Medical Mission Trips
On this page:
Nurse Anesthetist Thao Hoang Hones Skills on Mexicali Mission
Nurse Anesthetist Debbie A. Paris Teho Provides Hernia Treatment in Haiti
Nurse Anesthetist Thao Hoang Hones Skills on Mexicali Mission

Last fall, I attended my fourth medical mission to Mexicali, Mexico with the organization Interface. Interface was established in 1977 and provides cleft lip and palate and other plastic reconstruction surgeries to the children and adults of Mexico. Interface serves five different sites in Mexico, once or twice each year. Attendees spend two to five days each trip performing between 10 and 75 surgeries.
My team consisted of over fifty volunteers, including surgeons, anesthesiologists, nurse anesthetists, pediatricians, nurses, scrub technicians, and interpreters. We stationed ourselves at the Red Cross clinic, converting three patient clinic rooms into five operating beds. We also established a pre-screening room and a post-anesthesia care unit.
Patients were screened by a pediatrician, surgeon and an anesthesia provider. The clinic supplied us only with space and oxygen cylinders. We brought our own anesthesia airway equipment, supplies and medications. We did not have anesthesia machines, but used Bain circuits to deliver oxygen and anesthesia gases. We also made sure the environment had the necessary safety measures needed in an operating room.

In two days, we performed over 50 surgeries, on patients two to 40-years-old. We performed cleft lip and or palate repair, syndactly excisions, scar revisions, microtia repairs and septoplasties. Each patient was escorted into the operating room, placed on monitors and mask-induced with sevoflurane and oxygen. After a peripheral IV was established, intubation was performed without the use of muscle relaxants, and spontaneous ventilations were resumed. Fentanyl and clonidine were administered for pain and sedation judiciously. At the end of surgery, the patient was extubated and transported to the recovery room. Most patients were discharged the same day, while those that had cleft palate surgery or needed more monitoring stayed the night.
It is always challenging to provide anesthesia in unfamiliar surroundings with limited resources. On the trip, I became more comfortable using the Bain circuit and honed my skills in managing the pediatric airway. The use of clonidine intraoperatively provided great analgesia and sedation in the patients. An intravenous dose of 0.5mcg/kg provided very satisfactory sedation and pain control.
This trip was rewarding and humbling. I felt a sense of accomplishment seeing the patients do well after receiving their anesthestic and surgery. It is always a pleasure serving a population in need of medical services. The patients were grateful, and I know that we made a positive impact on their lives. Also, I was truly impressed by the skill and work ethic of the volunteer team. I look forward to continuing many more medical missions with Interface, an amazing and hard-working organization.
Nurse Anesthetist Debbie Paris Teho Provides Hernia Treatment in Haiti
Hernia repairs are among the most common operations performed anywhere. But prior to this mission trip with the nonprofit organization Hernia Help, I did not realize how widespread and debilitating the diagnosis of a hernia can be. One in every four men and one in every 50 women around the world will suffer from a hernia in their lifetime. The problem is without boundaries, and affects members of every country, ethnicity, and socioeconomic status.
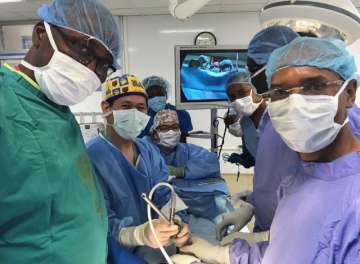
In May 2018, I was fortunate to participate in a medical mission to Port-au-Prince, Haiti. The week-long mission was conducted at Hôpital St. François de Salle. Hernia Help provides free hernia surgery to underserved adults and children. It also strives to train, mentor, and support local general surgeons who will serve as independent trainers and educators in hernia surgeries. The ultimate goal is to assist hospitals in creating self-sustaining hernia repair teams to care for the local community.
Our team hailed from UCLA and the University of Nebraska, and included two surgeons, two surgical residents, a pediatric anesthesiologist, a critical care pulmonologist, an advanced-practice pediatric nurse, five nurses, and myself. UCLA surgeon David Chen, MD, was our team leader. Our UCLA team provided care for all adult patients, while the University of Nebraska handled all pediatric cases. The hospital staff was essential in orienting us to hospital practices and assisting in the operating room. Two local interpreters were immediately available to us since most of the people we encountered spoke Haitian Creole and little or no English. My limited French was of little help, as I learned that Haitian Creole is completely different!
Patients were screened the day before surgery by Joanne Bando, MD, who is a critical care pulmonologist at Santa Monica UCLA. Dr. Chen and I reviewed all cases with preoperative concerns, and the team determined patient suitability. Our team performed 24 hernia operations during the week. Depending on the patient and the type of hernia, the surgeries were done either with open or laparoscopic techniques.
I experienced several challenging airways within our patient population, and was fortunate that Dr. Chen brought a videolaryngoscope to donate to the hospital. This was a welcome and unexpected luxury on a mission trip! The anesthesia personnel in Haiti had heard of a videolaryngoscope but had never seen or used one before. I had the pleasure of instructing them on its use.
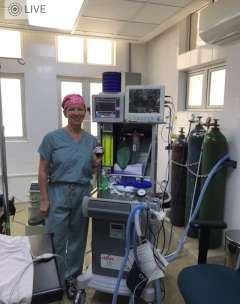
The hospital has a very sophisticated anesthesia machine called the UAM (Universal Anesthesia Machine). Produced in the UK, it is a compact machine perfect for a location where there are few resources and a constant threat of power outages. The machine is capable of running for six hours on a rechargeable battery. It also has an oxygen concentrator that entrains room air and removes the nitrogen, thus producing a higher concentration of oxygen. There was no additional oxygen source; I had to rely on the concentrator.
Each morning the OR charge nurse supplied me with a tray of medications for the day. This included midazolam, fentanyl, propofol, cefazolin, and their version of IV acetaminophen called Neomol (paracetamol). Many of the medications are donated by mission teams like ours.
But with some unexpected luxuries also came unexpected challenges. The anesthesia machine lacked end-tidal carbon dioxide monitoring, isoflurane was our only inhaled agent, and there were no infusion pumps for propofol. I definitely found myself practicing outside of my comfort zone. We did many cases under monitored anesthesia care (MAC), and I had to get creative with the propofol infusions. I injected propofol into the liter bottle of saline and used the roller clamp to titrate to effect. This worked quite well. Overall, I feel I was able to provide safe, effective anesthesia for our patients.
I am looking forward to returning to Haiti with Dr. Chen next year. It was such a rewarding experience to help people who would otherwise be unable to work or take care of their families, and would have to live in extreme pain on a daily basis. With such unrest in the country lately, we have not set a definite return date. We are hoping for peace for the people of Haiti, and look forward to being of service again soon.