“The brain is like real estate,” says May Nour, MD, PhD, vascular and interventional neuroradiologist, director of UCLA Health’s Mobile Stroke Rescue Unit. “Location, location, location. There is eloquence in the tissue and losing two million neurons per minute in a clinically significant region of the brain, can leave someone with grave disability for the remainder of their life. Returning blood flow swiftly to the deprived tissue is essential for meaningful recovery.”
That reality is a call to action, says Satoshi Tateshima, MD, DMSc, professor of radiology, division of interventional neuroradiology, Ronald Reagan UCLA Medical Center. “Rapid opening of the blocked vessel is key to survival and quality of life. We must provide care as soon as possible,” he says.
The most fortunate stroke patients are swiftly transferred to facilities (like Ronald Reagan Medical Center) where neurointerventionalists can perform a thrombectomy. This procedure is a manual mechanical removal of a clot. It restores blood flow to brain tissue before it dies.
“Interventionalists insert a catheter, advance it into the blocked artery and remove the occlusion using retrievable stents, suction devices or both,” says Dr. Saver. “It’s been a major breakthrough here, improving outcomes for 40% of patients otherwise headed for a devastating stroke.”
But for patients in rural or underserved communities lacking quick access to tertiary hospitals, the clock may run out. “This country is huge, making disparity of subspecialty care an issue,” says Dr. Tateshima. “Patients delayed even an hour may not make it. Even emergency air transfer is unreliable due to weather conditions and flight risks.”
An emerging solution
Drs. Tateshima, Saver and Nour are among the members of a UCLA team working to perfect robotic thrombectomy, and ultimately, remote robotic thrombectomy.
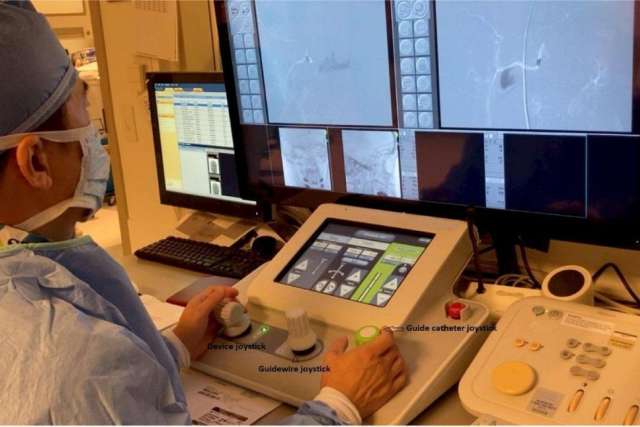
“During robotic thrombectomy, interventionalists control navigation of catheters and deployment of retrieval devices, not by putting their hands on the wire at the groin or wrist, but on joystick controls directing the robot to grip the wire,” says Dr. Saver. “Interventionalists are outside of the procedure room, behind glass. Thus, their radiation exposure is reduced.” (Studies have shown interventionalists have higher than normal rates of cancer related to radiation and back disease caused by wearing heavy protective lead aprons.)
If robotic thrombectomy can be done outside the procedure room, can it also be done remotely from many miles away? UCLA’s team says “yes.”
“Interventionalists will be at one hospital, and patients at distant hospitals,” says Dr. Saver. “Long delays in getting to a thrombectomy center will disappear because patients will go to local hospitals where procedures can be done remotely, quickly. That saves more brain.”
Stroke patients in rural or underserved communities often do not have access to the most advanced, life-saving treatment options in their local hospital, says Geoffrey Colby, MD, PhD, director of cerebrovascular neurosurgery.
“Robot technology combined with remote control capabilities will allow an experienced specialist in one location to perform a sophisticated, minimally invasive surgery for a patient in need at another location,” says Dr. Colby. “The ability to intervene from afar should greatly reduce time needed to initiate treatment and ultimately lead to better patient outcomes.”
Thanks to other types of robotic surgery, technology required to perform robotic thrombectomy is already a reality. In Canada, a recent hybrid remote thrombectomy required an on-site physician to puncture the artery, guide the catheter into the patient’s neck and the microcatheter into the groin. Then the microcatheter was hooked into the robotic system and the rest of the procedure was done remotely.
“At UCLA, we want to do it differently,” says Dr. Tateshima. “Once a local physician establishes arterial access, we want our robot to put the guiding catheter into the neck, the microcatheter into the brain and open up the occlusion. We call that ‘complete robotic.’”
Successful simulations
The UCLA team now performs remote thrombectomy simulations on patient models and collects vital data. “Our chance of successfully removing a clot from a brain artery and restoring blow flow robotically is the same as in a manual procedure. Though a bit slower, we still can give patients a better chance to survive and recover normally compared to those delayed in transfer to a thrombectomy center,” says Dr. Tateshima.
“We have a geographic mapping of all the California hospitals providing stroke care, some of which only provide medicine, not catheter-based treatment,” he continues. “Medicine only is inadequate. We’ve already identified that when stroke centers are more than 50 miles away from a hospital that performs catheter-based treatment, converting them into remote thrombectomy centers would be particularly beneficial because delay to treatment would be reduced by three hours and 30 minutes, on average.”
It should be noted there are still challenges, not least of which is FDA approval. In addition, when relying on remote technology, there must be absolute certainty of uninterrupted internet connection. “Communication technology has to develop at the same time as the medical technology,” says Dr. Nour. “It’s no small task.”
But UCLA is up for the challenge. “What’s the alternative?” asks Dr. Tateshima. “If we do not find a way to quickly provide catheter-based procedures to patients, the chance they’ll die or be severely disabled is 90%. That’s just not acceptable. This is a moral obligation.”
Learn more about the UCLA Health Comprehensive Stroke Center.
Related:
UCLA doctor performs world’s first robotic embolization




