Some two-dozen antiseizure drugs are now on the market to treat epilepsy, but it is estimated that one-third of the more than 3 million adults in the United States with the disorder continue to experience seizures despite being on medication. This is called medication-resistant epilepsy. Living with even occasional seizures has a substantial impact on quality of life, both from the seizure risk and the potential for cognitive impairment and sudden death from epilepsy, says John Stern, MD, codirector of the UCLA Seizure Disorder Center. Many patients also experience debilitating medication side effects, as well as comorbidities, such as depression and suicidality.
Dr. Stern and center codirector Dawn Eliashiv, MD, recommend that any patient who isn’t seizure-free after one or two medication treatments be referred to a specialized center of excellence, such as UCLA. But studies have found that many patients with uncontrolled epilepsy haven’t seen appropriate specialists. Among the reasons, Dr. Eliashiv notes, is the misconception that specialized centers are only for patients who need surgery. “Many patients fear surgery, and that has served as a barrier for physicians in referring to a comprehensive epilepsy center for evaluation, even though we offer much more than that,” Dr. Eliashiv says.
Often, major interventions aren’t required to improve a patient’s condition. “Sometimes a new medication is all a person needs,”Dr. Stern says. “But we find that many patients worry about experiencing side effects from the change, so they become stuck in their current, inadequate regimen.”
Determining the best course of treatment for each patient starts with a thorough evaluation to pinpoint the diagnosis — a process that generally involves some combination of MRI, PET, EEG and, most important, the workup and history-taking of subspecialized clinicians. Dr. Stern points out that in as many as one-third of patients, such an evaluation may reveal that a patient’s seizures aren’t epileptic, but rather the result of another condition that mimics epilepsy and calls for a treatment other than antiseizure drugs. For patients with epilepsy, a subspecialist with intimate knowledge of the many medications and their side effects can successfully guide the patient to the ideal medical regimen.
For patients found to have medicationresistant epilepsy, the best hope for stopping the disabling seizures is to surgically remove the portion of the brain that is causing them. “Resective surgery is the gold standard in terms of giving people with epilepsy a chance for total seizure freedom, with minimal or no side effects,” says neurosurgeon Ausaf Bari, MD, PhD. But Dr. Bari explains that, while more patients are surgical candidates than in the past, the majority still are not — in many cases because their seizures originate from areas of the brain that serve critical functions.
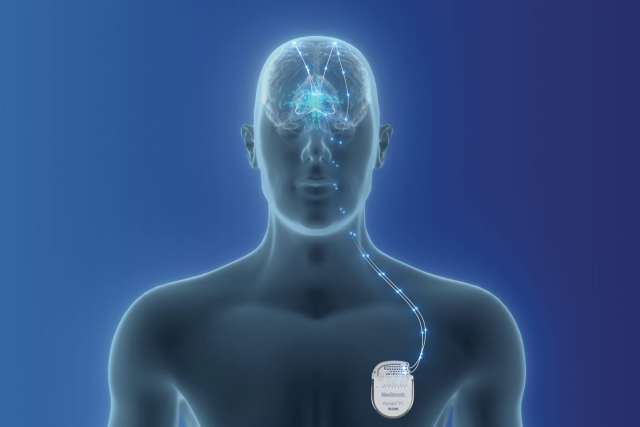
For these patients, the UCLA Seizure Disorders Center offers three modalities of neurostimulation, which can reduce seizure risk in a manner that is both less invasive and reversible. In deep-brain stimulation (DBS), which has been used effectively for patients with movement disorders such as Parkinson’s disease for two decades, the neurosurgeon makes dime-size openings in the skull to place electrodes on either side of the brain that receive continuous electrical signals from a battery-operated device implanted under the collarbone to disrupt abnormal brain rhythms responsible for the seizures. Another procedure, responsive neurostimulation (RNS), uses a device that learns how to read brain signals to detect seizures, then stimulates the brain to abort the activity before it becomes a full-blown seizure. For patients who want to avoid any type of brain procedure, vagus nerve stimulation places an electrode around the nerve in the neck that goes to the brain and indirectly stimulates the brain through a pacemaker-like device implanted in the chest that monitors heart rates as a proxy for seizure activity. In each case, if the modality proves to not be effective or well tolerated, it can be switched off.
Dr. Stern and Dr. Eliashiv stress that patients referred to the UCLA Seizure Disorders Center see a multidisciplinary team of subspecialists who collaborate with the referring physician to develop and implementatreatment plan individualized to the patient’s needs. “We are relentless in going the extra mile for our patients,” Dr. Eliashiv says. “With so many treatment options, it’s important not to give up.”