Parathyroid Hyperplasia
Find Your Care
We deliver effective, minimally invasive treatments in a caring environment. Call 310-267-7838 to connect with an expert in endocrine surgery.
Parathyroid Hyperplasia: Symptoms, Treatment, Diagnosis
Definition
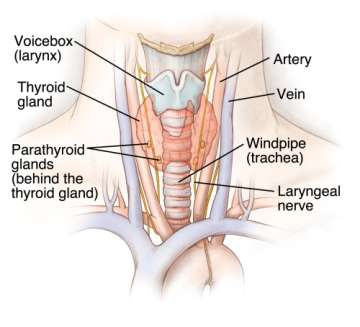
What is Parathyroid Hyperplasia?
Parathyroid hyperplasia involves enlargement of all four parathyroid glands, which are located in the neck and control calcium metabolism. The condition produces high levels of calcium in the blood (hypercalcemia).
Causes, incidence, and risk factors:
Parathyroid hyperplasia causes about 15% of cases of hyperparathyroidism, which leads to elevated levels of calcium in the blood (hypercalcemia). Parathyroid hyperplasia may occur sporadically (without a family history) or as part of three familial (inherited) syndromes: multiple endocrine neoplasia 1 (MEN 1) and MEN 2A and isolated familial hyperparathyroidism. In the familial syndromes, a mutated gene is inherited in an autosomal dominant fashion (you only need to get the gene from one parent to develop the condition). In MEN 1, the problems in the parathyroids are associated with other tumors in the pituitary and the pancreas. In MEN 2A, the overactivity of the parathyroids is associated with tumors in the adrenal gland or thyroid. The genetic basis of isolated familial parathyroidism is not yet clear.
Symptoms:
Symptoms of hyperparathyroidism associated with parathyroid hyperplasia may include:
- lethargy
- nausea
- constipation
- myalgias (muscle pains)
- kidney stones
- bone fractures
Signs and tests:
Signs of hyperparathyroidism associated with parathyroid hyperplasia may include:
- fractures
- renal colic
Tests may show:
- elevated serum calcium
- low serum phosphorus
- elevated intact PTH
- elevated serum chloride
- low serum bicarbonate
- elevated 24-hour urine calcium
- low bone mineral density
Treatment:
Surgery is the preferred treatment. Usually 3 1/2 glands are removed. The remaining tissue may be implanted in the forearm to regulate calcium levels but allow easy surgical access if hypercalcemia recurs.
Expectations (prognosis):
The success rate for surgery for parathyroid hyperplasia is lower than that for parathyroid adenoma. Persistent or recurrent hypercalcemia occurs about 20% of the time.
Complications:
Advanced complications of hyperparathyroidism associated with parathyroid hyperplasia include nephrocalcinosis and osteitis fibrosa cystica. Patients may also have complications from the other endocrine tumors that are part of the multiple endocrine neoplasia syndromes:
- MEN 1 -- includes pancreatic and pituitary tumors, adrenal adenomas and lipomas
- MEN 2A -- includes medullary carcinoma of the thyroid and pheochromocytoma
Calling your health care provider:
Call your health care provider if you have any symptoms of hypercalcemia, or there is a family history of any of the MEN syndromes
Prevention:
Patients with a family history of the MEN syndromes may be genetically screened for presence of the defective gene and then screened regularly with standard diagnostic methods for endocrine problems if this test is positive.