What is a Lumpectomy?
Find Your Care
UCLA Health’s Breast care specialists develop a personalized plan to help you recover. For more information, reach a cancer care specialist at 310-825-2144.
Lumpectomy
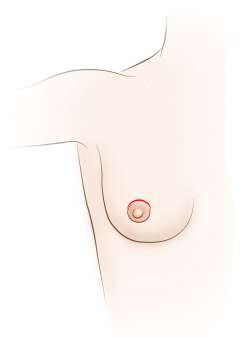
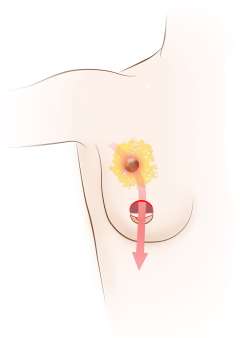
A lumpectomy, also called a partial mastectomy, is the most common operation performed for breast cancer. A lumpectomy implies removal of a lump of breast tissue with the intention of obtaining clear margins around the area of disease. It is sometimes performed for atypical or precancerous breast abnormalities as well as large or enlarging benign breast lesions, but it is most commonly performed as a part of breast cancer treatment.
A lumpectomy, as part of breast conserving surgery, refers to removal of only a portion of the breast as opposed to a mastectomy which refers to removal of the entire breast.
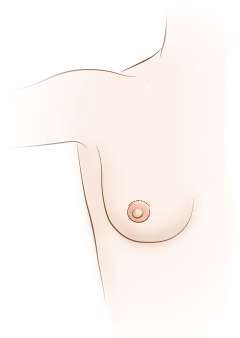
The goal of the lumpectomy procedure is to remove the breast cancer while preserving the aesthetic appearance of the breast. Because only part of the breast is removed, occasionally patients will need a second surgery to achieve negative margins based on final pathology. Sometimes wires are placed by the radiologist prior to surgery to help the surgeon localize tumors that cannot be felt on exam to better guide the lumpectomy resection and achieve clear margins.
Patients who are good candidates for lumpectomy have a tumor or tumors close enough together such that the amount of breast tissue needing to be removed with a clear margin will not disturb the shape of the breast, enough to avoid a negative psychological impact on the patient. Your surgeon should be skilled and experienced in the procedure and obtaining the desired result. Oncoplastic techniques are available to improve cosmetic outcomes after lumpectomy and these techniques are employed by surgeons with advanced training or in conjunction with a plastic surgeon.
A lumpectomy surgery is typically performed in the outpatient setting under anesthesia, either general or monitored anesthesia care. Risks for lumpectomy are minimal and include bleeding, infection,
seroma (excessive fluid collection in the lumpectomy cavity), wound healing issues and change in breast size and shape. Patients generally do not have significant pain after a lumpectomy, but the breast can be swollen, bruised or tender for a few days to a week or two after surgery depending on a patient’s breast size and size of the tumor removed. Drains are usually not used after lumpectomy surgery.
Pathologists then take time to thoroughly review all tissue removed at surgery. This generally takes several working days to fix, cut, stain and review all the specimens. As difficult as it is to wait for final results, it is exceedingly important to afford the pathologists the time they need to perform a complete and accurate analysis of your cancer. This will determine your final cancer stage, need for any additional surgery and provide the information that your medical oncologist and radiation oncologist need to determine your next steps after surgery.
Patients who are better suited for mastectomy with or without reconstruction include those (1) whose tumors are too large for lumpectomy with a nice cosmetic result, (2) two or more tumors in different areas of the breast, (3) patients who cannot receive radiation therapy for some reason such as scleroderma, prior radiation therapy to the breast, or logistical issues, (4) BRCA gene positive, (5) significant skin or muscle involvement, e.g. inflammatory breast cancer, or (6) personal choice.
Phone: 800-UCLA-MD1 or 424-424-0273