Heart Failure & CHAMP
CHAMP was designed to reduce the deadly risks and consequences of heart disease by improved use of secondary prevention treatments. Through this focused hospital based program, it has been demonstrated that the treatment gap for secondary prevention can be reduced and patient survival after discharge improved. The methods and tools used to implement CHAMP are available on this web site. By applying a similar program in your hospital setting, you can improve the care of your cardiovascular patients and save lives.
This web site describes the design, rationale, and results of CHAMP. It provides all the tools you need to implement a hospital based atherosclerosis treatment program. Included are the UCLA CHAMP Clinical Practice Guideline, UCLA LDL Treatment to Goal Guideline, UCLA Cardiac Preprinted Admission Orders, CHAMP Care Maps, Cardiac Discharge Orders, Patient Tracking Forms, Patient Education Materials, and Key Scientific References. There are downloadable slide sets. Links to other useful web sites are also provided.
A New Way to Improve Patient Care
All the tools you need to start a similar program in your hospital are available on this web site. Applying this program at your hospital will improve treatment rates, reduce the risk of recurrent hospitalization, and save lives
Assess your current treatment intervention rates. If you provide care at one of the 1500 National Registry of Myocardial Infarction Hospitals, this data is already available for your hospital. Regional, Statewide, and National Data from this registry and other data sources demonstrates that significant treatment gaps exist and there is substantial opportunities to improve.
Each time you see one of your patients with atherosclerosis, whether in the hospital or the outpatient office setting, make sure they are receiving each of the four cardiovascular survival medications, unless contraindicated or not tolerated (aspirin, beta blocker, ACE inhibitors, statin) and have achieved LDL < 100 mg/dl and BP target levels.
Take advantage of hospitalization as a "teachable moment". Patients are more likely to follow guidance and be compliant with mediations immediately after they have had an event.
Create a team within your hospital to improve implementation of secondary prevention treatments for atherosclerosis and improve adherence to national guidelines. This team can apply quality improvement measures such as preprinted admission orders, care maps, discharge protocols and monitor your hospitals progress with data monitoring tools. The tools utilized at UCLA for the CHAMP Program are all available for your use from this web site.
Monitor the treatment rates for patients hospitalized with cardiac disease and make sure they are improving.
For further information please contact: Gregg C. Fonarow, M.D.
Background
A number of studies have documented that secondary prevention medical therapies are underutilized in patients with established coronary artery disease receiving standard medical care.
Patients At Risk
Individuals that have presented with coronary heart disease have a risk of recurrent events and death that is 5 to 7 times that of the general population.
According to the AHA, within 6 years after a myocardial infarction, 18% of men and 35% of women will have a recurrent myocardial infarction, 7% of men and 6% of women will experience sudden death, and 22% of men and 46% of women will be disabled with heart failure.
Medical treatments that target the underlying atherosclerosis disease process can markedly lower the risk of recurrent cardiovascular events and death. Clinical trials have demonstrated significant risk reductions with aspirin, beta blockers, ACE inhibitors, and statins in patients with established coronary heart disease. Failure to implement these effective therapies when guided by conventional care has resulted in large numbers of patients at unnecessarily high risk. Over 2.5 million patients are hospitalized each year with coronary heart disease, but the majority do not receive the optimal treatments proven to reduce events and save lives. review of CAD patient treatment rates at the UCLA Medical Center in 1992 and 1993 revealed a significant treatment gap when guided by conventional care.
Program Results
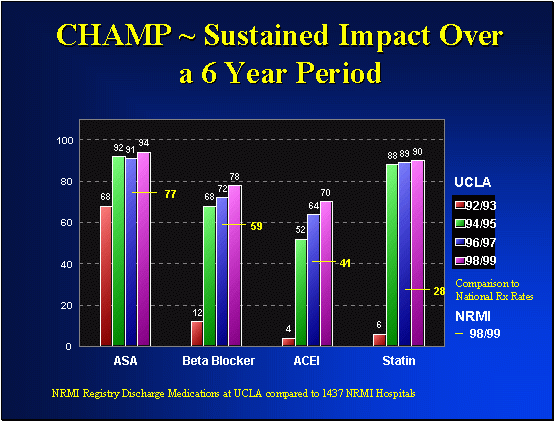
To assess the impact of the program, treatment rates and clinical outcome were compared in patients discharged after myocardial infarction in the 2 year period before (1992-1993) and the 2 year period after (1994-1995) CHAMP was implemented. In the pre and post CHAMP patient groups, aspirin utilization rates at discharge improved from 68% to 92% (p<0.01), beta blocker utilization improved from 12% to 62% (p<0.01), ACE inhibitor utilization from 6% to 58% (p<0.01), and statin utilization from 6% to 86% (p<0.01). These treatment rates at the time of hospital discharge represent among the highest overall treatment rates ever reported.
This increased treatment utilization persisted during subsequent follow-up. At one year, after hospital discharge 91% of patients were on statin treatment. The treatment rates for beta blockers, ACE inhibitors, and aspirin also remained high. The CHAMP study demonstrated for the first time that hospital based initiation of lipid lowering therapy markedly improves patient compliance with treatment. Further evidence of improved treatment was provided in that there was a significant increase in patient achieving an LDL cholesterol < 100 mg/dl (6% vs 58%, p<0.001).

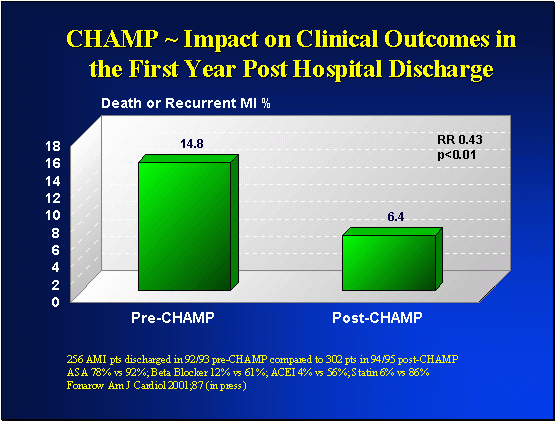
Marked Impact on Clinical Outcomes
The improvement in treatment rates had dramatic impact on clinical outcomes for patients CHAMP was associated with a marked 57% reduction in the risk of recurrent myocardial infarction and mortality in the first year after hospital discharge. There was also a significant reduction in hospitalization. Thus CHAMP reduced health care costs while at the same time saving lives.
Click here to download original article.
Clinical Significance
This study demonstrates that coronary artery disease risk factor modification and treatment can be systematically integrated into the treatment provided during cardiac hospitalizations without additional resources or medical personnel. This approach appears to be considerably more effective than the use of conventional guidelines and care.
Widespread application of CHAMP or other hospital based treatment protocols could dramatically effect coronary artery treatment rates with proven cost effective therapies and thus substantially reduce the risk of future coronary events and prolong life in the large number of patients hospitalized each year with coronary artery disease.
In 1998, 1,263,000 males and 915,000 females diagnosed with coronary heart disease were discharged from hospitals. Increasing the implementation of secondary prevention medical therapies though the use of hospital based programs such as CHAMP would result in tens of thousand of additional lives saved.
There are 5000 acute care hospitals in the United States but only a few have programs in place to ensure cardiac patients are treated with secondary prevention measures.
For more information and to implement CHAMP at your institution please visit http://www.med.ucla.edu/champ/
© Copyright 2001-2004. University of California, Los Angeles
This page last updated on: 12/13/04