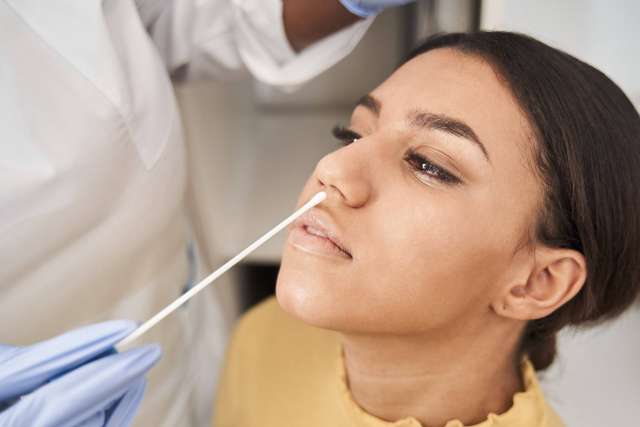
Say you’re having a big party. You want to be COVID-safe, so you check guests for the virus using a rapid antigen test before they enter the venue. They swab their nose on the spot, wait 15 minutes for the result, and come into the event believing they — and the other attendees — are free of COVID-19.
Unfortunately, this approach creates a false sense of security, says Omai Garner, PhD, director of clinical microbiology for UCLA Health. A person could actually be infected with COVID-19 but have virus levels below what an antigen test can recognize.
“It takes a lot of virus to make an antigen test positive,” Dr. Garner says. One’s viral load could be growing as the individual mixes and mingles at the party, unwittingly turning it into a super-spreader event.
“That’s the real challenge of the desire to use antigen testing asymptomatically, and I don’t endorse that at all,” Dr. Garner says. “Because a person could have a lower amount of virus than is the threshold for an antigen test and still either be contagious or be moving toward contagious pretty rapidly. So you could antigen-test negative at the start of the wedding, but four hours later, now you have enough virus to be contagious.”
What’s the difference between antigen tests and PCR tests?
Antigen tests are available over-the-counter for at-home use. Granted emergency use authorization by the U.S. Food and Drug Administration in December 2020, these tests typically use nasal swabs and a reagent solution to look for a protein particular to SARS-CoV-2, the virus that causes COVID-19.
Antigen tests are far less sensitive than polymerase chain reaction, or PCR, tests, which detect genetic material from the virus. PCR tests must be performed by a laboratory and results can take hours or days.
Both antigen and PCR tests can identify active COVID-19 infection, but PCR tests can do so when an individual is asymptomatic or viral levels are still emerging.
“A PCR test is exquisitely sensitive, so it can measure a much lower level of virus,” says Dr. Garner, who pioneered in-house COVID-19 testing at UCLA Health. “PCR tests done in a laboratory are the most accurate way to test for COVID. I don’t see a scenario where antigen testing should be used in the asymptomatic population, because the viral load is not high enough.”
When should you use an antigen test?
Dr. Garner says he keeps antigen tests in his home medicine cabinet to help him distinguish whether respiratory symptoms, such as a cough or stuffy nose, are caused by a cold or COVID-19.

“If somebody is symptomatic, and it’s COVID, they should have a lot of virus at that point,” he says — enough to trigger an antigen test to come up positive.
If you have cold symptoms, an antigen test can help you determine whether you need to isolate from other members of your household. If the antigen test comes back positive, Dr. Garner advises isolating immediately and confirming results with a PCR test. Antigen tests can return false positives, he says.
If an antigen test comes back negative but symptoms worsen the next day, or include a fever, a PCR test is a good idea, he says: “If it's a fever, it's time to go get the gold-standard test performed in a professional laboratory, so that you can be sure of the result.”
Symptoms such as congestion, aches and fever could point to COVID-19 or the flu, so symptomatic patients screened at UCLA Health are tested for both, Dr. Garner says.
With both PCR and antigen tests, access and availability are potential issues.
Antigen tests are sold out in some parts of the country, and at $25 for a two-pack, could be financially out of reach for some families. PCR testing is even more expensive – at least $150 --particularly for those paying out-of-pocket, and typically require a trip to a testing site or medical center.
If a PCR test isn’t an option and an individual has cold symptoms, an antigen test can be helpful, if not definitive.
Says Dr. Garner: “The onset of rapid testing in the home, these antigen tests create an interesting new tool for us to be able to fight COVID in the midst of an upcoming respiratory viral season.”
Stay up to date on the latest COVID-19 information related to the virus, testing, vaccines and more.
Related articles
How viruses, including the coronavirus, make you sick
Will children 5 to 11 soon be able to get their COVID-19 vaccines?
Study finds people with blood cancer need more protection against COVID-19, even if vaccinated