Photos by Nick Carranza, Milo Mitchell and Joshua Sudock
Have you ever donated blood only to wonder where it went and who it went to? We’ve all heard the phrase “donating saves lives,” but we rarely know who has survived as a result of this generous donation. To convey the urgency and lifesaving power of a blood donation, below is a photo essay that gives a glimpse into all the stops of a blood unit, the people who help along the way, and Leanna Lopez, a 7-year-old girl with anemia.
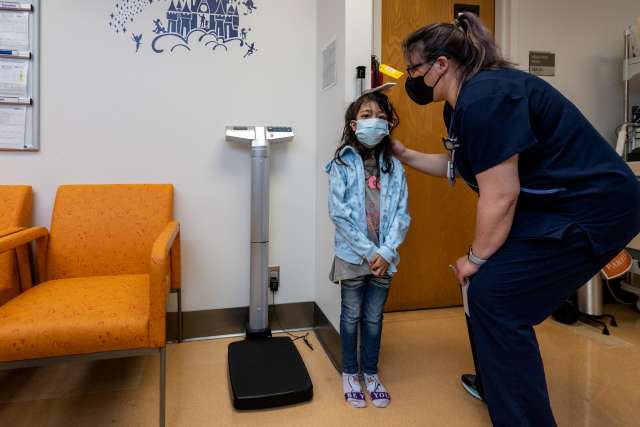
Leanna Lopez has congenital dyserythropoietic anemia, a rare blood disorder in which the body cannot produce red blood cells effectively, thereby preventing blood from carrying oxygen throughout the body. She requires a unit of type O+ blood for transfusion every three weeks.
Site 1: Blood & Platelet Center

The beginning of the many stops of a blood unit traveling from a donor’s arm to a patient involves the telerecruiting office at the Blood & Platelet Center. Telerecruiter Melanie Capetillo calls previous blood donors to schedule an appointment.

One of those donors includes Ingrid Bermeo, an O+ blood donor who has been regularly giving blood since 2003. “I have been a longtime donor because my blood can be transfused to any patient with a positive blood type, around 80% of the population,” Bermeo said. Only 3% of age-eligible people donate blood every year, according to the American Red Cross, so there’s an endless need for blood donors.

Here, she checks in with hospital lab technician Gregory Domond, fills out a donor history questionnaire (DHQ), and reviews the donor educational material for her appointment. The DHQ ask questions such as whether Bermeo is feeling healthy and well, whether she is currently taking medication and whether she’s donated blood in the past eight weeks.

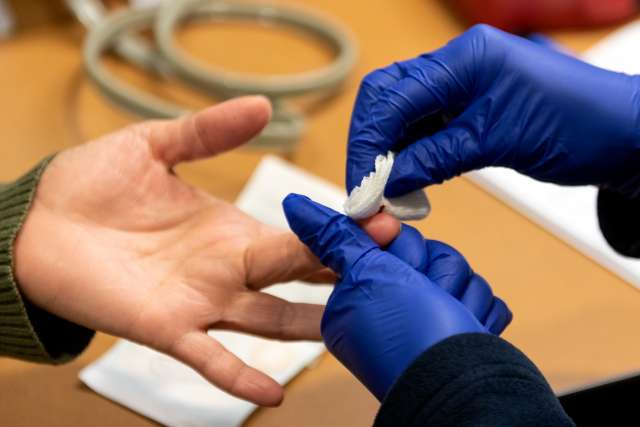
Katherine Ramirez, a hospital lab technician, covers Bermeo’s finger after a routine finger prick screening that measures hemoglobin levels. Ramirez also measures Bermeo’s vital signs. These screenings are in place to ensure a donor can safely give blood, and to ensure a recipient is receiving safe, pure and potent blood.
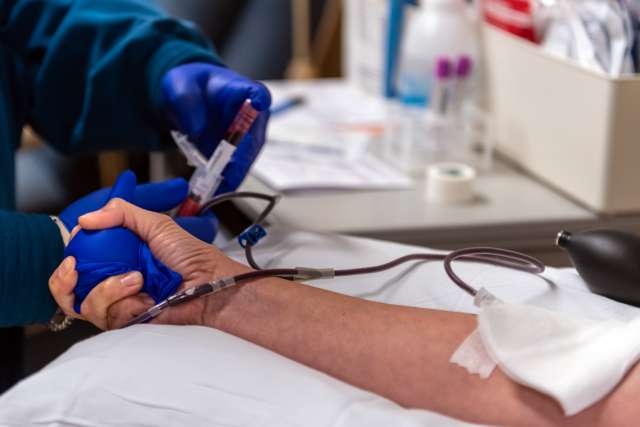
Bermeo is eligible to donate. Hospital lab technician Danny Perez has disinfected Bermeo’s arm, inserted a needle and collected about a pint of blood for approximately 10 minutes. A few extra tubes are sent to a laboratory to be tested for infectious diseases.
Perez then labels, scans and stores Bermeo’s blood unit and the test tubes in insulated boxes to maintain blood quality.

While Perez labels Bermeo’s blood unit, the donor waits in the Blood & Platelet Center for 15 minutes after giving blood as a safety precaution. The center thanks donors, and builds up their strength, with snacks and coffee.

Courier Jose Zapata picks up blood units, including Bermeo’s, and drives the boxes to the component processing lab at the Center for Health Sciences building.

Site 2: Components Processing Lab


Once the courier delivers the boxes to the Components Processing Lab, Steven Zuniga, a hospital lab technician, unpacks the units and stores Bermeo’s unit in a refrigerator.
Hospital lab technician Jamie Baldoza begins the first processing step in the lab: leukoreduction. This step removes white blood cells from Bermeo’s blood unit, which decreases the risk of an adverse reaction once the blood is transfused to Leanna.


Baldoza places Bermeo’s blood unit into a centrifuge, which spins and separates the blood unit into red blood cells and plasma.


The Components Processing Lab also sends the tubes of blood to an off-site testing center to undergo infectious diseases testing and ABO blood-typing. A blood type is determined by identifying the antigen on the red blood cell. A second test determines whether a protein called Rh is present or absent from the red blood cells. The blood type is labeled as either O+, O-, A+, A-, B+, B-, AB+ or AB-.
The blood unit remains in quarantine in the Components Processing Lab until the blood type is determined and the infectious diseases test results are received.

Sites 3 & 4: Pediatric Infusion Center Blood Bank at Ronald Reagan UCLA Medical Center


Bermeo’s blood unit then gets delivered from the Components Processing Lab to the blood bank at the Ronald Reagan UCLA Medical Center. Teddy Salle, a hospital lab technician, unpacks the daily delivery from the Components Processing Lab.
Before Bermeo’s blood unit is transfused to Leanna, it undergoes a second blood typing test and is also tested for whether certain antibodies are present to determine blood compatibility. Bermeo is type O+, matching Lopez’s blood type. It’s crucial that the donor and recipient have compatible blood, otherwise, the body’s immune system may fight off the donated blood. O- is the universal blood type, meaning any recipient can receive this blood donation.


Meanwhile, Leanna checks in at the Pediatric Infusion Center next door after a long drive from Lancaster. Millicent Ongaco, a Child Life Specialist, plays games with Leanna prior to her blood transfusion. “Making Leanna feel safe during a stressful time brings me so much joy,” Ongaco said.

While Salle tests Bermeo’s blood unit in the blood bank laboratory, Diane Kui, Leanna’s nurse, takes samples of Leanna’s blood to crossmatch with Bermeo’s blood unit.

Back at the blood bank, Leticia Alvarez, a hospital lab technician, receives a type O+ blood request for Leanna. Alvarez doesn’t work directly with the young patient, but she is grateful to have an impact. “I believe in treating each patient request for blood products as if it was for a family member and will often say little prayers for them to myself,” Alvarez said.

Before Leanna receives a transfusion, Andrew Cottrell, a clinical laboratory scientist, performs a crossmatch test. This transfusion trial involves mixing a sample of the blood from donor and recipient to ensure they are compatible.

The issue bench is the last stop in the blood bank. Dabby Aquino, a clinical laboratory scientist, looks at Bermeo’s history and checks if the patient requires special modifications to their blood unit. After Aquino completes these tasks, she sends her unit to the Pediatric Infusion Center through a pneumatic tube system.

Prior to the transfusion, Leanna is given Desferal, a medicine that removes excess iron from the body. After Kui checks Bermeo’s blood unit delivered from the blood bank, Leanna is ready to receive the donation, a transfusion that will last four hours.

After the transfusion, Leanna is ready to go back home. Her spirit and health are a testament to how the gracious act of donating blood can save a life.


