Endometrial cancer is the most common gynecologic cancer in the United States and is one of the few cancers in which survival rates have steadily declined over the last few decades. The most aggressive subtypes are a significant driver of that trend: uterine papillary serous carcinoma accounts for just 10% of diagnoses but nearly 40% of deaths.
Now, UCLA researchers have developed a novel immunotherapy that could begin to change the calculus for a disease that has resisted treatment progress. In a study published in Experimental Hematology & Oncology, the team describes how CAR-NKT cell therapy is more effective than current immunotherapies at fighting endometrial cancer.
“Across all forms of endometrial cancer, recurrence remains one of the greatest challenges — and it’s especially frequent and devastating in aggressive subtypes,” said gynecologic oncologist Dr. Sanaz Memarzadeh, a co-senior author and a member of the Eli and Edythe Broad Center of Regenerative Medicine and Stem Cell Research at UCLA. “Patients often discover the cancer has returned after undergoing a combination of surgery, chemotherapy and radiation, so it’s crucial that we devise and test new therapeutic strategies that can help save women’s lives.”
While current personalized immunotherapies can cost hundreds of thousands of dollars and take weeks to manufacture, the new therapy sidesteps both problems, using an off-the-shelf production platform designed to make treatment more accessible and affordable.
How CAR-NKT cells strike cancer on multiple fronts — safely and precisely
The therapy centers on a rare but powerful type of immune cell called invariant natural killer T cells, or NKT cells. When equipped with a chimeric antigen receptor, or CAR, targeting mesothelin — a protein found on endometrial cancer cells — these engineered cells can precisely detect and destroy tumors through three pathways simultaneously, unlike conventional CAR-T cell therapies, which rely on a single recognition mechanism.
“This cancer is remarkably good at escaping treatment, but it can’t escape multiple attack pathways at once,” said co-senior author Lili Yang, a professor of microbiology, immunology and molecular genetics and a member of the UCLA Broad Stem Cell Research Center. “By the time it adapts to one threat, our therapy has already hit it from another angle.”
The most striking results came from mouse models of endometrial cancer: The therapy achieved complete tumor elimination and prolonged survival, while conventional CAR-T cells used as a comparison provided only partial, temporary control before tumors returned.
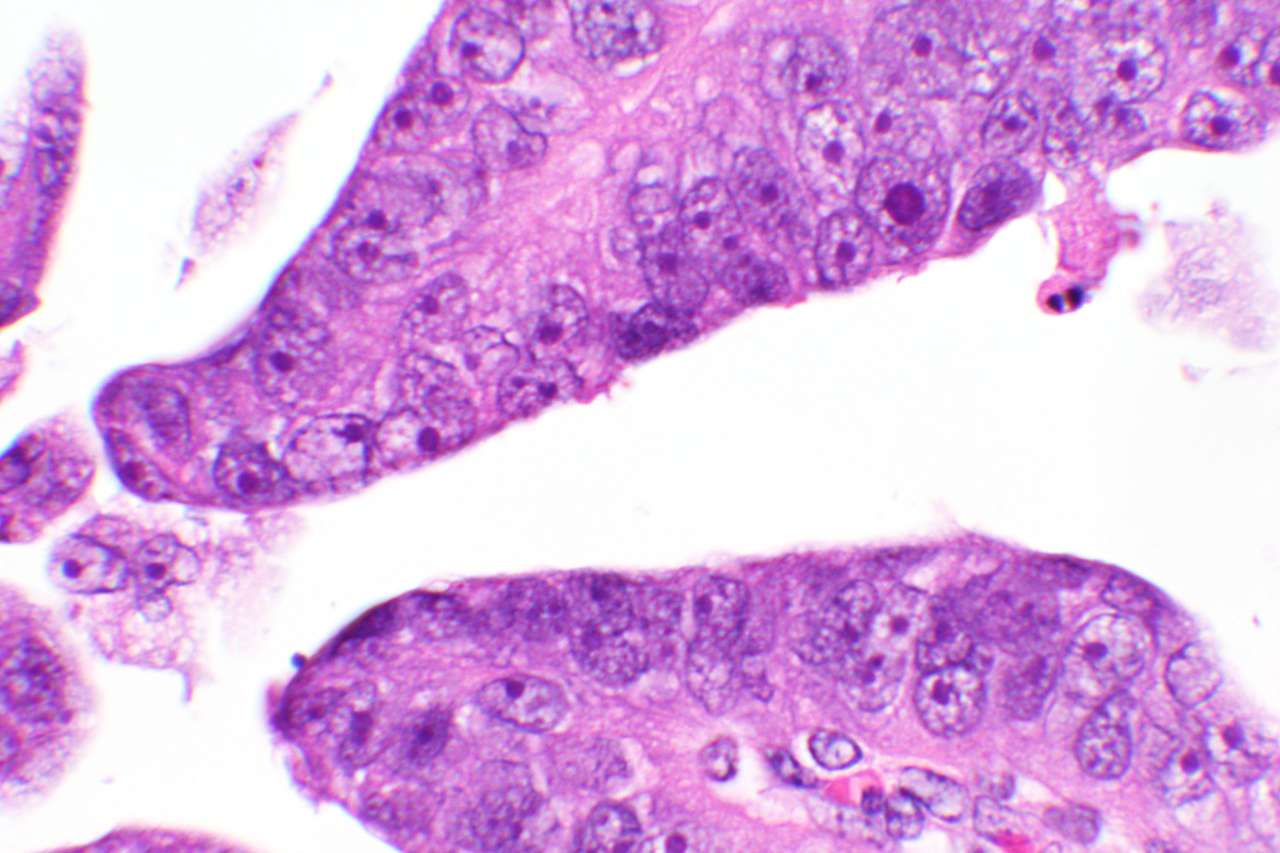
Broader testing across patient tumor samples and patient-derived tumor cell lines confirmed the therapy’s superior cancer-killing ability in aggressive endometrial cancer subtypes such as uterine papillary serous carcinoma.
Crucially, the CAR-NKT cells showed no safety concerns. They didn’t trigger graft-versus-host disease, a dangerous condition in which donated immune cells attack healthy tissues.
A therapy that’s ready when patients need it
Current personalized immunotherapies require collecting a patient’s own immune cells, shipping them to a specialized facility for genetic modification and returning them to the patient — a process that can take several weeks and cost well into the six figures.
The UCLA platform addresses both barriers. CAR-NKT cells are produced from donated blood stem cells in a scalable process, and because NKT cells are naturally compatible with any immune system, a single donation can yield enough cells for thousands of treatments.
“The idea is to pre-make the product, cryopreserve it and have it ready to go as soon as the patient needs the therapy,” said Yang, who is also a member of the UCLA Health Jonsson Comprehensive Cancer Center.
One product to tackle breast, ovarian, endometrial, lung and pancreatic cancers
One of the most consequential features of the therapy is its versatility. Because mesothelin is expressed not only in endometrial cancer but also in ovarian, breast, pancreatic and lung cancers, the same manufactured product could be used to fight a wide range of tumors.
“This is a platform technology,” said co-first author Yanruide (Charlie) Li, a postdoctoral scholar in the UCLA Broad Stem Cell Research Center Training Program. “The goal is one product that doesn’t require patient-by-patient customization.”
With all preclinical studies now complete, the team is preparing to submit applications to the Food and Drug Administration to begin clinical trials.
“Despite its prevalence, endometrial cancer remains understudied,” Memarzadeh said. “Research efforts and funding is how that changes. It’s what allows us to ask important questions, develop innovative therapies and ultimately get them to the patients who need them.”
Additional authors include Gabriella DiBernardo, Yuning Chen, Xinyuan Shen, Ryan Hon, Lauryn Ruegg, Jie Huang, Adam Neal and Neda Moatamed.
The research was supported by the California Institute for Regenerative Medicine, the Department of Defense, the UCLA Broad Stem Cell Research Center, the Wendy Ablon Trust, the Department of Veterans Affairs, the Parker Institute for Cancer Immunotherapy, UCLA’s department of microbiology, immunology and molecular genetics, the UCLA Office of the Chancellor and the UCLA Goodman-Luskin Microbiome Center.
The therapeutic approach described in this study has been used in preclinical tests only; it has not been tested in humans in clinical trials or approved by the FDA as safe and effective for use in humans.





