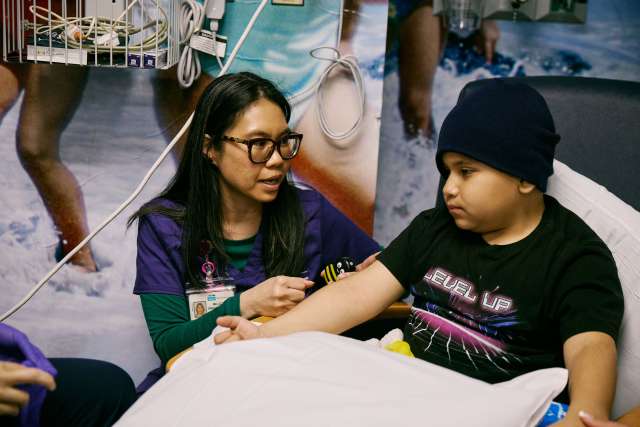Child Life Specialists are the only people on the hospital staff who get paid to play with kids, says KellI Carroll, MS, CCLS, director of the Chase Child Life program at UCLA Mattel Children’s Hospital.
But they do so much more than that.
“Child Life Specialists are dedicated to helping kids be kids while they’re in the hospital,” Caroll says. “It’s not just about physical healing, but the emotional safeguard we provide the family and the kiddo as well.”
Child Life Specialists help children and families navigate the uncertainty of diagnosis and treatment, serve as a liaison between a patient’s care teams and provide levity, play and emotional support. Every inpatient child at UCLA Mattel Children’s Hospital is met and assessed by the department’s 22 Certified Child Life Specialists.
And while Carroll says she hopes families “never have to meet a Child Life Specialist” because their children are never hospitalized, it’s important to ask for one if they ever are.
“We are often unseen professionals in the medical space,” she says. “But we are the people who are going to help you or your child not just heal physically, but heal emotionally and intact and ready to take on life.”
In honor of March being Child Life Month, meet two of UCLA Health’s Child Life Specialists, in their own words.
Hanna Skane, MS, CCLS
Losing one of my best friends to cancer while we were in college ultimately inspired me to become a Child Life Specialist.
After Madison died, I ended up doing a lot of philanthropy work through my sorority with St. Jude Children’s Research Hospital. I’ve always loved working with kids. I have like a thousand nieces and nephews. I started volunteering at MemorialCare Miller Children’s & Women’s Hospital in Long Beach with their Child Life program, which helped me to learn more about the field before entering it myself.
After finishing my masters and a Child Life internship at Memorial Sloan Kettering Cancer Center in New York, I came to UCLA Health in 2023. I worked in the emergency department before moving to pediatric oncology at UCLA Mattel Children’s Hospital.
We’re here to help kids cope while being in the hospital, whether that’s making sense of a diagnosis, helping them through treatment or being an emotional support for them through the end of life.

The main skill is being able to build rapport with these kids. That might mean getting on the floor with younger kids and playing Barbies or dinosaurs, or sitting with teenagers and offering a space for them to be themselves and reclaim some of their identity beyond their diagnosis.
I think that’s something Madison struggled with a lot in the end — not being treated like a 19-year-old college kid and feeling like she was just the sick girl who had to leave school.
I have a lot of young adult patients, in the 18- to 22-year-old range. That’s a big population in pediatric oncology. These are some of the hardest ones for me. They’re a little closed off and a little unsure, like, ‘Do I need a Child Life Specialist? I’m 20 years old.’ It’s truly an honor when they let you in. They already have so much life behind them, and have dreams and goals they want to accomplish. We get to know them so well and I want them so badly to achieve all their dreams and goals. So it can be really hard when we see that they’re not going to be able to fulfill everything that they want to.
There’s no real typical day at this job. The first thing I do when I come in in the morning is check my list of patients and see if anything’s changed from the day before. I usually have eight to 10 patients. Some weeks it could be as few as five or as many as 14.
If any of my kids have a procedure in the morning, that’s always a priority. I’ll accompany them to their procedure and just stay with them until they fall asleep. If we have any end-of-life situations or bereavement support that’s needed, that’s obviously going to be a priority. We may spend the whole day with the family, helping siblings if they’re there, creating memory-making items. There are days that it’s just kids here for their chemo admissions, which means they’re stuck in their room, so I just try to entertain them and support them through that. After that, it’s really just checking in and spending time with the kids — sitting with them, talking with them, playing with them, giving them whatever space they need.
The other day, I was playing Monopoly with one of my patients, and he started opening up about some challenging family dynamics. We were just sitting there playing a game together and he led the conversation, which was incredible.
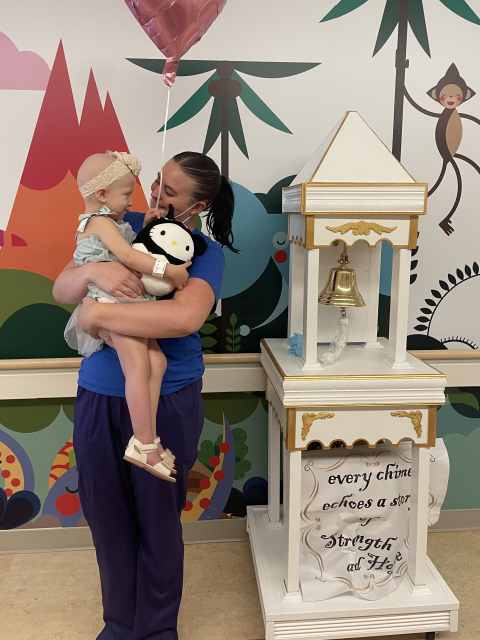
I definitely struggle with leaving here and not being consumed with thinking about the kids here and hoping they’re doing OK. We’re all really close in this department. I think the wins really do matter — like when a kid finishes treatment and gets to ring the bell, when they get to be discharged, seeing them go off to college. We have to really sit in that and feel the joy of that to kind of outweigh the really difficult losses that we have.
It’s such an honor to know these kids and families. They’ve all impacted me in a different way. And every kid that I’ve lost, I just know I will remember them forever. I have photos of all my patients here on my desk. I’m very privileged to get to know them on such a deep level and have these relationships with them. As difficult as the losses can be — there are days that I don’t know if I can show up again the next day — I’m glad that I do. I’m glad that I show up for the next kid and take whatever I learned from the last patient and show up for them even better. I’m very thankful that I get to do this job.
Millicent Ongaco, MS, CCLS
I originally thought I was going to be a teacher, because I love working with kids. But I realized teaching in a traditional classroom setting was not for me.
"After graduating from college, I spent five years working in a domestic violence shelter and transitional housing, supporting kids’ emotional safety. I went to a conference about early childhood education and ended up learning more about Child Life. I was interested, because I’d always wanted to work in medicine, too, and this was the perfect marriage between working in the medical field and being able to engage with kids at their level. That’s what had appealed to me about teaching, but I didn’t want to commit to one grade, one age group. In Child Life, I could be working with an infant in the morning, and then a school-age child, a teen, a toddler and a young adult, all in the same day.
I’ve been a Child Life Specialist for 17 years, the last 10 at UCLA Health. I work in the pediatric infusion center, so it’s an outpatient setting. I meet with whoever is on the schedule that day — it could be patients of any age, plus parents or caregivers.

The first thing I do is introduce myself and try to find out about them and what they know about what’s about to happen, because they could be in a really vulnerable state. They may have needle phobia; they could be really scared about a test being done; they might be dealing with a new diagnosis. So they might have a lot of feelings, and I want to create a safe environment for them to explore those feelings. I mostly just want to find out how I can help them, how I can serve them. From there, I’ll make a plan to make sure they feel safe, understand what’s happening and realize they still have agency. There’s a lot they don’t have a choice in, but there are other things where they do have a say. I want to make sure they feel like they are part of the process.
This job really requires really being attentive to patients’ energy and the energy in the room. I acknowledge that they don’t know me and the whole situation can be awkward and scary. I invite the parent or caregiver into the conversation, too. With younger kids, maybe they brought in a stuffed animal and I’ll ask its name. I’ll bring in a stethoscope and ask if they know how to listen to its heart. Or if they’re wearing a Super Mario shirt, I’ll ask if that’s their favorite game. Bubbles are usually pretty effective. You try to find different ways to connect and build rapport, so hopefully their anxiety goes down.
I apply this to working with parents and caregivers, too. I’m used to working with kids and teens and young adults, different age groups and developmental levels. But then I've also had to add a component of working with the adult in the room as well, because sometimes adults are really nervous. They may not want the child to know why they’re in clinic, but then the child themselves may be asking.
Sometimes I’ll be answering questions for a patient and you see the light bulb go on in the parent’s head, like, “Now I understand.” It’s amazing how much the work I do can even dispel some of their misconceptions.
It can be a challenge to balance and prioritize everything we have going on. It’s easy to get caught up in all of the feelings, the celebrations and the sadness, because we are literally in the middle of folks dealing with life or death. Our role is really broad, because we do a lot of the fun stuff, but we also do hold a lot of emotion for these patients and families. We deal with a lot of sad things, that’s part of the job, but it’s not the only part. I have to make sure I find the glimmers of joy within my day, like playing a game of Uno with a patient, or putting together a puzzle, or making slime together, or just talking about things that bring them joy.

Over the years, I’ve realized that play is my superpower. That’s how we’re able to bridge the gap with kids. It’s a nonthreatening way of communicating and a quick way to build trust. In this setting, where there are so many stressful and traumatic things, sometimes just going back to simple play helps shift and refocus the situation. There are so many facets and layers to our work, but play is definitely the foundation.