Parathyroid Surgery Benefits
Find Your Care
We deliver effective, minimally invasive treatments in a caring environment. Call 310-267-7838 to connect with an expert in endocrine surgery.
Benefits of parathyroid surgery at UCLA in Los Angeles, California
Clinical signs & symptoms | Background | Improved bone health | Reduced risk of kidney stones | Improved quality of life | Primary hyperparathyroidism & hypertension | Primary hyperparathyroidism, diabetes & obesity | Primary hyperparathyroidism, cardiovascular disease, & premature death | Special case: Parathyroid surgery in the elderly | Conclusion | Summary | References
Primary hyperparathyroidism: Clinical signs and symptoms
Primary hyperparathyroidism is a disease of calcium imbalance. Because calcium is an important regulator of many cellular functions in all of the body’s organ systems, the clinical manifestations of primary hyperparathyroidism range widely (1). Classically, medical students are taught the following rhyme to recall the effects of excess blood calcium levels:
- Bones – Parathyroid bone disease, osteoporosis, fractures
- Stones – Kidney stones
- Moans – Abdominal pain, nausea, constipation, pancreatitis, peptic ulcer disease
- Groans – Muscle weakness, pain in the muscles and joints
- Neuropsychiatric overtones – Fatigue, delirium, depression, memory loss
When queried about symptoms of hyperparathyroidism, about 95% of individuals with the disease do have one or more of the above complaints (2). That said, it is important to note that many of the symptoms listed above are nonspecific. In other words, the symptoms can be caused by a number of other conditions unrelated to the parathyroid glands. These diagnoses include chronic fatigue syndrome, fibromyalgia, and depression, just to name a few.
Though the benefits of parathyroid surgery are increasingly well-defined, it is not a panacea. However tempting the concept may be, it is not realistic for patients to believe that parathyroid surgery will cure all of a their ills, nor is it appropriate for physicians to create that expectation. Patients who are promised a miracle cure for any condition should exercise great caution (Information about healthy web surfing) from the U.S. National Library of Medicine and the National Institutes of Health).
As is true for most medical treatments, the benefits of parathyroid surgery vary in how well the scientific literature supports them. Certain benefits are clearly established, and others less so. Below, we review the evidence behind health improvements following parathyroid surgery, from the strongest data to the weakest (Figure 1).
Figure 1. Strength of evidence behind potential benefits of parathyroid surgery

Background: The NIH criteria for surgery in asymptomatic primary hyperparathyroidism
In developed nations, the routine of use laboratory testing and imaging studies has resulted in the identification of two distinct patient populations for many disease processes: symptomatic patients (those who are noticeably suffering from the disease and would clearly benefit from treatment), and asymptomatic patients (those who are unaware of any abnormality). Physicians are generally cautious in recommending surgery for asymptomatic patients, with the idea being that it is hard to make a patient better if s/he is already feeling fine. Recommending surgery for asymptomatic patients, therefore, rests on the clear demonstration of future health benefits and/or the avoidance of problems down the line.
With this in mind, the National Institutes of Health developed a list of criteria for surgery in primary hyperparathyroidism (3). In 2002, parathyroid surgery was recommended for asymptomatic patients meeting one or more of the following criteria:
- Blood calcium level more than 1.0 mg/dL above normal
- 24-hour urinary calcium excretion greater than 400 mg/day
- Kidney function reduced by 30% below normal
- Bone mineral density reduced by 2.5 standard deviations below young, healthy controls
- Age less than 50
It is important to note that, in the development of these criteria, only patients with kidney stones and obvious parathyroid bone disease were considered symptomatic. Muscular and neuropsychiatric symptoms, though common, are often considered too vague and difficult to measure systematically. For this reason, these symptoms have frequently been disregarded in prior articles, which is unfortunate since many patients may benefit from parathyroid surgery in the realm of improved quality of life (discussed below). For the sake of simplicity, hereafter we will refer to patients meeting NIH criteria for surgery as having severe parathyroid disease, and those not meeting criteria as having mild disease.
Improved bone health following parathyroid surgery – Strongest evidence
Improvements in bone mineral density following parathyroid surgery are very well established, and patients can routinely expect these benefits soon after surgery.
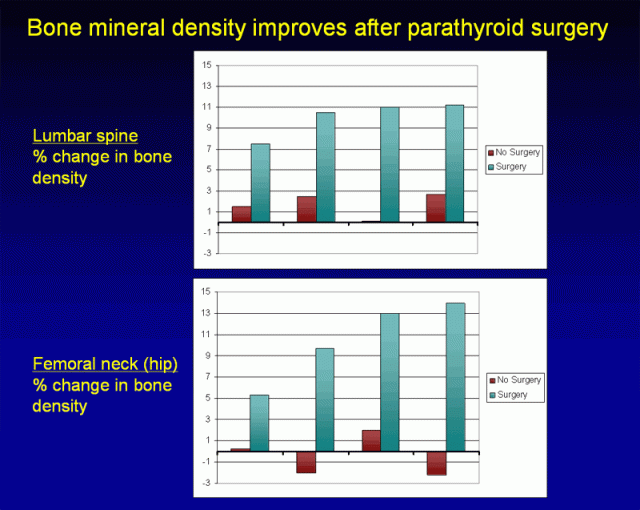
The single most important article on this topic was written by Silverberg and associates from Columbia University; their findings are represented in Figure 2 > (4).
They reported that parathyroid surgery for patients with severe primary hyperparathyroidism resulted in significant increases in bone mineral density that were measurable 1 year after surgery and continued for the next 10 years.
A related article examined changes in bone mineral density in patients with mild parathyroid disease (5).
Figure 2. Bone mineral density improves after parathyroid surgery. Patients having surgery are shown in teal, patients not having surgery are shown in burgundy. Figures show changes in bone density at 1, 4, 7, and 10 years after surgery. Parathyroid surgery leads to prompt increases in bone density in both the spine and hip. These improvements continue for 10 years after surgery. (Adapted from Silverberg, NEJM 1999)
The findings appear in Figure 3.
Nakaoka and associates demonstrated that all patients with primary hyperparathyroidism experience improvements in bone health after parathyroid surgery – this was equally true for patients with mild disease and severe disease.
A more recent article studied fracture risk in patients with primary hyperparathyroidism.
Patients undergoing parathyroid surgery experienced a significant reduction in the risk of fractures, particularly those involving the hip(6).
Reduced risk of kidney stones following parathyroid surgery – Strongest evidence
In the Silverberg article mentioned above, parathyroid surgery was found to completely eliminate future episodes of kidney stones. In contrast, most of the patients in their study who did not undergo surgery continued to have stone events.
Figure 3. Parathyroid surgery improves bone mineral density in all patients with primary hyperparathyroidism. Asymptomatic patients meeting NIH criteria for parathyroid surgery (biochemically severe disease, shown in teal) gain bone mass after parathyroid surgery. The same is true for patients not meeting NIH criteria for parathyroid surgery (biochemically mild disease, shown in burgundy). Bone density measurements were taken before and one year after parathyroid surgery. (Adapted from Nakaoka, JCEM 2000)
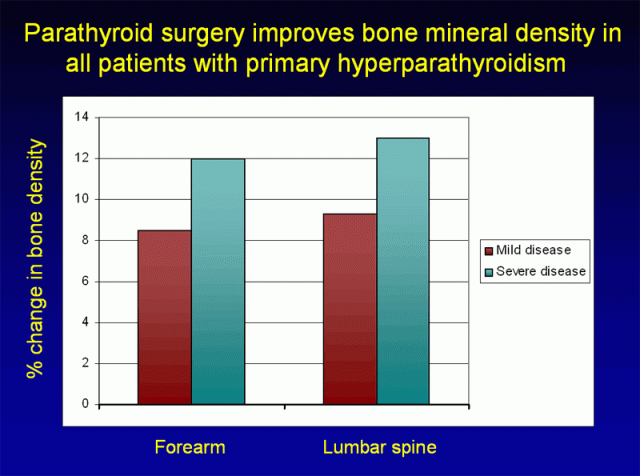
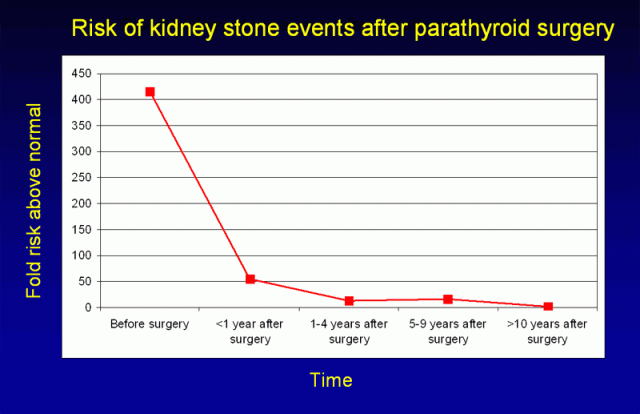
Figure 4 shows results from a large Danish study examining kidney stone events in patients undergoing parathyroid surgery (7).
The risk of future stone episodes decreased dramatically soon after surgery, though the level of risk did not reach normal levels until several years later.
Therefore, patients with kidney stones who undergo parathyroid surgery can expect major improvements in this area, but a certain number may continue to form new stones for a few years afterwards.
Figure 4. Reduction in kidney stone events after parathyroid surgery. Immediately prior to surgery, the risk of stone events is approximately 400 times normal. That risk rapidly declines during the first year following surgery, though a return to completely normal risk levels takes several additional years. (Adapted from Mollerup, BMJ 2002).
Improved quality of life following parathyroid surgery – Strong evidence
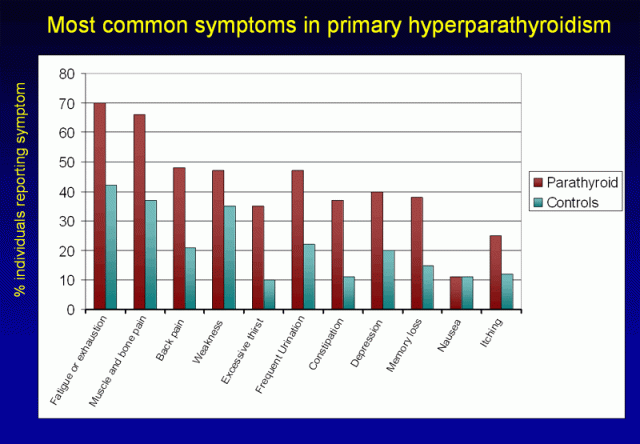
As mentioned above, the majority of patients with primary hyperparathyroidism do report symptoms when they are asked the right questions (2, 8). The most common symptoms are shown in
Figure 5.
They include fatigue, exhaustion, pain in the muscles and bones, weakness, frequent urination, constipation, depression, and others.
Figure 5. Most common symptoms in primary hyperparathyroidism. Individuals with primary hyperparathyroidism (shown in burgundy) are more likely to suffer from the symptoms listed above when compared to individuals without parathyroid disease (shown in teal). (Adapted from Chan, Ann Surg 1995; and Eigelberger Ann Surg 2004)
Eigelberger and associates from the University of California, San Francisco compared the frequency of symptoms in patients with mild parathyroid disease and severe disease
( Figure 6).
They found that all patients with primary hyperparathyroidism were equally likely to suffer from symptoms, and that the majority of patients (approximately 70%) reported improvement in their symptoms after parathyroid surgery (Figure 7).
Therefore, it appears that symptom frequency and severity in primary hyperparathyroidism have no clear relationship with the calcium level or other biochemical markers.
Even patients with minor laboratory abnormalities frequently experience symptoms.
Figure 6. Symptom frequency is not related to disease severity. Among individuals with primary hyperparathyroidism, those with biochemically mild disease (shown in burgundy) are equally likely to experience symptoms when compared to those with biochemically severe disease (shown in teal). (Adapted from Eigelberger Ann Surg 2004)
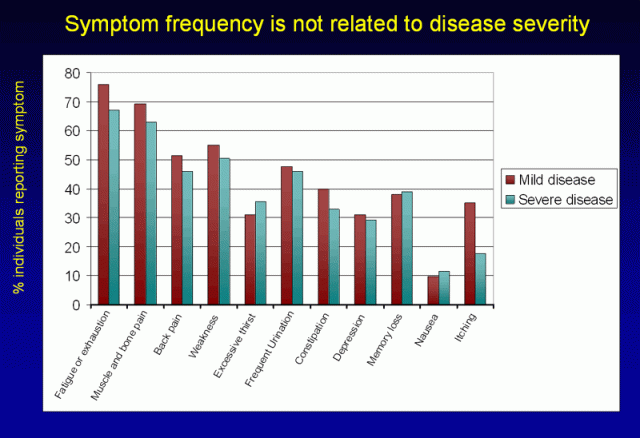
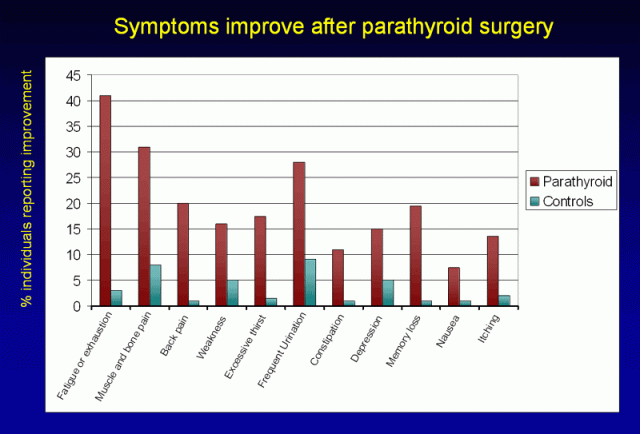
Figure 7. Symptoms improve after parathyroid surgery. After surgery, individuals with primary hyperparathyroidism (shown in burgundy) experience a marked decrease in the symptoms listed above when compared to individuals without parathyroid disease, who underwent a thyroid operation (shown in teal). Overall, approximately 70% of patients who undergo parathyroid surgery experience improvement in one or more of their symptoms. Equivalent rates of improvement are seen for patients with biochemically mild disease (those not meeting NIH criteria for surgery) and those with biochemically severe disease (those meeting NIH criteria for surgery). (Adapted from Chan, Ann Surg 1995; and Eigelberger Ann Surg 2004)
A small number of well-designed studies have examined quality of life measures in patients with parathyroid disease. Rao and associates noted mild but significant improvements in health related quality of life following parathyroid surgery (9). In another recent study, no such benefits were observed (10). Both of these studies have been criticized because quality of life was measured using generic survey tools rather than questionnaires specifically aimed at symptoms of parathyroid disease. Indeed, when disease-specific tools are used, the quality of life benefit of parathyroid surgery appears to be much greater (11). Controversy remains on this topic.
Our experience at UCLA is compatible with the findings from UCSF: about two-thirds of our patients report improvements in quality of life following parathyroid surgery. In most cases, the changes are noted within days or a few weeks of surgery.
Primary hyperparathyroidism and hypertension (high blood pressure) – Weak evidence
Patients with primary hyperparathyroidism appear more likely to have hypertension than those who do not. However, no clear cause-and-effect relationship between the two processes has been established, and parathyroid surgery does not appear to reliably improve blood pressure (12-14).
Primary hyperparathyroidism, diabetes, and obesity – Weak evidence
In some studies, higher rates of type 2 diabetes and obesity have been found in association with primary hyperparathyroidism (15-19). To date, there has been no systematic evidence to suggest that parathyroid surgery reverses these associated conditions.
Primary hyperparathyroidism, cardiovascular disease, and premature death – Weak evidence
Several large scale studies performed in Sweden and Denmark have demonstrated a significantly increased risk of death from cardiovascular disease (stroke, heart attack, heart failure, and abnormal heart rhythms) in patients with primary hyperparathyroidism (20-23) . These studies utilized national health databases covering many thousands of individuals. In some cases, parathyroid surgery was shown to bring patients back down to normal levels of risk (24) .
That said, similar studies performed in the United States have failed to replicate these results (25) , calling into question the generalizability of the findings. The question of whether primary hyperparathyroidism adversely affects cardiovascular health, therefore, remains unanswered. The Scandinavian studies have raised some intriguing possibilities that require further study.
Parathyroid surgery in the elderly: Special case
Several studies have indicated that elderly patients with primary hyperparathyroidism experience significant delays before being offered surgery (26, 27) . Almost half of elderly patients in one study experienced mental impairment as a result of their disease. At expert centers, parathyroid surgery involving patients older than 80 years is both effective and uncomplicated (28) . Elderly patients enjoy the same benefits from parathyroid surgery that younger patients do in the areas of health related quality of life and bone density. A growing body of literature suggests that elderly individuals experience improvements in cognitive function and mental status after parathyroid surgery (29) .
Conclusion: Which patients with primary hyperparathyroidism should have surgery?
The 2002 NIH criteria set out to define a group of patients with severe parathyroid disease who require surgery and a separate group of patients with mild disease who do not. However, as reviewed above, these two groups are indistinguishable in many respects. Patients with severe disease and mild disease are equally likely to have symptoms of primary hyperparathyroidism and are equally likely to benefit from parathyroid surgery.
This fact has led some experts and national physician organizations to conclude that all patients with primary hyperparathyroidism should be considered for parathyroid surgery(30, 31).
(See the 2005 position statement on primary hyperparathyroidism jointly written by the American Association of Clinical Endocrinologists and American Association of Endocrine Surgeons (PDF) >)
Most physicians would agree that the decision to proceed with parathyroid surgery is dependent on the balance of risk and benefit for each individual patient. We recommend that people who are diagnosed with primary hyperparathyroidism discuss this option with an endocrinologist or endocrine surgeon, when appropriate.
Major advances in surgical technique, particularly the advent of focused (minimally invasive) parathyroid surgery, have made parathyroid surgery a better option for increasing numbers of people worldwide
(Figure 8).
Growing awareness of the health benefits of parathyroid surgery has also driven this trend, which reflects a general shift in the risk-benefit ratio in favor of surgery.
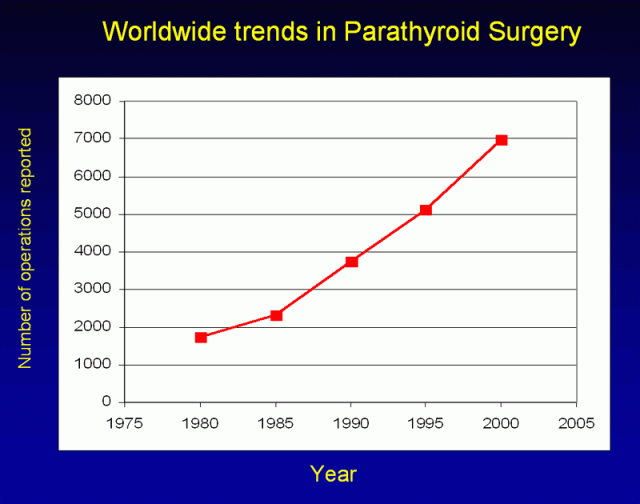
Figure 8. Worldwide trends in parathyroid surgery. Members of the International Association of Endocrine Surgeons have reported increasing rates of parathyroid surgery across all continents. (Adapted from Sackett, Arch Surg 2002)
Benefits of Parathyroid Surgery
Video: Dr. Michael Yeh discusses the benefits of parathyroid surgery

Summary points
- Primary hyperparathyroidism affects many organ systems of the body.
- Most patients with primary hyperparathyroidism have significant health problems associated with the condition.
- Individuals with mild parathyroid disease and severe parathyroid disease are very similar, and individuals in both categories are likely to benefit from parathyroid surgery.
- Improvements in bone health after parathyroid surgery are consistent and well-established.
- Reductions in kidney stone events after parathyroid surgery are consistent and well-established.
- About 70% of people experience improvements in health-related quality of life after parathyroid surgery.
- Other conditions associated with primary hyperparathyroidism continue to be investigated.
- Elderly individuals may benefit significantly from parathyroid surgery and should not be denied this option.
- Improvements in surgical technique have made parathyroid surgery a better option for many people worldwide.
References
- Marx SJ. Hyperparathyroid and hypoparathyroid disorders. N Engl J Med, 343: 1863-1875, 2000.
- Chan AK, Duh QY, Katz MH, Siperstein AE, and Clark OH. Clinical manifestations of primary hyperparathyroidism before and after parathyroidectomy. A case-control study. Ann Surg, 222: 402-412; discussion 412-404, 1995.
- Bilezikian JP, Potts JT, Jr., Fuleihan Gel H, Kleerekoper M, Neer R, Peacock M, Rastad J, Silverberg SJ, Udelsman R, and Wells SA. Summary statement from a workshop on asymptomatic primary hyperparathyroidism: a perspective for the 21st century. J Clin Endocrinol Metab, 87: 5353-5361, 2002.
- Silverberg SJ, Shane E, Jacobs TP, Siris E, and Bilezikian JP. A 10-year prospective study of primary hyperparathyroidism with or without parathyroid surgery. N Engl J Med, 341: 1249-1255, 1999.
- Nakaoka D, Sugimoto T, Kobayashi T, Yamaguchi T, Kobayashi A, and Chihara K. Prediction of bone mass change after parathyroidectomy in patients with primary hyperparathyroidism. J Clin Endocrinol Metab, 85: 1901-1907, 2000.
- VanderWalde LH, Liu IL, O'Connell TX, and Haigh PI. The effect of parathyroidectomy on bone fracture risk in patients with primary hyperparathyroidism. Arch Surg, 141: 885-889; discussion 889-891, 2006.
- Mollerup CL, Vestergaard P, Frokjaer VG, Mosekilde L, Christiansen P, and Blichert-Toft M. Risk of renal stone events in primary hyperparathyroidism before and after parathyroid surgery: controlled retrospective follow up study. Bmj, 325: 807, 2002.
- Eigelberger MS, Cheah WK, Ituarte PH, Streja L, Duh QY, and Clark OH. The NIH criteria for parathyroidectomy in asymptomatic primary hyperparathyroidism: are they too limited? Ann Surg, 239: 528-535, 2004.
- Rao DS, Phillips ER, Divine GW, and Talpos GB. Randomized controlled clinical trial of surgery versus no surgery in patients with mild asymptomatic primary hyperparathyroidism. J Clin Endocrinol Metab, 89: 5415-5422, 2004.
- Bollerslev J, Jansson S, Mollerup CL, Nordenstrom J, Lundgren E, Torring O, Varhaug JE, Baranowski M, Aanderud S, Franco C, Freyschuss B, Isaksen GA, Ueland T, and Rosen T. Medical observation, compared with parathyroidectomy, for asymptomatic primary hyperparathyroidism: a prospective, randomized trial. J Clin Endocrinol Metab, 92: 1687-1692, 2007.
- Pasieka JL, Parsons LL, Demeure MJ, Wilson S, Malycha P, Jones J, and Krzywda B. Patient-based surgical outcome tool demonstrating alleviation of symptoms following parathyroidectomy in patients with primary hyperparathyroidism. World J Surg, 26: 942-949, 2002.
- Fardella C and Rodriguez-Portales JA. Intracellular calcium and blood pressure: comparison between primary hyperparathyroidism and essential hypertension. J Endocrinol Invest, 18: 827-832, 1995.
- Lind L, Hvarfner A, Palmer M, Grimelius L, Akerstrom G, and Ljunghall S. Hypertension in primary hyperparathyroidism in relation to histopathology. Eur J Surg, 157: 457-459, 1991.
- Sancho JJ, Rouco J, Riera-Vidal R, and Sitges-Serra A. Long-term effects of parathyroidectomy for primary hyperparathyroidism on arterial hypertension. World J Surg, 16: 732-735; discussion 736, 1992.
- Cardenas MG, Vigil KJ, Talpos GB, Lee MW, Peterson E, and Rao DS. Prevalence of type 2 diabetes mellitus in patients with primary hyperparathyroidism. Endocr Pract, 14: 69-75, 2008.
- Khaleeli AA, Johnson JN, and Taylor WH. Prevalence of glucose intolerance in primary hyperparathyroidism and the benefit of parathyroidectomy. Diabetes Metab Res Rev, 23: 43-48, 2007.
- Procopio M, Magro G, Cesario F, Piovesan A, Pia A, Molineri N, and Borretta G. The oral glucose tolerance test reveals a high frequency of both impaired glucose tolerance and undiagnosed Type 2 diabetes mellitus in primary hyperparathyroidism. Diabet Med, 19: 958-961, 2002.
- Siilin H, Rastad J, Ljunggren O, and Lundgren E. Disturbances of calcium homeostasis consistent with mild primary hyperparathyroidism in premenopausal women and associated morbidity. J Clin Endocrinol Metab, 93: 47-53, 2008.
- Taylor WH and Khaleeli AA. Coincident diabetes mellitus and primary hyperparathyroidism. Diabetes Metab Res Rev, 17: 175-180, 2001.
- Hedback G and Oden A. Increased risk of death from primary hyperparathyroidism--an update. Eur J Clin Invest, 28: 271-276, 1998.
- Nilsson IL, Wadsten C, Brandt L, Rastad J, and Ekbom A. Mortality in sporadic primary hyperparathyroidism: nationwide cohort study of multiple parathyroid gland disease. Surgery, 136: 981-987, 2004.
- Vestergaard P and Mosekilde L. Cohort study on effects of parathyroid surgery on multiple outcomes in primary hyperparathyroidism. Bmj, 327: 530-534, 2003.
- Vestergaard P and Mosekilde L. Fractures in patients with primary hyperparathyroidism: nationwide follow-up study of 1201 patients. World J Surg, 27: 343-349, 2003.
- Vestergaard P, Mollerup CL, Frokjaer VG, Christiansen P, Blichert-Toft M, and Mosekilde L. Cardiovascular events before and after surgery for primary hyperparathyroidism. World J Surg, 27: 216-222, 2003.
- Wermers RA, Khosla S, Atkinson EJ, Grant CS, Hodgson SF, O'Fallon WM, and Melton LJ, 3rd. Survival after the diagnosis of hyperparathyroidism: a population-based study. Am J Med, 104: 115-122, 1998.
- Chen H, Parkerson S, and Udelsman R. Parathyroidectomy in the elderly: do the benefits outweigh the risks? World J Surg, 22: 531-535; discussion 535-536, 1998.
- Kebebew E, Duh QY, and Clark OH. Parathyroidectomy for primary hyperparathyroidism in octogenarians and nonagenarians: a plea for early surgical referral. Arch Surg, 138: 867-871, 2003.
- Egan KR, Adler JT, Olson JE, and Chen H. Parathyroidectomy for primary hyperparathyroidism in octogenarians and nonagenarians: a risk-benefit analysis. J Surg Res, 140: 194-198, 2007.
- Coker LH, Rorie K, Cantley L, Kirkland K, Stump D, Burbank N, Tembreull T, Williamson J, and Perrier N. Primary hyperparathyroidism, cognition, and health-related quality of life. Ann Surg, 242: 642-650, 2005.
- The American Association of Clinical Endocrinologists and the American Association of Endocrine Surgeons position statement on the diagnosis and management of primary hyperparathyroidism. Endocr Pract, 11: 49-54, 2005.
- Utiger RD. Treatment of primary hyperparathyroidism. N Engl J Med, 341: 1301-1302, 1999.
The Benefits of parathyroid surgery are improved bone health, reduced risk of kidney stones and improved quality of life. About 70 percent of people experience improvements in health-related quality of life after parathyroid surgery. Primary hyperparathyroidism is a disease of calcium imbalance.