COVID-19 Prompts New Guidelines for Stroke Care
Patients should seek early treatment for a suspected stroke, they advise
May 4, 2020: FOR IMMEDIATE RELEASE
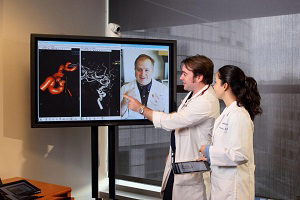
To keep patients and health-care providers safe from COVID-19, while providing urgent treatment to stroke patients, extra precautions must be taken, according to new guidelines published in the journal Stroke.
The guidelines were established by the Society of Vascular & Interventional Neurology (SVIN).
UCLA Professor of Neurology Dr. David Liebeskind, who is President of SVIN and Director of the UCLA Stroke Center, expressed concern that fear of COVID-19 may make patients hesitate to seek treatment in the event of a possible stroke.
“People are passing away or having severe strokes out of the hospital,” he said. “There’s a lot of people who are not coming in.”
Delaying treatment by just 15 minutes can make a world of difference in terms of the patient’s recovery. Yet stroke centers around the country report that they are treating fewer patients than usual. To minimize the possibility of transmitting infections among patients in the hospital, the SVIN team developed guidelines based on review of the published research, consensus among practicing neurologists and shared best practices.

“Some of these things are intuitive or straightforward in terms of minimizing exposure and maximizing the use of personal protective equipment,” said Dr. Liebeskind. Because stroke patients may be unable to communicate and describe their history or symptoms, he said, every patient should be initially considered to be positive for COVID-19.
According to the guidelines, a definitive diagnosis of COVID-19 should be made as soon as possible, as patients who test negative can decrease the use of protective equipment. Patients who test positive should be placed in isolation in a negative pressure room, when available.
Any tests that do not change the treatment strategy should be delayed or deferred until COVID-19 status is established, the guidelines recommend.
The doctors say that telemedicine can play a monumental role in minimizing the number of people who come in direct exposure to the patient. For an acute stroke or thrombectomy code, one person in protective equipment can be with the patient, while another coordinates care via computer or phone.
Remote tele-stroke technology can also be used to obtain history, perform neurological exams and monitor the patient after the stroke has been treated.

“Telemedicine in neurology has evolved over the last 10 years to meet the needs of a consultation,” said Dr. Liebeskind. “In stroke, imaging becomes incredibly important, and that becomes integrated as well. We can do the examination very easily via telemedicine, using a video link at the patient bedside. And, through that same link we can access the imaging information as well. At UCLA, we also have dedicated robots that can travel through the hospital that can do all of this.”
A head CT or computerized tomography scan is typically the first test performed in the event of a stroke. A chest CT can be performed at the same time, to check the lungs for COVID-19, if this does not unduly delay stroke treatment.
Angiography is another imaging technique that allows doctors to look at the blood vessels. Implementing a “direct to the angiography suite” approach can minimize exposure to emergency department and CT personnel, and avoid unnecessary contamination of MRI devices.
Intubation is another practice that the team re-evaluated. “Mechanical ventilation may help stabilize the patient, but also may expose others to airborne risk of contamination,” Dr. Liebeskind said.
Where possible, conscious sedation can be an alternative to general anesthesia and intubation. This protects anesthesiologists from exposure, protects patients from unnecessary intubation and conserves mechanical ventilators, he said.
Finally, after thrombectomy or surgery to remove the blood clot, doctors should consider relocating patients back to primary stroke centers to recover, especially for hospitals overwhelmed with critical care or intensive care unit bed shortages. This can help maintain thrombectomy access, Dr. Liebeskind added.
Media Contact
Marrecca Fiore
310-562-4161
[email protected]