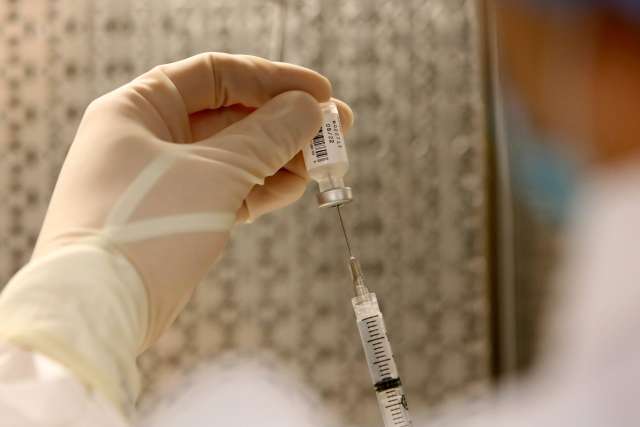
Kelsey Brockway has had a lifelong fear of needles. As a child, she dreaded going to the doctor for her annual vaccines, which left her feeling lightheaded, tired and sore from the injection.
Even as she matured, her fear of needles never left her, she says.
Earlier this year, when the COVID-19 vaccines became widely available, Brockway, now 27, convinced herself she didn’t need the vaccine: She was young, in good health and got tested often for her job.
“Inside, I knew I wasn’t getting the vaccine because I’m afraid of the needle, but I would tell people I wanted to see more research to make sure the vaccine is safe, or some kind of funny way to keep pushing it off,” she says.
Brockway is not alone. A recent study in the United Kingdom found that about 25% of adults and up to 50% of adolescents and 63% of children screen positive for needle anxiety, or trypanophobia, which experts say is playing out in COVID-19 vaccine hesitancy throughout the world.
The study correlates with what health professionals at UCLA Health observe about vaccine hesitancy, says Brenda Bursch, PhD, and reveals a surprising statistic: Successful treatment of needle anxiety could boost COVID-19 vaccine rates by 10%.
Given the need to boost the vaccination rate as the pandemic again surges, this could make a significant difference.
“It’s a huge number,” says Dr. Bursch, a professor of clinical psychiatry and pediatrics at UCLA’s David Geffen School of Medicine.
Difficult to talk about
Dr. Bursch notes the stigma associated with phobias is one reason the topic is rarely discussed.

“If you are somebody who otherwise prides themselves on being stoic or being able to handle stress or a high-pressure job, needle anxiety could feel incongruous to your personality,” says Dr. Bursch. “So, I think it’s not something people talk about frequently.”
Eric Curcio, MD, an associate program director of the combined internal medicine and pediatrics training program at UCLA Health, co-founded UCLA’s Needle Anxiety Program, designed primarily for medically complex patients with cognitive limitations. Such patients are referred to the program by their UCLA Health primary care physician or specialist. Since the program’s inception five months ago, his team has treated about 50 patients with a severe fear of needles.
“These are people who are having full-blown panic attacks just at the thought of getting blood drawn or seeing a needle, and we do see plenty of that with the COVID-19 vaccine,” Dr. Curcio says.

“We’ve seen quite a few patients who weren’t getting the COVID vaccination and weren’t forthcoming with their doctor, saying they needed more time to think about it or there’s not enough research yet,” he says. “But when we dig deeper, we find out these patients, consciously or subconsciously, are avoiding the vaccine because of the needle itself.”
Dr. Curcio says the U.K. study aligns with what he sees in his practice.
“Of that 25%, maybe only 10% avoid to a point of severity where they’re skipping doctor appointments, skipping bloodwork or skipping vaccines,” he says. “This starts adding up. Even 5% of billions of people is a big sector of the population.”
Symptoms and causes vary
The U.K. study reveals needle anxiety occurs in populations around the world, with a higher prevalence in children and teens, women, and Black and Asian ethnic groups. Symptoms can include dizziness, lightheadedness, a sudden drop in blood pressure, panic attacks or fainting.
“It varies from person to person, so thinking about, talking about or seeing a needle, seeing somebody get injected — any of that can be disturbing for some people,” Dr. Bursch says. “Other people can handle it as long as the needle is not going toward them.”
The fear may be rooted in a traumatic childhood experience, it may be genetic or learned from one’s parent’s fears, Dr. Bursch says.
Addie Bortz, a clinical psychology resident at the Jane and Terry Semel Institute for Neuroscience and Human Behavior at UCLA, says needle anxiety is prevalent with the inpatient pediatric population with which she works. Much of it, she says, is due to repeated exposure to unpleasant procedures.
“Even just one negative experience with a procedure, including an injection or IV placement, can really prime kids for future anticipatory anxiety for any sort of additional injection or procedure,” Bortz says.
For Brockway, no childhood trauma was involved, just a general dislike of needles. “I think over the years I just built up angst,” she says.

For patients such as Brockway, needle anxiety can be addressed by providing a comfortable environment, talking to them about their fears or distracting them by showing a music video as the vaccine is being administered, Dr. Curcio says. For those who require a greater level of distraction, a chilled, vibrating massager is often used in conjunction with the topical numbing cream lidocaine to dull any pain.
For severe cases, referral to a mental health professional may be warranted. For those unable to learn self-management skills, anxiety medication is occasionally used in this subspecialty clinic. Dr. Curcio notes that as patients begin to have positive experiences, their fear of needles usually diminishes.
“It’s important to remember it’s not the pain that’s driving this fear, it’s fear that’s driving this,” says Dr. Curcio.
Incorporating exposure therapy
A research-based approach called exposure therapy has had good results in patients with varying degrees of needle anxiety, Dr. Bursch says. The treatment involves habituating a patient’s brain by inducing a state of relaxation and exposing the patient, gradually, to a needle. For those who become light-headed, it is helpful to tighten one’s muscles and elevate one’s feet to avoid a sudden drop in blood pressure.
For some people, even looking at a photo of a needle could be problematic, Dr. Bursch says. Those individuals might first look at a cartoon of a needle or a similar shape and then progress to more realistic photos before practicing with an actual needle.
Patients at the more severe end of the phobia might need professional assistance or additional interventions, but those with mild needle anxiety can try a self-help approach using the same steps, she says.
Bortz says she has used exposure therapy effectively with her patients.
“They just have to be identified and have the right care plan in place and it usually has favorable outcomes,” she says.
On vaccination day, it’s important to have an action plan. That could include asking to wait for your vaccine away from other patients being vaccinated, asking to put your feet up, or requesting the needle be hidden from view when the shot is administered.
“Anything you know will help should be shared with the person delivering the shot so they can be your ally,” Dr. Bursch says.
Distraction techniques also can be helpful, she says. Do a word puzzle. Bring along somebody to support you, to tell jokes or rub your back, which can release comforting substances in your body.
Once the vaccination is over, reward yourself — and go big.
“This is a big deal that you overcame this fear, and it should be exciting or rewarding enough so when you’re having second thoughts it will help get you through a little easier,” Dr. Bursch says.
Changing her perspective
Last spring, as COVID-19 vaccinations began to ramp up, Brockway knew that, eventually, she would have to get the vaccine for her job.
After she admitted her fear of needles to a friend who works at UCLA Health, she was directed to hackthevax.org, an initiative to raise awareness about needle anxiety that was started by licensed clinical psychologist Jody Thomas, a former trainee of Dr. Bursch’s.
When Brockway learned others have the same fear, it changed her perspective.
“That totally made me go, ‘OK, I can be stronger than the vaccine,” Brockway says. “To know that I’m not in this alone, but also to know that this is normal, made me feel comfortable in getting the vaccination.”
Brockway says the shot itself was so easy she didn’t even realize she had been poked. Three weeks later, she had her second dose and now makes a point of telling others who fear needles about her positive experience.
“I know I’m just one small person in the grand scheme of things, but the more people who get vaccinated, the less chance the virus has of spreading,” Brockway says. “It was like a simple math equation once I got over the scary part.”
For information on the UCLA Anxiety Disorders Program visit semel.ucla.edu/adc
For information on UCLA Health’s Needle Anxiety Program, call 310-315-8900.
Jennifer Karmarkar is the author of this article.
Related articles
COVID vaccine and kids: What you need to know
‘Confía en la ciencia’ video promotes vaccine confidence in L.A. communities
COVID vaccines for people with disabilities: Building confidence to get the shot