It’s a part of the annual physical most men dread. But as unpleasant as it may be, the prostate examination is essential: Cancer of the walnut-size gland is one of the most prevalent forms of the disease, killing nearly 35,000 men in the United States each year.
Radiation therapy is an effective, standard of care option for prostate cancer both as an initial treatment and for recurrence after surgery. However, the treatment has historically involved a long course, with a standard regimen often requiring low doses per day over as many as 45 visits.
Though radiation therapy is considered safe overall, there is always a small chance of significant urinary or bowel side effects after radiation. These risks are thought to be related to technical nuances – the prostate is a moving target that can be difficult to see clearly with standard, X-ray-based imaging. There also are biological factors – whether a patient is sensitive to radiation.

Now, Amar U. Kishan, MD, and a team of his UCLA Health colleagues, are conducting clinical trials on a more effective and less burdensome treatment that uses genetics and advanced technology to determine if a patient can be cured with large doses of radiation given in short sequences, even for patients with recurrences after surgery.
So far the results of this precision medicine approach have been positive.
“We've learned that prostate cancer responds very well to a higher daily dose radiation delivered precisely and with expertise,” said Dr. Kishan, chief of genitourinary oncology and vice chair of clinical and translational research in the Department of Radiation Oncology at the David Geffen School of Medicine at UCLA and the UCLA Jonsson Comprehensive Cancer Center.
“There have been a lot of technological revolutions within radiation that will help us make the treatments safer and more effective,” he said. “There are many patients that can be cured by radiation, and there are many patients who might be meaningfully helped by radiation.”
Optimism about the efforts comes out of the SCIMITAR and GARUDA clinical trials.
"We're trying to push the envelope a little bit and innovate and use our sophisticated technologies to deliver more convenient, cost-effective and potentially better care for our patients," Dr. Kishan said.
In the SCIMITAR trial, Dr. Kishan is studying a high-dose targeted procedure — condensed to five treatments over two weeks — called SBRT, or stereotactic body radiotherapy. Dr. Kishan said 100 patients have been treated as part of the SCIMITAR clinical trial, which started in 2018 and completed enrollment earlier this year.
Regarding the results of the SCIMITAR trial, he said, “I don't want to overstep and make any claims that are inappropriate, because we just are finishing it, but I can say that clearly we're pleased enough with our results that we want to immediately open up the follow-up trial.”
The UCLA Health research team is planning to launch the follow-up EXCALIBUR study before summer to include more than 100 new participants. Dr. Kishan is encouraging men with a rising PSA (prostate-specific antigen) count after prostate cancer surgery to contact Radiation Oncology if they are interested in participating.
The studies build on previous UCLA Health research showing that the majority of participants who underwent the high-dose treatment for low- and intermediate-risk prostate cancer were still disease free seven years later.
Dr. Kishan and his team decided to expand their research through the SCIMITAR trial to see if a shorter course of radiation treatment would benefit men with aggressive prostate cancer. Generally, the course of radiation treatment for prostate cancer requires eight to nine weeks of daily sessions.
“It can be quite long,” he said. “Imagine if you're a working person, or even if you're not a working individual, you have other responsibilities, other things to do.”
That could explain why radiation treatment for prostate cancer patients is generally underutilized in the United States, Dr. Kishan said.
“Patients are not referred for radiation or they're not interested in radiation or they're scared of the radiation. All kinds of reasons exist for that,” he said. “But even if they get a chance to hear about radiation, the length of the treatment course can disincentivize a lot of men. Overall, the underutilization is a big problem, because radiation is a major curative treatment in someone that has a rising PSA after surgery.”
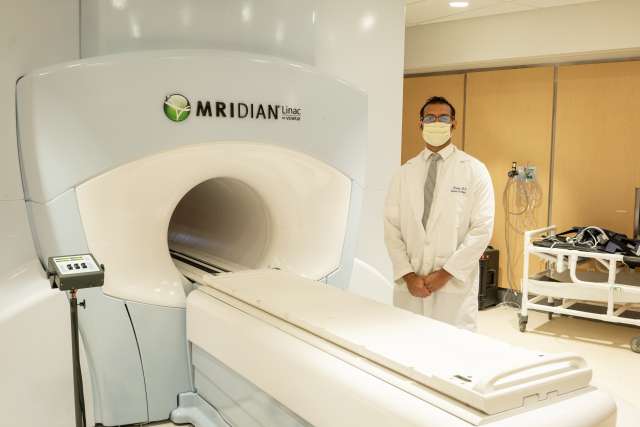
One of the machines researchers are using is the MRIdian Linac, which has a built-in MRI to guide radiation treatment. UCLA Health is one of the few health systems in the country with this machine, which also is being used in clinical studies for treating pancreatic cancer and sarcomas.
For study participant John Babcock, who first was diagnosed with prostate cancer in 2004 at age 52, the intensive treatment at UCLA Health has given him hope.
Babcock’s PSA had been rising for years after his initial surgery. UCLA Health was not Babcock’s first stop for care, however, due to insurance contracting. Doctors at another health system told him he could not be cured and he would have to be on hormone therapy indefinitely. This caused problems, including “man-opause,” with hot flashes, Babcock said.
Babcock came to UCLA Health after a change in insurance and was referred to Dr. Kishan to discuss SCIMITAR. He was able to stop hormonal therapy and receive radiation.

“It’s been a little over a year now and my PSA is barely measurable,” Babcock said. “Dr. Kishan’s work and advanced research provided relief where there had been no hope before. His brilliant work is certainly going to help a great number of people. I am just one example.”
Another paradigm-changing study that Dr. Kishan and the UCLA Health research team is running is the GARUDA trial, in which men who are going to receive radiation as their only treatment for prostate cancer are checked in advance for whether they might be sensitive to radiation (specifically, SBRT).
Patient Hiram McCall, 68, was one of the first patients enrolled in this study. He praised UCLA’s effort as “far more evolved.” Treatment doesn't compare with what it was like even 30 years ago, he says, noting the seemingly non-personalized nature of some standard treatments.
McCall was one of the rare patients found to be more sensitive to radiation, so his treatment plan was altered, and he is doing well, with minimal side effects after radiation therapy.
“Any patient who is a candidate for SBRT for their prostate cancer is a candidate for the GARUDA study,” Dr. Kishan said. “It just involves a quick cheek swab, and we run our tests in our lab with results back in 10 days or so. This allows us to tailor our radiation technique to the specific biology of the patient we are treating, in terms of risk of side effects.”
Dr. Kishan cautioned it will be another two years before the first major report on the UCLA Health studies is complete. But he believes it will underscore that prostate cancer is “highly curable” for a majority of patients.
“A major focus should be how can we cure their cancer while maintaining their quality of life, because one of the things that can happen with prostate cancer treatments is impacting various aspects of a man's quality of life,” Dr. Kishan said.
“So my hope is that we will continuously make prostate cancer treatments more widely available and accessible to patients, and a big part of that is making them shorter,” he said. “And I hope we can get to a point where we can tailor the type of radiation to whether a man is intrinsically sensitive to radiation or not.”
Learn more about Radiation Oncology services at UCLA Health.
Tina Daunt is the author of this article.




