Oral Cancer
Find Your Care
Our head and neck surgeons consistently rank among the best in the nation. To find out more about our services, call 310-206-6688.
What is the oral cavity?
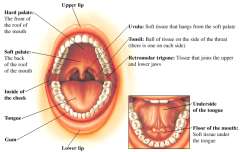
The oral cavity refers to a person’s mouth. The subsites of the oral cavity include the tongue, teeth, gums, jaws, floor of mouth, and the inner the lining of the cheek (buccal mucosa). The oral cavity plays an integral role in chewing, speaking, and swallowing.
How common are oral cancers?
More than 26,000 new cases of oral cavity cancers will be diagnosed in the United States this year, and 300,373 worldwide. Oral cancers make up the majority of head and neck cancers. While oral cancers are frequently diagnosed at early stages, the five-year overall survival rate remains around 50% even in developed countries. Treatment of cancer at an early stage can make a big difference.
The incidence of oral cancers is on a general decline—mainly due to less smoking and drinking—however, young Caucasians, African Americans, and females are becoming more impacted by oral cancers. The increased use of tobacco and smoking among women may be linked to the increased oral cancer incidence in women.
(Useful reference: Listl S, Jansen L, Stenzinger A, et al. Survival of patients with oral cavity cancer in Germany. PLoS One. 2013;8(1):e53415]
Can young people get oral cancers?
Historically, cancers have been considered a disease of the elderly. Recent studies, including a landmark collaborative study by UCLA, have shown that the incidence of oral cancers has been increasing in young, Caucasian patients who live in affluent communities. We do not yet have a good explanation for this epidemiological finding, but UCLA Head and Neck Surgery is at the forefront of opportunities to reveal potential causes (see below: What efforts are being made to understand more about oral cancers?).
[Useful Reference: Tota JE, Anderson WF, Coffey C, et al. Rising incidence of oral tongue cancer among white men and women in the United States, 1973-2012. Oral Oncol. 2017;67:146-152.]
What causes oral cancers?
As the mouth serves as an interface to the outside world, exposure to carcinogens is attributed to causing oral cancers. Chemical carcinogens such as tobacco (smoked, chewable, or secondhand exposure) increases the risk of oral cancer by 1.7-fold. Alcohol consumption, marijuana smoke, and betel quid chewing are also linked with the development of oral cancers.
Some studies suggest that oral hygiene (periodontitis), use of mouth wash that alters the oral microbiome, diet (low vegetable consumption), and environmental exposure (proximity to specific industries) may also play roles.
Does the human papillomavirus (HPV) cause oral cancer?
The epidemic of human papillomavirus (HPV) has been on the rise in recent decades. The head and neck subsite most impacted is the throat (also known as the pharynx), where the majority of throat/oropharyngeal cancers are caused by chronic HPV infection. In contrast, only a smaller portion of oral cancers are considered to be directly related to HPV infection.
[Useful reference: Herrero R, Castellsagué X, Pawlita M, et al. Human papillomavirus and oral cancer: the International Agency for Research on Cancer multicenter study. J Natl Cancer Inst. 2003;95(23):1772-1783.]
What are some treatment options for oral cancer?
Any medical intervention for oral cancer requires careful planning to preserve the function and appearance of the face while eradicating the tumor with minimal potential for recurrence. Precision surgery is the cornerstone of oral cancer management, in which the goal is to achieve removal of the cancer with sufficient margins. In easily accessible areas, your surgeon will determine the margins under surgical loupes. If the area is difficult to reach, a surgical robot will be used to assist in the resection of the tumor (also known as TORS or Trans Oral Robotic Surgery). Clear margins will be confirmed using rapid (also known as intraoperative) histopathological analysis under the microscope by a senior pathologist. In advanced cancers, it may be necessary to remove involved muscles and bones. In such cases, a graft or flap can be utilized to preserve the function and appearance related to the mouth and face.
Depending on the findings from surgery and a physical exam–chemotherapy, radiation therapy, or immunotherapy may be included as part of the treatment regimen. In general, pembrolizumab (Keytruda) and nivolumab (Optivo) are reserved for very advanced-stage disease. Our experienced medical oncologists at UCLA will discuss your eligibility as well as the risks and benefits of including these options with you in detail.
TORS Surgery Patient Stories:
Can I be cured from oral cancer?
Only a patient-specific treatment regimen will maximize function, appearance, and survival during the treatment of oral cancers. The combination of surgery, radiation, chemotherapy, and immunotherapy will remove both obvious and microscopic tumors. After treatment, we will provide scheduled exams for active surveillance of the site of the tumor. Additional blood tests or cross-sectional imaging can be used to obtain more information about suspicious lesions. Cancers most often recur within the first two years after treatment. In general, a cancer is considered “cured” when no recurrence is observed five years after the treatment. Our cancer survivorship program clinic will continue to work with you to help with speaking, swallowing, and aesthetics even after the completion of your treatment.
Why should I choose UCLA Head and Neck Cancer Program?
UCLA Head and Neck Cancer Program is one of the nation’s first multidisciplinary treatment centers specialized for head and neck cancers. We will provide a personalized approach to your cancer and your social and emotional needs. We offer the latest in tumor margin analysis and reconstruction of the oral cavity after surgery so you benefit from complete surgical resection while maintaining function of your oral cavity. We continue to serve more than 50,000 patients each year. Our team of experienced surgeons, medical oncologists, radiation oncologists, psychologists, and other support staff will exceed your needs.
What efforts are being made to understand more about oral cancers?
Since its inception, UCLA Head and Neck Cancer Program (HNCP) has been at the forefront in grant-funded research to uncover the causes of oral cancers and offer the newest treatments from bench to bedside via clinical trials. The latest projects include the study of dysbiosis in oral cavities of young patients with tongue cancer as well as deep sequencing of HPV in oral cancers compared to oropharyngeal cancers. Our collaboration with medical oncologists aims to determine the optimal timing and indications for immunotherapy in oral cancers.
Please contact 310-267-7076 to enroll in clinical trials or offer a special gift toward our oral cancer research.
Other useful links for oral cancers:
What are oral cancers?
Surgery for Oral Cancer
What Happens During Surgery for Oral Cancer