What are fibroids?
Find your care
You receive exceptional care and personalized pain management from an expert team. Call to connect with our fibroid experts.
OB/GYN appointments
If you’re looking to review fibroid treatment options with an OB/GYN provider or want a second opinion, please call: 310-794-7274
Radiology appointments
If you already have a provider helping you manage a fibroid condition and are interested in uterine artery embolization (UAE) treatment, please call 310-481-7545.
Uterine fibroids overview
What is a fibroid? Fibroids are tumors made of smooth muscle cells and fibrous connective tissue that develop in the uterus. It is estimated that 70 to 80 percent of women will develop fibroids in their lifetime — however, not everyone will develop symptoms or require treatment.
The most important characteristic of fibroids is that they’re almost always benign, or noncancerous. That said, some fibroids begin as cancer — but benign fibroids can’t become cancer.
Cancerous fibroids are very rare. Because of this fact, it’s reasonable for women without symptoms to opt for observation rather than treatment.
Studies show that fibroids grow at different rates, even when a woman has more than one. They can range from the size of a pea to (occasionally) the size of a watermelon. Even if fibroids grow that large, we offer timely and effective treatment to provide relief.
In addition to understanding what a fibroid is, here are some other key points about uterine fibroids you should be aware of:
- Uterine fibroids are the most common tumor of the reproductive tract.
- Women who are nearing menopause are at the greatest risk for fibroids.
- Fibroids are most often found during a routine pelvic exam.
- Symptoms may include heavy and prolonged periods, bleeding between periods and pelvic pain.
- There are a variety of treatment options available.
Types of fibroids
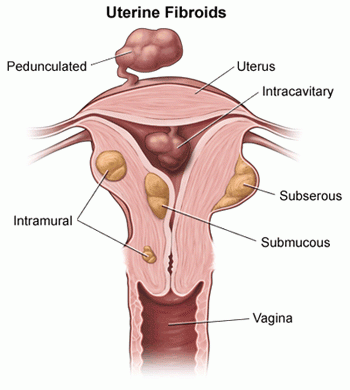
Now that you know what a fibroid is, it’s time to discuss types of fibroids. Along with the size and number of fibroids, the type can also affect treatment recommendations. The three main types of fibroids include:
- Subserosal fibroids: These are the most common fibroids. They can push outside of the uterus into the pelvis. Subserosal fibroids can grow large at times and sometimes have a stalk that attaches to the uterus (pedunculated fibroid).
- Intramural fibroids: These fibroids develop in the muscular wall of the uterus.
- Submucosal fibroids: These fibroids are uncommon. They can grow into the open space inside the uterus and may also include a stalk.
What causes fibroids?
The cause of uterine fibroids is not known, although studies demonstrate there may be a genetic component. There is no definite external exposure that a woman can have that causes her to develop fibroids.
Who is at risk for uterine fibroids?
Various factors can increase the risk of developing fibroids:
- Age: Fibroids become more common as women age, especially during their 30s and 40s and up to menopause. After menopause, fibroids are much less likely to form and usually shrink if they’re present.
- Family history: Having a family member with fibroids increases your risk. If a woman's mother had fibroids, her risk of having them is about three times higher than average.
- Ethnic origin: African-American women are more likely to develop fibroids than other ethnicities .
- Obesity: Women who are overweight are at higher risk for fibroids. For very heavy women, the risk is two to three times greater than average.
What are the symptoms of uterine fibroids?
Most women with fibroids will experience no symptoms at all. However, large or numerous fibroids can cause the following symptoms:
- Heavy or prolonged periods
- Bleeding between periods
- Pelvic pain and pressure
- Frequent urination
- Low back pain
- Pain during intercourse
- Difficulty getting pregnant
How are uterine fibroids diagnosed?
Fibroids are most often found during a physical exam. Your health care provider may feel a firm, irregular (often painless) lump during an abdominal or pelvic exam.
Scans can confirm a diagnosis. These tests are the two main options:
- Ultrasound: Ultrasound is the most commonly used scan for fibroids. It uses sound waves to diagnose fibroids and involves frequencies (pitch) much higher than what you can hear. A doctor or technician places an ultrasound probe on the abdomen or inside the vagina to help scan the uterus and ovaries. It is quick, simple and generally accurate. However, it relies on the experience and skill of the doctor or technician to produce good results. Other tests such as MRI may be better for other conditions, such as adenomyosis.
- MRI: This imaging test uses magnets and radio waves to produce images. It allows your provider to gain a road map of the size, number and location of the fibroids. We can also distinguish between fibroids and adenomyosis, which sometimes gets misdiagnosed. We use MRI to confirm a diagnosis and help determine which treatments are best for you. MRI may also provide a better option for related conditions such as adenomyosis.
Other tests for uterine fibroids
In special circumstances or if doctors can’t identify the source of your pain, you may need additional testing:
- Hysterosalpingogram (HSG): Doctors typically use an HSG for women having trouble getting pregnant. It checks the inside of the uterus (uterine cavity) and fallopian tubes. After a doctor places a catheter (small tube) in the uterus, the doctor slowly injects a special dye for contrast and takes X-rays.
- Hysterosonogram: Doctors use a hysterosonogram to see the inside of the uterus. After they place a small catheter inside the uterus, they inject water while taking a series of ultrasound images. The test can confirm the presence of uterine polyps or intracavitary fibroids that can cause heavy bleeding.
- Laparoscopy: For laparoscopy, a doctor makes tiny incisions in or near the navel. The doctor then inserts a long, thin instrument (laparoscope) into the abdomen and pelvis. The laparoscope has a bright light and a camera. It allows your doctor to see the uterus and surrounding structures. The view can help your doctor determine if you have a condition such as endometriosis, which can cause pelvic pain.
- Hysteroscopy: For suspected abnormalities inside the uterus, a doctor uses a long, thin instrument with a camera and light. The doctor passes the instrument through the vagina and cervix into the uterus. No incision is needed. The doctor can look for fibroids or endometrial polyps within the cavity of the uterus with this approach. Your doctor may also remove some types of fibroids during this procedure.
How are uterine fibroids treated?
Since most fibroids stop growing and may even shrink as women approach menopause, your doctor might initially recommend observation. However, some fibroids might require more active treatment, depending on:
- Extent of symptoms
- Your age
- Your fertility goals
- Number and size of the fibroids
- Any previous fibroids treatments
- Other health conditions present
Learn more about fibroid treatment.
What are the complications of uterine fibroids?
It is uncommon for fibroids to cause severe health consequences. However, women can have heavy bleeding that can lead to dangerous anemia, or lack of red blood cells.
Rarely, large fibroids can press on the bladder and the channel (ureter) that sends urine there from the kidney. This pressure can lead to kidney damage. Other complications include infertility and repeated pregnancy loss.