Orthopedic Surgery
Mobility and Motor Function
Abnormal muscle tone, along with poor motor control or coordination, can make walking and other motor skills difficult for people with cerebral palsy. In the growing child, it can affect bone and joint development. We utilize many different non-operative methods such as therapy, bracing, casting and adaptive equipment to achieve an individual’s mobility goals, including sitting, standing and walking. For our pediatric patients, the UCLA/LOIC CCP utilizes a team approach to evaluate and maximize your child’s mobility and function as he or she grows.
For some patients, the orthopaedic surgeon may recommend surgery to optimize mobility, improve independence, and prevent pain. For patients who walk, an evaluation may be performed at the Center’s Kameron Gait & Motion Analysis Laboratory to assist in treatment planning. This is especially important if surgery is a consideration to improve mobility. After the team reviews the gait data, surgery may be recommended and can include:
- Tendon/muscle lengthening for muscles that are limiting joint mobility and function
- Tendon/muscle transfers to “balance” tighter muscles with less-tight muscles
- Bone surgery to correct deformities and improve alignment
Hip Surveillance
Typically, certain muscles are more spastic than others. This muscle imbalance, combined with delayed weight bearing, may lead to hip dislocation, when the top of the femur (thigh bone), moves out of the hip socket. Hip dislocation in children with cerebral palsy is associated with difficulties in sitting, personal care and hygiene and pain or scoliosis (curvature of the spine) may occur. The team at the UCLA/LOIC CCP is committed to preventing hip dislocations in children with cerebral palsy by performing regular exams and obtaining x-rays over time. This is called hip surveillance. Our method of hip surveillance is based on evidence and best practice from clinicians around the world.
The UCLA/LOIC Center for Cerebral Palsy hip surveillance and treatment program includes:
- Clinical evaluation every 6 months by the pediatric orthopaedic surgeon
- Periodic x-ray evaluation based on your child’s mobility
- Surgical release of spastic muscles for “hips at risk” – hips that are partially dislocated, or “subluxated”, to prevent full dislocation
- Surgery of the hip and pelvic bones for more severely affected hips (those with a greater amount of subluxation) in older children
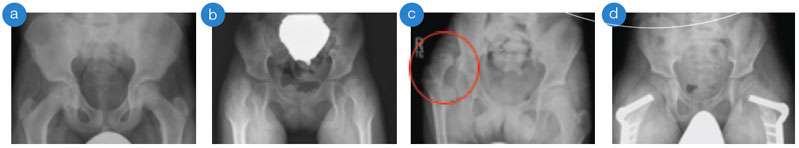
(a) normal hips and pelvis, (b) subluxated/partially dislocated hips, (c) right dislocated hip (circle), (d) after surgical correction of subluxated hips with plates and screws
Spine Surveillance
Unlike hip surveillance, there is no evidence that radiographic (x-ray) screening for scoliosis improves outcomes. Instead, the orthopaedic surgeon evaluates your child’s spine twice yearly and obtains sitting x-rays only if scoliosis is observed during the exam. Some curves are flexible, meaning they change based on the child’s position, while others are fixed. We treat scoliosis using a number of different methods.
- Seating modifications are recommended for patients who use a wheelchair as their primary means of mobility. These modifications may partially correct a flexible scoliosis to allow optimal sitting function.
- Braces (orthoses) are used in mild, flexible scoliosis in children who walk.
- Surgical stabilization, typically with a rod and screws, is offered to patients whose curves becomes too large or too stiff for wheelchair modifications or a brace to control.
Orthopaedics, Cerebral Palsy & Science
We are continually involved in research studies that will further advance our understanding of cerebral palsy and improve care for children with cerebral palsy. In this light, we may periodically offer you and your child with the opportunity to be involved in our ongoing research projects.