In a research article published today in the journal Science, UCLA researchers have found that fibroblasts – scar-forming cells that reside in the scar tissue of an injured heart -- directly play a role in promoting a disturbance of the heart rhythm, otherwise known as an arrhythmia. This finding holds promise for novel approaches to life threatening rhythm problems of the heart.
Every year in the U.S., sudden cardiac death kills upwards of 350,000 people who have had no previous symptoms of heart disease, and in the majority of cases, the underlying cause is an arrhythmia. While there is a strong association between the amount of scar tissue in the heart and the likelihood of an arrhythmia to occur, whether fibroblasts in scar tissue directly communicated with cardiac muscle cells to promote arrhythmias was not known.
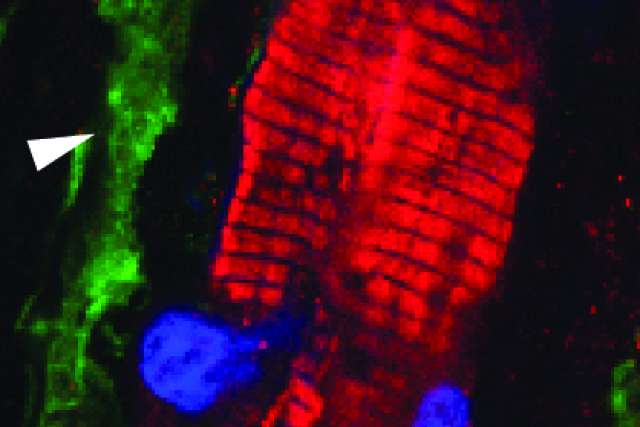
In cardiac scar tissue, cardiac muscle cells are surrounded by cardiac fibroblasts and often come in close contact with cardiac fibroblasts. "For decades, scientists have wondered whether the cardiac fibroblasts are electrically passive and just form scar tissue or whether by coming in close contact with myocytes, they directly increased the excitability of cardiac muscle cells and promoted life threatening arrhythmias in vivo," said Dr. Arjun Deb, senior author, professor of medicine and director of the UCLA Cardiovascular Theme, at the David Geffen School of Medicine.
A new study, led by Yijie Wang, a postdoctoral fellow in Dr. Deb’s lab, demonstrates that cardiac fibroblasts within scar tissue robustly communicate with cardiac muscle cells to promote electrical excitability and generate arrhythmias.
The researchers genetically engineered only the fibroblasts in the heart of a mouse to express a light sensitive ion channel (also known as optogenetic channel) that led to fibroblasts being electrically excited upon exposure to a flashing light. The researchers flashed light upon scar tissue in the heart and observed that the heart rate and rhythm could be controlled by the frequency of illumination of scar tissue. A substantial fraction of animals immediately developed life threatening rhythm disturbances after the illumination of scar tissue was stopped.
“The results are striking and suggest that fibroblasts play a much bigger and more direct role in regulating cardiac conduction than we previously appreciated,” said Dr. Deb, who is also a professor of molecular cell and developmental biology and a member of the UCLA Broad Stem Cell Research Center.
The research team also identified new mechanisms of fibroblast-myocyte communication. The team found that proteins called connexins that have been previously thought to attach fibroblasts to myocytes were dispensable for fibroblast-myocyte communication, but rather the electrical field generated by the fibroblast excited the myocyte to generate the arrhythmia.
The study has clinical implications. The current therapy to treat a scar tissue related arrhythmias is cardiac ablation, which destroys myocytes in the scar tissue area to homogenize the scar and decrease excitability of the scar tissue. Ablation is highly effective but 50% of patients have a recurrence within a year. Dr. Deb says ablation by destroying myocytes within scar increases fibroblast numbers and fibrosis and their work suggests that new foci of fibroblast-myocyte communication could potentially result in new arrhythmias.
The researchers’ next steps are to further understand how fibroblasts and myocytes communicate and to develop therapeutic strategies to target this mechanism for future therapies for sudden cardiac death. Dr. Deb also says these findings could be broadly applicable to the nervous system as well where similar questions about the direct effect of non-excitable cells on excitability of neurons remain unanswered.
"This was a team science effort" says Dr. Deb. Dr. Bennett Novitch, Matteo Pellegrini, Zhilin Qu, Riccardo Olcese from UCLA and Dr. Zhen Song (Peng Cheng Lab, China) and Dr. Feiyang Ma (Northwestern University) were faculty collaborators, and along with their trainees, are co-authors on the paper.
Article: Fibroblasts in heart scar tissue directly regulate cardiac excitability and arrhythmogenesis. DOI 10.1126/science.adh9925