Deep Vein Thrombosis (DVT)
Find your care
Our clinic is nationally and internationally renowned for IVC filter removal. Call 310-481-7545 to learn more about the IVC Filter Clinic at UCLA Health.
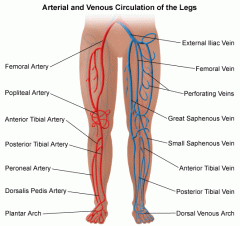
Deep Vein Thrombosis (DVT) is the medical term for blood clots within the veins, usually within the legs. The term venous thromboembolism (VTE) is also frequently used, and in fact describes two conditions, DVT and pulmonary embolism (PE) or clots in the lungs. This term is used because the two conditions are very closely related, and because their prevention and treatment are also closely related.
Deep vein thrombosis is a blood clot or thrombus in a deep vein. They are most common in the legs. But they may develop in the arm or other part of the body. Part of the clot, called an embolus, can break off and travel to the lungs (PE). This can cut off the flow of blood to all or part of the lung. PE is an emergency and may cause death.
DVT is extremely common, and affects up to 900,000 people in the US per year. There are several risk factors including obesity, surgery, immobility, birth control pills, a family history of blood clots, varicose veins and cancer. However frequently no cause is found. Most people with DVT develop symptoms of pain, swelling, and redness in the leg, arm, or other area. Sometimes DVT is symptomless. Over time the clots can resolve or complications can occur. The two most common complications of a blood clot are chronic venous insufficiency and post-thrombotic syndrome.
- Chronic venous insufficiency may happen following a blood clot in a leg vein. It means that a vein no longer works well. It is a long-term condition where blood pools in the vein instead of flowing back to the heart. Pain and swelling in the leg are common symptoms.
- Post-thrombotic syndrome may also happen following a blood clot in a leg vein. It is a long-term problem with pain, swelling, and redness. Ulcers and sores can also happen. All of these symptoms may make it difficult to walk and take part in daily activities.
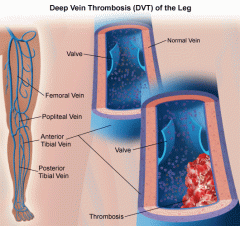
How is deep vein thrombosis diagnosed?
Along with a medical history and physical exam, your healthcare provider may do other tests including:
- Duplex ultrasound. This painless procedure involves placing ultrasound gel on the affected area and then moving a handheld device across it. A picture of the blood flow is displayed on a monitor. Duplex ultrasound is the most common test for DVT.
- Lab work. Blood work may be done to look for blood clotting and other problems.
What is the treatment for deep vein thrombosis?
Specific treatment will be determined by your Vascular Interventional Radiologist specialized in venous disease based on:
- Your age
- Your overall health and medical history
- How sick you are
- The location of the clot
- How well you can handle specific medicines, procedures, or therapies
- How long the condition is expected to last
- Your opinion or preference
The goal of treatments is are to prevent the clot from getting larger, to prevent a blood clot from traveling to the lungs (PE), to decrease the chance of another blood clot forming and to prevent development of PTS.
Treatment may include:
- Blood thinners (anticoagulant medicines).
- Walking. Getting up and moving as soon as possible after diagnosis.
- Elastic or compression stockings, if prescribed by your healthcare provider.
- Clot busters (fibrinolytics or thrombolytics). These medicines are used to break up clots and can be given directly into the clot by your Interventional Radiology specialist using a minimally invasive endovascular therapy called Catheter Directed Thrombolysis (CDT). This is typically a day case, and has been shown to help symptoms and complications of DVT in carefully evaluated patients.
- Clot suction. These devices are small (less than width of a pen) and can be placed directly into the vein by an IR specialist where the clot is and then the clot removed, allowing normal blood flow to pass again.
- Inferior vena cava filter.In some cases, a filter is placed in the vena cava (the large vein which returns blood from the body to the heart). This filter prevents clots from reaching the heart and lungs.
For an expert evaluation or to discuss any of these treatment options, please contact our expert Vascular Interventional Radiologists at (310) 481-7545