New Inpatient Dialysis Starts Program (NIDS)
Advancing the current state of patient care by innovative practices and programs.
End Stage Renal/Kidney Disease (ESRD/ESKD) is a major driver of morbidity, mortality and healthcare costs in the United States. To this effect, in 2019, the President passed the Executive Order which was implemented as the Kidney Health Initiative.
The three main goals of the Kidney Health Initiative are:
- To slow down the progression of kidney disease so we have fewer patients ending up with need of dialysis or transplantation.
- Patients who did advance to the state that they need dialysis or transplant, they would end up on home dialysis rather than what we call in-center hemodialysis.
- Increase rate of transplantation in patients with advanced kidney disease.
One in three patients ending up on dialysis in the United States have never seen a kidney specialist. These are staggering facts if you think about it. The first 90 days in the life of a patient on dialysis is extremely critical and is associated with the highest morbidity and mortality as well as financial cost. There is an epidemic of kidney disease in the United States with one in seven US adults suffering from kidney disease and it is projected to only get worse with time with increasing rates of obesity, diabetes, and an aging population.
Impact
The CORE Kidney goal is to advance healthcare by implementing its CORE values of Clinical Excellence, Outreach, Research and Education. Our hope is that we can make our patients their own best advocates. The program is truly integrative with various specialists working together with one goal: to get our patients the best care that they can. We have made significant improvements in the outcomes of our patients especially with ESRD and have made significant progress towards the three goals set by the kidney health initiative.
We have slowed down the progression of kidney disease in our patients by early diagnosis, implementing best practices and clinical research. For the patients who do advance to ESRD, the proportion of our patients on home dialysis is 55% compared to the national average of only 10%. We also have a very significantly higher rate of transplantation with a major focus on living kidney donation.

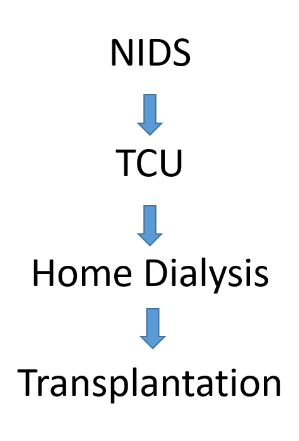
We have initiated a very novel program called the NIDS Program. NIDS stands for New Inpatient Dialysis Starts. As the name suggests, this program focuses on patients who start dialysis in the hospital. Most of these patients are crashers and might not have had pre-dialysis care (as previously mentioned, one in three patients ending up on dialysis have never seen a kidney specialist). These patients tend to have one of the worst outcomes even among dialysis patients. The NIDS program has been specifically designed to address this problem. It is based out of the hospital with a multidisciplinary team (nephrologists, surgeons, interventional nephrologists, nurses, social workers, dietitians among others) that work together. These patients are eventually transferred to Transitional Care Unit (TCU) at our outpatient dialysis units located in Century City and Brentwood. From the TCU, our goal is to transition them to HOME Dialysis with that acting as a bridge for eventual transplantation.
Educating the patient is a major part of the process and our trainees including clinical fellows are heavily involved in this. This is very novel with nothing similar to this in the country. This has had a major positive impact on patient care and outcomes.
These are tough times and there is no better place than to be at home for our especially vulnerable patients during the pandemic. Besides being on dialysis, most of them have significant other comorbid conditions including diabetes and cardiovascular disease placing them at increased risk. Our goal is to transition as many as we can to home dialysis and transplantation. We have made significant progress at our goal of providing truly comprehensive integrative care for our patients with ESRD.