As a Hispanic woman growing up in the New Mexican desert, my skin tone would shift from caramel brown to mocha brown during the summertime months. I hardly wore sunscreen because I didn’t think I needed to. Friends and family would pour baby oil on their legs and lay out in the sun.
Among the Hispanic and Latino people that I knew, skin cancer was not top of mind. We didn’t realize our behaviors were risky.
My goal is to change that mindset.
On Feb. 23, 2022 I learned that a mole on my ankle was melanoma, a type of skin cancer that begins in the melanocytes, which controls the pigment in the skin.
This can’t be happening to me; skin cancer happens to people with fair skin who sunburn easily, I told myself. Unfortunately, this is a belief that many people hold.
Hispanic/Latino people come in all shades of skin tones. And while it’s true that people with lighter skin tones have the highest risk for skin cancer, the incidence of melanoma among Hispanic/Latinos has risen by 20% over the last two decades, and continues to rise, according to recent research.
Data show that on average, Hispanic/Latino people present with thicker tumors and have tumors that are more likely to metastasize (spread) than their white peers. Reasons for these disparities might include being unaware of risks and symptoms, a lack of sun-safe behaviors and less access to health insurance.
Not all melanomas are caused by exposure to ultraviolet (UV) radiation from the sun or tanning beds. The exact origins are complex, and for some, it can be genetic or due to genetic mutations. To my knowledge, I’m the first in my family to have melanoma. It wasn’t until I was out of college and working as a reporter that I even learned what it was.
In 2013, I wrote a story about a 25-year-old woman named Erin Wright Turner, who had beaten stage-3 melanoma, twice, after it had spread to her liver. She died a year later, in 2014, after battling cancer for six years.
Turner was an inspiration to our community. She spoke about her condition and on the importance of sun safety with others openly. On the day before her appointment at MD Anderson to remove some of the tumors, she ran a 10-mile race.
Because I had reported on Turner’s story, I was aware of the risks and still, I didn’t think it could happen to me.
Early prevention is key
Late last year, I noticed a node-like bump on my back that became itchy.
I emailed my primary care provider for her opinion. Without hesitation, she gave me a referral to see a dermatologist.
At my appointment with dermatologist Mengjun Hu, MD, she noted that the bump on my back was likely benign, but she would have it biopsied to make sure. What she did find suspicious was a mole on my left ankle that looked much darker than the rest of my moles.
I had once been suspicious about this mole, too. Over the years it had grown in size and darkened to a blackish color.

In 2020, while a patient at a different health care system, I asked my primary care provider for a dermatology referral. Because the COVID-19 pandemic was raging, I was scheduled for a virtual visit with a dermatologist.
During the visit, I zoomed in on the mole as best as I could and pointed out the changes I had seen, including the darkened color. The dermatologist said it looked normal to him. He said if I noticed any additional changes, I should reach back out.
In the meantime, I switched my health care over to UCLA Health. On March 21, 2022, dermatologic surgeon Jenny Kim, MD, PhD, extracted a half-dollar-sized section of skin from my ankle to ensure the melanoma hadn’t spread. A week later, I had a skin graft by Andrew Vardanian, MD, who specializes in scar management and plastic surgery, to close up the wound on my ankle with skin from the front of my thigh.
This was my first surgery in almost 20 years and naturally, I was nervous. I shared my uneasy feelings with the nurse and anesthesiologists and they each assured me I wouldn’t feel pain.
Both anesthesiologists shared their skin histories with me, too.
One shared that she too gets frequent skin checks for melanoma. She said she always thought people with fairer skin and lighter eyes were more at risk. (“Me too,” I said to her.) We talked about singer and activist Bob Marley, who died at 36 from a melanoma that began in his big toenail and spread to his brain, lungs and stomach.
The other anesthesiologist showed me a scar above his eye, where he had Mohs surgery for a basal cell carcinoma, one of the most common types of skin cancer.
Their vulnerability reassured me that I was in good hands with people who understood my experience.
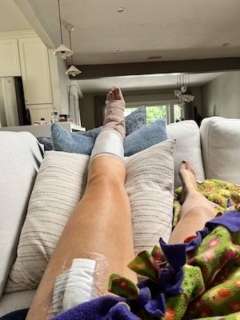
After the surgery, the months-long healing process began. Because of the location on my ankle, I was given orders to elevate, rest and stay off my feet as much as possible.
A little over a month later, I’m almost fully healed. The skin from the donor site is hot pink in color, but healing, and the skin graft continues to change color and texture as the graft heals.
I also got some closure with my original skin visit. The bump on my back was diagnosed as a cellular dermatofibroma, a benign buildup of soft tissue cells under the skin, which will get removed this summer.
Access and equity
Though the melanoma was caught at the earliest possible stage, the entire experience made me think more deeply about mortality, access and privilege.
I grew up on Medicaid. For periods in my adult life, I was not insured. I wonder what the outcome might have been had I not been privileged to have the employment that afforded me health insurance and access to world-class doctors.
In addition to access, I wonder about the gap in skin-related education among Hispanics and Latinos, Asians, Native Americans, and Black people.
In 2021, dermatology was named the second-least diverse specialty in medicine. Though UCLA is taking steps to improve diversity and health equity, change, like healing, takes time.
In the meantime, recommendations call for mentorship for students of color that are considering the specialty, implicit bias training at all levels, and education and understanding of skin conditions and how they present on various skin tones.
My urging to all is to check your skin carefully. Ask a partner, family member or friend to check the spots that aren’t visible to you – like the back of your body, underarms and elbows. If you notice a change, get it checked out.
My dermatologist, Dr. Hu, shared with me the ABCs of melanoma to watch out for:
A – Asymmetry: If a mole or lesion isn’t symmetrical, or the two halves don’t match.
B – Border: If the borders are uneven, notched or jagged.
C – Color: If the mole or lesion has different colors or changes colors.
D – Diameter: If the mole or lesion is the size of a pencil eraser (6 mm or ¼-inch in diameter) or larger.
E – Evolving: If it’s changed in color, shape, size, is crusting, itching or bleeding.
Have these conversations with your families, encourage routine skin checks and be vigilant about any changes to your skin.
Learn more about melanoma and skin cancer prevention.



