Global Health

Mission
The Department of Medicine Global Health Pathway was started in July 2013 to enhance the opportunities for global health training for Internal Medicine and Medicine-Pediatrics residents. Residents interested in the track can apply mid-way through their intern year (for IM residents) or 2nd year (for Medicine-Pediatrics residents). Residents who complete the track receive a certificate of completion acknowledging their participation at the end of residency.
The track consists of five main components:
- International electives in Malawi (Lilongwe), Peru (Iquitos), or Thailand (Bangkok); Domestic elective in Shiprock, New Mexico with the Indian Health Service.
- Longitudinal curriculum consisting of lectures and workshops
- Mentoring by Global Health faculty
- Scholarly project
- Local clinical experiences with a focus on tropical medicine and the underserved.
Curriculum
- International Electives: Residents have the opportunity to work abroad for one month in both their PGY-2 and PGY-3 years in Malawi, Peru, or Thailand. The costs of the electives are covered by the Department of Medicine, including flights, housing, local transportation and stipend.
- Domestic Electives: Residents have the opportunity to work at Northern Navajo Medical Center in Shiprock, New Mexico. This is a unique clinical experience with the Indian Health service combining inpatient and outpatient care.
- Local Clinical Experience: In addition to the international rotations, local clinical experiences are arranged in underserved settings to take advantage of global health within our community. Residents join street medicine teams caring for the homeless in their environment as well as participate in clinics at Venice Family Clinic (Simms Mann), the Travel Tropical Medicine Clinic, and our affiliated HIV clinics (CARE and THE). We are continuously developing new relationships with other pertinent clinics, such as a nearby Leprosy and Leishmaniasis clinic.
- Didactics: A longitudinal curriculum takes place in the evenings with lectures that cover topics pertinent to global health including, but not limited to, HIV, TB, malaria, STIs, dermatology, disaster preparedness, and public health. We also highlight the global health work of UCLA faculty and explore pertinent research topics through journal clubs lead by the residents. The workshops include teaching in malaria diagnostics and bedside ultrasound. This year, we have also added a street medicine component to the curriculum.
- Scholarly Activities: The scholarly project can manifest in multiple ways, including case presentations, literature reviews, or clinical research with one of the UCLA faculty.
- Mentorship: Residents will be matched with a mentor in global health to aid in developing a scholarly project and to personalize their training in line with their career and goals.
Malawi Elective
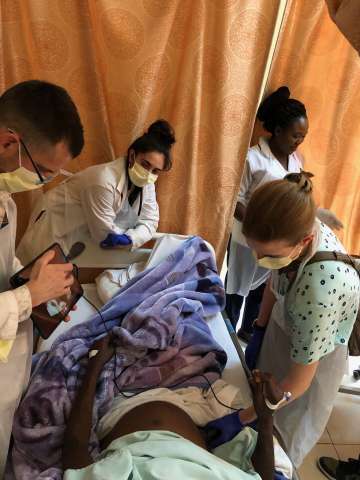
For those interested in global health, the Malawi rotation has consistently been one of the most eye opening, educational and life changing experiences in residency. Since 2007, the UCLA Department of Medicine has established a formal rotation at Partners in Hope Medical Center in the capital city of Lilongwe, Malawi. Malawi is among the poorest countries in the world with an HIV prevalence estimated at 9% and it is a leader in Africa with respect to HIV care.
Residents participating in this elective staff the free clinic which delivers primary care to HIV/AIDS patients, as well as staff the inpatient ward. A typical day consists of rounding on your inpatients in the morning, treating cases such as TB meningitis, Cryptococcus meningitis and severe malaria. Afterwards, the residents head over to the free clinic where they will diagnose multiple patients with HIV and educate them on the treatment course as well as manage complications of AIDS such as Kaposi Sarcoma. In addition to HIV/AIDS, the residents become very familiar treating pulmonary and extrapulmonary TB, malaria, other parasitic infections and common routine health problems such as diabetes and hypertension.
Residents will learn first-hand about the barriers to care in Africa and will experience the structure of the health care system by visiting facilities such as the central hospital as well as small community health centers. UCLA physicians with experience working in Malawi join the residents during their rotation to provide supervision. This rotation is extremely well organized allowing the residents to maximize their clinical experience. Thanks to the generosity of the Department of Medicine, funding is provided for roundtrip airfare from Los Angeles to Malawi, one month accommodation and food, in-country transportation to and from the clinic, and medical evacuation insurance.


Peru Elective
The Peru elective is a 4-week clinical experience available to Spanish-speaking residents that takes place at the government hospital (the Hospital Regional de Loreto) in the city of Iquitos. With a population of over half a million in the metro area, Iquitos is largest city in the Peruvian Amazon, and is only accessible by plane or boat. The Hospital Regional de Loreto is the major government referral center for the Peruvian Amazon, serving over a million residents in the city and surrounding rural communities of the Amazon basin, some of whom travel for days to reach the hospital.
Residents will spend the majority of their time in the inpatient Infectious Diseases wards under the supervision of the inpatient attending and Peruvian infectious diseases residents as well as a supervising UCLA attending. Following morning rounds, afternoons are flexible with the opportunity to participate in noon conference presentations such as morning report style cases, didactic lectures either at the hospital or at the local college of medicine, or taking call in the emergency room with one of the infectious diseases residents.

Residents will also get the chance to work in outpatient clinics in the “floating” neighborhood of Belen as well as other government community clinics such as Clinica Nanay. During the course of their rotation, they will get considerable exposure to diagnoses such as snake bites, malaria, dengue fever, leptospirosis, HIV/AIDS, tuberculosis, leishmaniasis, and helminthic infections. The costs of the Peru elective are covered by the Department of Medicine, including flights, housing, and travel stipend.
Thailand Elective

The Thailand elective is a 4-week clinical experience that takes place at the Siriraj Hospital, Mahidol University in Bangkok. Siriraj Hospital is one of the main government hospitals in Thailand and is affiliated with the oldest medical school in the country, Mahidol University. Residents will spend time on the Infectious Diseases ward and affiliated clinics, with opportunities to rotate on inpatient medicine and traditional Thai medicine.

The diseases commonly treated include HIV, TB, malaria, dengue, leptospirosis, talaromyces and melioidosis. A particular highlight of the Siriraj ID service is microbiology rounds, with intensive hands-on teaching about lab techniques, bacteria identification, and parasitology, and discuss the laboratory findings of patients on service. Rounding with the medical teams takes place in English and if needed, translators are used to communicate with patients.
Each year UCLA hosts 2 Infectious Diseases fellows from Siriraj Hospital to help maintain our partnership. Residents will be expected to participate in this bilateral exchange by giving educational presentations at Siriraj Hospital and helping to host their fellows and residents at UCLA.


Shiprock, New Mexico Elective
The Shiprock elective is a 4-week clinical experience that takes place at The Northern Navajo Medical Center in Shiprock, New Mexico. The Shiprock Service Unit is the largest service unit of the Navajo Nation, serving approximately 81,000 Native Americans (mostly Navajo). The inpatient load is approximately 30 per day and the outpatient volume averages around 600 per day. The population is dispersed and many people live in homes without running water or electricity.
Residents have the opportunity to split their time between inpatient and outpatient clinical experiences. In the morning, they participate in ICU rounds where the entire internal medicine and family medicine departments put their heads together to care for the hospital's sickest patients. They then round on their ward patients, and proceed to various clinics including primary care, neurology and rheumatology. They can admit patients from clinic and follow them for their entire hospital admission. Residents also accompany attendings on home visits and on trips to remote clinics. Residents learn about diseases that are prevalent in the Navajo population as well as the socioeconomic factors that influence health. They also meet traditional healers and learn about Navajo health and medicine.
Outside of the hospital, residents have the opportunity to live alongside a close-knit group of medical providers and their families on the hospital campus. Indoor potlucks and outdoor mesa nights are an important part of the Shiprock experience. On the weekends, there is time to explore the rich history, beauty and adventure of the reservation and the Southwest.
If you have any questions or need further information regarding the UCLA Global Health Pathway, please contact Mercedes Vasquez, Program Coordinator at [email protected] or Dr. Christopher Tymchuk, Pathway Director at [email protected]