Epidural Corticosteroid Injection
Find your care
At the UCLA Health Spine Center, our experts diagnose, manage and treat all spinal injuries and conditions. Call 310-319-3475 to connect with a spine specialist.
Fax: 424-259-6560
Spine Injection Procedures for Pain Management
Spine injection procedures have been employed in the management of patients with cervical, lumbar, and radicular pain syndromes for almost a century. The first report of epidural steroid injection was in 1951.
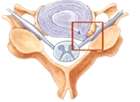
- Corticosteroids are known to have strong anti-inflammatory properties. Locally, corticosteroids act to inhibit the inflammatory response induced by mechanical, chemical, or immunologic agents.
- Epidural steroid injection is a term applying to a variety of techniques performed to deliver a corticosteroid preparation into the epidural and perineural spaces of the spine.
Three routes may be used in the lumbosacral spine:
- Caudal
- Translaminar
- Transforaminal epidural injections
The translaminar injection offers a potential advantage of delivering solutions directly into the epidural space and therefore closer to the source of pain, however, the medication is placed away from the disc, without any guarantees that it will flow to the front epidural space where the disc-nerve root pathology is occurring. The transforaminal technique requires fluoroscopic guidance for precise needle placement. This technique is favored by some, because of the precision with which solutions can be delivered to a specific nerve root and the front location of the needle in the epidural space. If fluoroscopy is not available, generally the caudal route is preferable for disc pathology at the L5/S1 level and the translaminar route for lesions above this level.
Several different steroid preparations may be used, with or without local anesthetic or normal saline, to increase the volume and ensure the spread of medication to all areas causing pain.
The primary indication for an epidural steroid injection is the relief of pain due to inflammation of the nerve elements in the epidural spaces of the spine, however, the question of when an epidural steroid injection should be administered has not been thoroughly studied. The decision on how often an epidural steroid injection should be administered is also unknown.
There are few contraindications to performing lumbosacral epidural steroid injections: a bleeding disorder, anticoagulation, and allergy to medications. Diabetes and congestive heart failure require caution. The current use of aspirin or nonsteroidal anti-inflammatory drugs is not an absolute contraindication, but most physicians ask patients to stop seven days before the planned injection.
Complications are uncommon, and usually temporary and serious complications are rare. Infections may be introduced by injection techniques. Inadvertent dural puncture, which occurs in about 5% of translaminar and 0.6% of caudal injections, may occur. A vasovagal reaction associated with deep pain of injection is another complication associated with these injections. Intravenous injection is also possible, but can be prevented using fluoroscopy. Last, the injection procedure may not improve a patient's pain.
The whole point of using an injection is to place the medication as close to the pathologic process as possible in order to gain the best therapeutic benefit. The treatment is used to achieve a significant reduction in pain without the need for surgery. More than a single injection may be required in any given patient.
Further information can be found at spineuniverse.com.