Many veterans who suffer concussions or more severe traumatic brain injuries (TBI) live with chronic disabling symptoms, including migraines, disrupted sleep, mood disorders and cognitive difficulties. Now, UCLA’s Operation Mend has launched an intensive-treatment program, called the Balanced Recovery and Integrated Neuroscience (BRAIN) program, to address the neurologic, psychological and social needs of these wounded warriors and their families.
“There is a somewhat intertwined, but also distinct, need for TBI-specific treatments that don't overlap completely with post traumatic stress disorder treatments,” says Assistant Professor of Neurology Kevin Bickart, MD, PhD, lead neurologist of the BRAIN program. “We proposed this TBI-specific track to address not only the psychological trauma of going through combat, but also to care for the warriors’ neurologic injuries and promote their overall brain health.”
Operation Mend has been providing world-class, personalized treatment to post-9/11-era veterans since 2007. The program began with a focus on reconstructive and plastic surgery for service members who had suffered highly complex facial injuries.
In 2016, the Wounded Warrior Project partnered with UCLA Health and three other medical centers to launch the Warrior Care Network, an initiative to provide mental health services for veterans experiencing PTSD. All care, travel and accommodations are arranged for and provided at no cost to the patients and their family members.

Veterans participating in these existing programs already receive neurologic assessments from UCLA Health’s multidisciplinary team of TBI experts. The BRAIN track provides TBI-specific neurologic care, including exercise and occupational therapy, nutrition and brain-health education to help the veterans and their families understand their symptoms and safely return to regular exercise and daily activities.
“Before, we were able to do an assessment based on one visit and make neurologic recommendations that they could take back to their home neurologist or primary care physician,” says neurologist Meeryo Choe, MD, assistant professor of pediatrics. “Now, we can take a comprehensive integrated-therapy approach to treat that particular veteran who is suffering from TBI and some of its long-term sequelae.”
The legacy of TBI
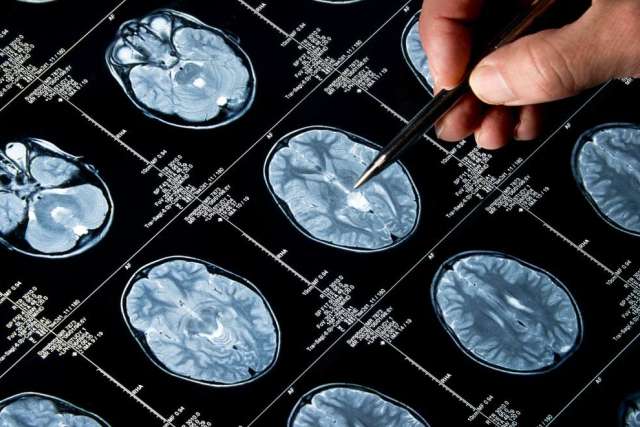
TBI can be caused by a physical blow to the head, a force such as an explosion or vehicle collision that jolts the brain inside the skull, or by an object that pierces the skull and enters the brain.
Although the brain can physically heal within a few weeks from a concussion or mild TBI, up to 20% of people may develop chronic symptoms. This is especially common when the injury is due to violence or a psychologically traumatic event, Dr. Bickart says.
“In addition to the traumatizing nature of the event itself, the other key piece is the aftermath of the event,” he adds. “If the aftermath is that you didn’t get enough rest, and you're thrown right back into combat, or, conversely, if you have a prolonged rest period, you're more likely to have persistent symptoms. There’s a fine line between rest and return to activity in which personalized recommendations are needed to optimize recovery.”
If not addressed, those symptoms can compound, he says. For instance, disorientation or lowered reaction time can lead to other injuries, and this can contribute to additional psychological distress.
“After a TBI, there is usually some cognitive slowing, disorientation, dizziness and/or headaches. That is typical and will go away as you gradually return to your regular level of activity,” explains Dr. Bickart. “But if they're not given that education and understanding of what to expect, and they experience one failure after another, that adds more stress. Solving persistent symptoms after TBI relies on warriors’ ability to cope with this cumulative stress using existing tools or having the access and opportunity to acquire new tools.”
Operation Mend’s TBI program addresses this issue by including both an intense integrated neuroscience education component and an exercise regimen to help veterans understand the neurology of TBI. By gradually ramping up their activity level using exercise equipment with concurrent heart-rate monitoring and personal coaching, the warriors learn to recognize their mental and physical limits as they progress toward higher levels of exertion.
“They might have been avoiding exercise because it triggers discomfort or pain, like migraines,” says Dr. Bickart. “It is common sense that if something is hurting you, you avoid it, especially if you believe that pain might be damaging your brain. We're educating them that the pain does not mean it's damaging their brain and those activities should be avoided; they should be gradually brought back into their life.”
“Biking is relatively low-impact compared to something like running,” says Dr. Choe. “We have access to hundreds of online classes on different types of exercise, including floor-based cardio workouts, yoga, meditation, body-weight strength, weights-based strength. This will help improve the likelihood that we are able to find some sort of body movement they enjoy. The goal is that they return home and continue all the things we’ve helped them to integrate into their schedule.”
Success after the program
In addition to the education and exercise components, the program offers training in brain-healthy nutrition, occupational therapy to help resume other daily activities, and neuropsychology for healthy coping and adjustment.
“Occupational therapy is a critical piece of the intensive-treatment program,” says Dr. Bickart. “It helps the warriors to consider their desires, their goals, their priorities, and to come up with plans and practical milestones to achieve those goals. With this unique approach to occupational therapy and the combination of disciplines involved in the BRAIN program, warriors have an unparalleled opportunity to learn about their minds, brains and bodies to make lasting, evidence-based changes in their lives.”
UCLA Health’s program also offers training and support for a caregiver, such as a spouse, child, sibling or friend. After the three-week on-site program at UCLA, the veteran and caregiver return home, and a case manager helps transfer the routines and recommendations they learned in the program back to their home environment.
“With the multidisciplinary approach, everybody comes together to make sure that we’re seeing to all aspects of the life of the veteran and the caregiver, and also to how the brain is functioning,” says Dr. Choe. “That multidisciplinary approach works for people who are having a lot of struggles in their work or home life because there may be many contributory pieces to their pain and dysfunction.”
Caroline Seydel is the author of this article.