Fellowship
Introduction
The UCLA Rheumatology Training Program is one of the largest in the United States with outstanding clinical, basic science, and translational researchers that manage some of most prevalent/complex rheumatic diseases while supporting cutting edge therapeutics to improve patient care and identify potential cures. It is an integral component of the largest health care system in Southern California.
All applications to the program are through ERAS, the Electronic Residency Application Service
Fellowship Coordinator: Gabriel Valdivia
Phone: 310-825-7992
Email: [email protected]
Program Director: Dr. Jennifer Grossman, MD
Program Description
A. Goals of the Training Program and Success in Achieving Those Goals
The goal of the UCLA program is to produce bench scientists, clinical investigators/educators, and practicing clinicians. In the past 5 years, there are 23 trainees who have completed the ACGME-certified training program. Of these 23 graduated trainees, 3 have received advanced degrees other than their MD and 3 have additional Board certification (2 Dermatology, 1 Geriatrics). Nine are pursuing careers in bench and/or clinical investigation, 1 is pursuing a career as a clinical / health service investigator, and 13 are practicing clinicians. Ten are in full-time academic positions. These trainees have produced 70 submissions during their fellowship or recently thereafter; 44 peer-reviewed articles, 9 reviews, 1 chapter, and 16 abstracts (published, in press/submitted) with faculty mentors. None of these numbers include numerous presentations at various meetings.
Metrics for success of our rheumatology fellowship program include:
- Number of participants completing an advanced degree
- Clinical excellence
- Number of publications during and after matriculation
- Quality/importance of the acquired new knowledge in the field
- Independent funding: The number and level of competitive peer-reviewed awards
- Success as a subsequent mentor
- Scores on in-service exams
- Scores on Board Certification exams
Of the 23 fellow graduates from the last five years, 8 have joined our faculty. In prior years, trainees (year two or year three) have had support from a variety of sources including:
- UCLA Immunology NIH T32.
- UCLA STAR Program (MS or PhD).
- National Arthritis Foundation / ACR individual awards – Physician Scientist, Postdoctoral Fellowship, Physician Scientist Development Award, ACR Lupus Investigator Fellowship Award, ACR-REF/RRF Clinical Investigator Award.
- ACR-REF/RRF Fellowship Training Award (UCLA has received this grant each year it has been offered).
- ASP Junior Career Development Award in Geriatric Medicine.
- Meyer Award of the Arthritis Foundation, Southern California Chapter.
- NIH K23 Development Award.
- Southern California Scleroderma Foundation Fellowship Award.
- Private Foundation non-recurring support for 1 or 2 years of training (e.g. Mitchell Foundation SLE Fellow).
- Biotech/Pharma fellowship resources.
B. Description of Curriculum
Didactic Program
The UCLA Rheumatology Fellowship Training Program is university affiliated and accredited by the ACGME. The training program has 42 faculty that include 8 emeritus faculty (Roy Altman, Pojen Chen, Philip Clements, Daniel Furst, Bevra Hahn, James Louie, Harold Paulus, David Yu) in Rheumatology. This includes 32 with MDs, 6 with MD+MS, 4 with MD+PhD or PhD. Of the MDs, all but 2 have some level of clinical teaching and patient care responsibilities.
The training program has 4 training sites:
Site 1) Ronald Reagan UCLA Medical Center
Site 2) UCLA Santa Monica Medical Center, a community hospital setting
Site 3) VA Greater Los Angeles Healthcare
Site 4) Harbor-UCLA County Hospital
The 4 sites offer our rheumatology fellows exposure to broad clinical, socioeconomic and cultural experiences. In addition to the diverse patient and research opportunities for the fellows, our Division of Rheumatology includes 7 Masters of the ACR, a Gold Medal recipient of the ACR (only 1 /year awarded), a past ACR President, and multiple editorships of major rheumatology textbooks and journals.
As part of the ACGME CORE curriculum, our rheumatology fellows present bi-monthly in journal clubs and case presentations to develop skills in review of evidence based information and review up-to-date medical literature. Fellows develop teaching skills through clinical rotations in the 4 training sites with medical residents and medical students. Fellows also lead our immunology lecture series in which each fellow is paired with a bench/clinical faculty member to present fundamentals as well as up-to-date immunology concepts and how they affect new and upcoming rheumatology therapies.
As part of our program, we have several additional teaching conferences for the fellows. These include Rheumatology Grand Rounds, Medicine Grand Rounds, joint Rheumatology-Radiology conference (fellows present cases to UCLA radiology faculty), Immunology Forum, Translational Research Conference in Autoimmunity, and ACR rheumatology slide review (led monthly by Dr. Roy Altman). Fellows also attend the Carl Pearson Symposium (organized by Drs. Daniel Furst, Philip Clements, and Harold Paulus in our program) as well as the national ACR annual scientific meeting and ACR SOTA meeting.
The UCLA Specialty Training and Advanced Research (STAR) program is also an excellent resource that the Rheumatology Training Program has used for advanced training / credentialing. Fellows have more flexibility with their clinical months while they obtain an advanced degree so critical to academic success (Masters in Clinical Research or a PhD in bench, translational, health services research). New this year is a post-doctoral 3-year STAR program for fellows that already have a PhD.
Patient Population
One of the strengths of the UCLA program is the diversity of patients seen at our multiple training sites. All fellows rotate through each venue. UCLA Reagan Medical Center and Santa Monica UCLA serve patients typically with 3rd party payers, including MediCal (MediCaid in other states) and MediCare. UCLA Reagan is a tertiary medical center where Fellows provide consults on complex co-morbid diseases such as vasculitis and transplant patients. Santa Monica UCLA is a community hospital and Fellows during their rotations there see "bread and butter" rheumatology. The VA population has a unique group of patients, predominantly male, enriched with spondyloarthropathies, microcrystalline arthropathies, and vasculitis. It also has a complete HMO-like structure with all services including pharmacy and rehabilitation and consultations provided on site at no or low cost. Harbor UCLA is a Los Angeles County hospital that serves an indigent population with a high prevalence of infectious rheumatic diseases and autoimmune diseases that strike individuals of minority groups and low socioeconomic groups, often with devastating outcomes. Depending on their specific rotation, the Fellows work in outpatient clinics twice a week at the VA, three times a week at Harbor, once a week at UCLA Reagan Medical Center, and 4 days a week at Santa Monica UCLA. In addition, Rheumatology clinics are open every day at UCLA Reagan Medical Center and at Santa Monica UCLA, where the fellow on rotations at those institutions can accommodate urgent cases that need to be seen on the same day. The fellows also have outpatient clinic blocks in which they rotate through pediatric rheumatology, physical medicine and rehabilitation, podiatry, neuro/EMG, radiology, and sports medicine/orthopedics. The total number of outpatient visits to UCLA Rheumatology for the last academic year was more than 30,000. For the fellows, the number of new outpatient encounters was nearly 4800 and inpatient consults totaled 780.(These fellow statistics do not include follow-up visits). The Fellows have a true continuity clinic, which is held at Reagan UCLA every Friday, where fellows typically have a schedule of 2 new patients and 4 follow-ups on average. They follow those patients throughout their training period. There are other outpatient clinic rotations that include many patients that they have previously seen longitudinally but in the Fellow's Continuity Clinic they are the patient's primary rheumatologist.
Procedures
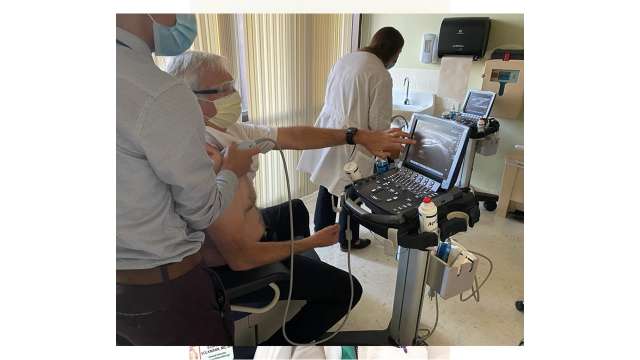
Fellows are exposed to a large number of procedures within Rheumatology as well as in other specialties. All forms of arthrocentesis and soft tissue injections are performed by the Fellows during their rotations with each faculty member. The fellows average at least 120 arthrocentesis.
Our program also has its own rheumatology-dedicated ultrasound equipment in the UCLA-Santa Monica and UCLA-Reagan Outpatient Clinics. Their use is taught didactically in Grand Rounds as well as through practical hands-on experience by our faculty trained in this procedure (Mihaela Taylor, M.D., Veena Ranganath, MD, and John FitzGerald, MD). We have also developed a formal ultrasound course that meets in the evening for 2 hours, 10 times per year. Each session addresses one of 8 anatomical regions, image display/capture, as well as ultrasound-guided arthrocentesis. Fellows also learn orthotics, including bracing techniques, in physiatry/rehabilitation medicine. Another core rotation is the EMG procedures clinic. Fellows can also observe arthroscopies in Sports Medicine/Orthopedic. They can elect time in various Orthopedic clinics (back, knee, hand, foot, shoulder/elbow, hip clinics) during their electives; teaching in each of those clinics is provided by an Orthopedic attending (or PM&R for some patients in back clinic). Muscle, nerve, and skin biopsies are regularly reviewed with the neuropathology and dermatopathology departments, whose members also teach in Rheumatology Grand Rounds.
C. Number of ACGME-Approved Training Slots, Fill Rates
With the current number of fellows our faculty-to-fellow ratio is more than 5:1. We are ACGME approved for 10 fellowship slots (probably the largest program in the U.S.) although the number of fellows in the program can vary depending on participation in our STAR program.
UCLA has always had a 100% fill rate for slots submitted through the Match. All rheumatologists in our program are ABIM certified in rheumatology and all fellow graduates have passed the ABIM in Internal Medicine and Rheumatology on their first attempt.
Additional Information about the UCLA Rheumatology Training Program
Ranked as one of the top 3 hospitals in the 2016 US News & World Reports, the Ronald Reagan UCLA Medical Center offers our fellows interdisciplinary exposures to other top sub-specialties at our institution, including intensive care and organ/bone marrow/stem cell transplant programs. Our program's lead rheumatology training site (Reagan UCLA) is also ranked by US News & World Reports in the top handful of training programs and has always been ranked "Best in the West". We offer fellows research experiences in clinical, health services, and bench investigations. Our faculty are on the cutting edge in areas such as Osteoarthritis (Roy Altman), Lupus (Bevra Hahn, Ram Raj Singh, Jennifer Grossman, Maureen McMahon, Brian Skaggs, Jennifer King, George Karpouzas), Genetics (Ari Weinreb), Rheumatoid Arthritis (Daniel Furst, Harold Paulus, Ernest Brahn, Christina Charles, Veena Ranganath), APS (Pojen Chen), Geriatrics-Rheum (Meika Fang, Veena Ranganath), Vasculitis (Jay Persselin, Tanaz Kermani), Scleroderma (Daniel Furst, Philip Clements, Suzanne Kafaja, Elizabeth Volkmann), Musculoskeletal Ultrasound (Mihaela Taylor, John FitzGerald, Veena Ranganath),Gout (Jay Persselin, John Fitzgerald), and Lupus Quality of Care (Jennifer Grossman).
Our research program includes both clinical and bench investigation in systemic autoimmune and inflammatory diseases. In bench research leadership: Ram Raj Singh studies T cells, NKT cells and dendritic cells in SLE / RA / scleroderma using mouse models and human samples; Bevra Hahn investigates peptide-specific regulatory and inhibitory T cells in mouse models of SLE as well as lipid abnormality biomarkers of atherosclerosis in SLE; Ernest Brahn employs models to explore translational therapeutics in RA / vasculitis; Antonio La Cava studies Treg cells and leptin in SLE; and Pojen Chen evaluates the pathophysiology of anti-phospholipid antibodies. In clinical investigations, leadership includes Daniel Furst (RA and scleroderma), Christina Charles and Veena Ranganath (polymyositis and RA), Philip Clements (scleroderma), and Bevra Hahn /Jennifer Grossman / and Maureen McMahon (SLE). Our unique STAR program allows fellows to simultaneously pursue a masters in clinical research or a PhD in bench/translational/health services research.
The UCLA Rheumatology training program has produced many leaders in rheumatology, including Robert Ashman, Chief, Division of Rheumatology, University of Iowa; Michael Brenner, Chief, Division of Rheumatology, Brigham and Women's Hospital, Harvard School of Medicine; Robert Hoffman, Chief (former), Division of Rheumatology, University of Miami; James Klinenberg, Chief (former), Division of Rheumatology, Cedars Sinai Medical Center; James Louie, Chief (former), Division of Rheumatology, Harbor Medical Center; Paul Bacon, Chief of Rheumatology, University of Birmingham, England; Yeong Song, Head, Department of Rheumatology, Seoul National University, South Korea; Dwight Kono, lupus geneticist, Scripps Research Institute, San Diego; Philip Clements, Professor, UCLA; James Peter, CEO (deceased), Specialty Laboratories; Kenneth Kalunian, Professor, UC San Diego; Harold Paulus, Professor Emeritus in Rheumatology, UCLA; Daniel Furst, Carl Pearson Professor, Division of Rheumatology, UCLA; Ralph Schumacher, Professor, VA Medical Center, Philadelphia; and Dinesh Khanna, Scleroderma Director, U of Michigan. The current faculty include 7 Masters of the ACR (Roy Altman, Philip Clements, James Louie, Daniel Furst, Bevra Hahn, and David Yu) and winners of the ACR young investigator award, mentoring award, and ACR Gold Medal.
Additional Information about Research Program
Another strength of the UCLA training program is diversity in research opportunities afforded by the Rheumatology full-time faculty and the large body of investigators at UCLA. The UCLA campus includes the medical center, medical school and all graduate and undergraduate schools on the same campus.
In addition, we have interdisciplinary training in research settings with pediatric rheumatology, ophthalmology, orthopedics, radiology, pulmonary medicine, dermatology, molecular genetics, geriatrics, molecular immunology, epidemiology, biostatistics, and health services research (including RAND).
UCLA CTSI (Clinical and Translational Science Institute) also offers mentoring, training courses, and workshops in clinical and translational research. This is available for fellows engaged in research in Year 2 or Year 3.