks in recurrent GBM patients.
- Aim 3: To identify potential mechanisms of resistance to targeting the intrinsic apoptotic machinery in diverse pre-clinical GBM samples.
Together, the studies proposed in this application present a new therapeutic paradigm through specific manipulation of intrinsic apoptotic pathways in malignant glioma and have the long-term potential to shift current approaches in glioma therapy.
Project 4
Targeting Glioblastoma Cells and Tumor Microenvironment with Bispecific CAR-T Cell Therapy to Overcome Resistance
Glioblastoma multiforme (GBM) is the most prevalent primary brain tumor among adults, with poor patient prognosis despite aggressive treatment regimens combining chemotherapy, surgery, and radiation. Immunotherapy is an appealing strategy because of the potential ability for immune cells to traffic to and destroy infiltrating tumor cells in the brain. Engineering T cells to express tumor-targeting chimeric antigen receptors (CARs) offers a tantalizing means to induce targets for CAR-T cell-based immunotherapies. Prior clinical trials have shown the safety of CAR-T cell therapy targeting interleukin-13 receptor subunit alpha-2 (IL-13Rα2), an antigen that is overexpressed by 58-78% of gliomas. However, the highly immunosuppressive tumor microenvironment (TME) is a major barrier hindering the effectiveness of these immunotherapies against GBM, with transforming growth factor-beta (TGF-β) playing a particularly prominent role. We have now developed a bispecific CAR that simultaneously targets TGF-β and IL-13Rα2, and observed superior in vivo anti-tumor efficacy against both patient-derived GBM xenografts and syngeneic gliomas in immunocompetent mice compared to single-input IL-13Rα2 CAR-T cells. Our central hypothesis is that IL-13Rα2/TGF-β bispecific CAR-T cells can directly attack GBM via IL-13Rα2 recognition and simultaneously disrupt the immunosuppressive feedback loop between TGF-β and tumor-infiltrating myeloid cells. In this SPORE Project, we have planned a series of studies with the following specific aims: 1) to optimize clinical-grade cell manufacturing of IL-13Rα2/TGF-β CAR-T cells for clinical testing; 2) to conduct a new first-in-human clinical trial of a novel IL-13Rα2/TGF-β bispecific CAR-T cell therapy for patients with recurrent glioblastoma; and 3) to determine correlates of response and potential resistance mechanisms to this novel therapeutic approach. At the conclusion of this grant, we hope to address some of the major hurdles of CAR T cell therapy for GBM by targeting both glioblastoma cells and the immunosuppressive tumor microenvironment. If successful, this project will expand our immunotherapeutic armamentarium and potentially help to enhance tumor eradication, thereby improving outcomes for patients with GBM.
IL-13Rα2/TGF-β bispecific CAR-T cells can simultaneously attack tumor cells through surface-antigen recognition and convert TGF-β in the tumor microenvironment (TME) from a suppressive cytokine into a T-cell stimulant. The bispecific CAR-T cells can both serve as a sink for TGF-β and produce inflammatory cytokines in response to TGF-β, further promoting endogenous immunity in the TME.

Seed Grant Programs
Read more about previously funded projects of the Developmental Research Program and the Career Enhancement Program.