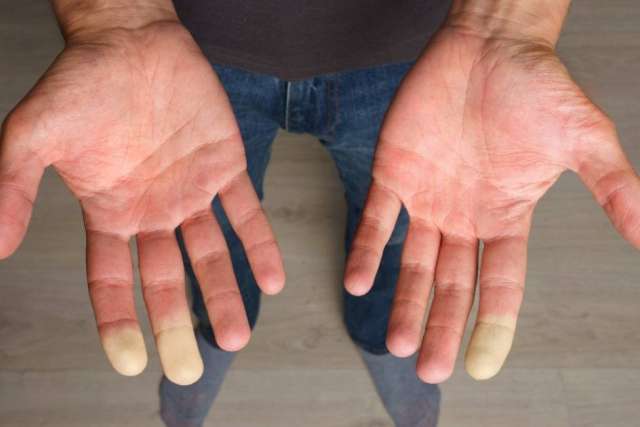
Dear Doctors: While stationed in Alaska more than 35 years ago, I experienced the tips of my fingers turning white in the cold weather. A doctor said it’s probably Raynaud’s syndrome. Does this condition slow down healing? I ask because a deep scratch on my shin still hasn’t healed after four weeks.
Dear Reader: Raynaud’s syndrome, also known as Raynaud’s phenomenon, is a condition in which the small arteries in the extremities suddenly contract and briefly become excessively narrow. This can occur in response to cold or stress. These spasms allow little or no blood to reach the surface of the skin. Raynaud’s phenomenon usually affects the fingers, but it can also involve the toes.
During an episode, the lack of blood flow causes the affected areas to turn white or a blueish purple. It can also cause numbness. When the episode has ended, normal blood flow resumes. This causes the affected skin to turn red and results in a throbbing pins-and-needles sensation. In severe cases, the repeated loss of blood flow can give rise to sores on the fingers or toes. It’s rare, but it can even lead to tissue death.
Raynaud’s phenomenon is estimated to affect 5% to 10% of the population. It is broken down into two categories -- primary and secondary. The primary form is the most common of the two, and is usually less severe. It typically arises between the ages of 15 and 25 and has no known cause.
Secondary Raynaud’s phenomenon is linked to other diseases. These are most often autoimmune or connective tissue diseases, such as lupus, scleroderma and rheumatoid arthritis. Thyroid disorders, certain blood disorders and pulmonary hypertension can also play a role. It has also been linked to tissue damage due to repetitive actions, chemical exposure, certain medications and hand or foot injuries.

The condition doesn’t usually cause permanent damage. However, it can be a symptom of an underlying illness. That’s why it’s important for someone with Raynaud’s phenomenon to see a doctor for tests. Microscopic examination of the blood vessels beneath the skin, known as nailfold capillaroscopy, can differentiate between primary and secondary Raynaud’s. If the diagnosis is primary Raynaud’s, the individual will be advised on how to limit episodes and how to care for the affected areas when they occur. When the diagnosis is secondary Raynaud’s, the next step is additional testing to identify the underlying disease or condition.
It’s possible for Raynaud’s phenomenon to interfere with healing time in a skin injury, but this is associated with severe disease. Additionally, it would affect areas of reduced blood flow. That would be unlikely to include the shin, where the scratch you are concerned about is located. But some of the underlying diseases involved in secondary Raynaud’s can have an effect on healing.
It sounds as though you have not yet had a definitive Raynaud’s diagnosis. We urge you to see your doctor. Whether it turns out to be primary or secondary Raynaud’s, they will be able to provide you with useful information and supportive care and help you determine the cause of your slow-healing scratch.
(Send your questions to [email protected], or write: Ask the Doctors, c/o UCLA Health Sciences Media Relations, 10960 Wilshire Blvd., Suite 1955, Los Angeles, CA, 90024. Owing to the volume of mail, personal replies cannot be provided.)