Clinical Training Program
Residency training in anesthesiology at UCLA is a four-year program. Each resident begins as a intern (PGY-1) during our tailored Clinical Base Year, followed by three years at the Ronald Reagan UCLA Medical Center (RRUMC) and affiliated sites including Olive View Medical Center, Children's Hospital Los Angeles, Long Beach Memorial Medical Center, and the Veteran's Administration Greater Los Angeles Medical Center.
Clinical Base Year (PGY-1)

The medicine-based curriculum focuses on preparation for future training in anesthesiology. Rotations on medical/surgical units take place primarily at the West Los Angeles VA Hospital, with a one-month introduction to clinical anesthesiology and additional subspecialty rotations at RRUMC.
The year is organized into two to four-week blocks. Rotations at the VA Medical Center include:
- General medicine wards
- Medical Consult service
- Pre-operative service
- Emergency Medicine
- Intensive Care Units (medical and surgical)
- Surgical co-management service
- Surgical night float
- Head and neck rotation
- Specialty Consult Service (cardiology, pulmonary, renal, infectious disease, endocrine)
Finally, each intern embarks on an anesthesiology rotation in the main operating rooms of RRUMC during one of the last four blocks. This rotation is supervised by UCLA anesthesiology faculty on a one-to-one basis, and includes daily didactic lectures and at least four simulator training sessions. Rotations at the VA are supervised by Dr. Satya Patel.
CA-1 – CA-3 Years
General Anesthesiology/Main Operating Room
The heart of our residency training occurs at RRUMC and Mattel Children’s Hospital. Over 50,000 anesthetics are performed at UCLA annually in all surgical subspecialties, including growing numbers of cases outside of the operating room. RRUMC has 23 operating rooms, six cardiac catheterization labs, and interventional radiology/CT suites located on the same floor. Many of our patients have been referred to UCLA from outside hospitals because of their complex conditions.
UCLA is one of the most prominent adult and pediatric organ transplantation centers in the world. RRUMC is a Level 1 trauma center with two helipads and two fully-equipped ER trauma bays with CT-imaging capabilities where up to four victims of major trauma can be treated simultaneously.
Pediatric Anesthesiology
The Mattel Children's Hospital, named among the top pediatric medical centers in the United States by U.S. News & World Report, provides full-service healthcare to babies and children with cardiac, liver, kidney, neurologic, and other diseases, including high-risk neonates. Additionally, Children's Hospital of Los Angeles offers a six-week pediatric anesthesiology rotation for our residents.
Obstetric Anesthesiology
RRUMC houses a busy Labor and Delivery Unit with an adjacent 28-bed neonatal ICU. Approximately 40 percent of our obstetric cases are high-risk, including patients with cardiac, liver, and neurologic disease. The overall cesarean section rate is approximately 30 percent. Residents also gain experience in obstetric anesthesiology in a fast-paced, private-practice setting at Long Beach Memorial Hospital.
Cardiothoracic Anesthesiology
Both adult and pediatric cardiac surgeries are performed at UCLA, with the use of transesophageal echocardiographic monitoring by the anesthesiology team in nearly every case. Many cases involve heart or lung transplantation, complex congenital heart disease, or acquired valvular pathology. Additionally, residents gain strong experience in anesthesiology for adult vascular and thoracic surgery as well as pediatric thoracic surgery; many cases require one-lung ventilation.
Neuroanesthesia
Our neuroanesthesia service provides anesthesia for intracerebral masses, complex aneurysms, and other intracranial pathology. Experiences include advanced techniques such as the “asleep-awake-asleep anesthetic” and the full spectrum of neurologic monitoring techniques.
Anesthesia for Ambulatory Surgery

UCLA has two outpatient surgery centers. The 200 Medical Plaza Ambulatory Surgery Center houses ten operating rooms plus four procedure rooms for a high-volume, rapid-turnover outpatient experience. The Santa Monica-UCLA Surgery Center, the health system’s first to be designed as LEED Gold for sustainability, contains eight operating rooms and two radiation oncology suites. At these surgery centers, education in techniques for prompt recovery from anesthesia and the special considerations of outpatient care are emphasized, and residents gain experience in regional nerve blocks.
Regional Anesthesiology
UCLA residents gain an outstanding training experience in regional anesthesia at the Olive View Medical Center, the Santa Monica-UCLA Medical Center and Orthopaedic Hospital, and the West Los Angeles VA. Use of ultrasound guidance and peripheral catheter techniques are taught by dedicated regional anesthesiology specialists.
Pain Medicine
Our Acute Pain Service provides excellent experience in regional anesthesia for pain control after thoracic, abdominal, and orthopedic surgeries, while the Pain Medicine rotation teaches the art of new patient evaluation and the full range of interventional treatments for chronic pain. Interventional procedures are performed at Santa Monica-UCLA Medical Center and Orthopaedic Hospital.
Anesthesia for Ophthalmic Surgery
Training in anesthesia for ambulatory ophthalmic surgery takes place at the Jules Stein Eye Institute (JSEI), with five operating rooms for adult and pediatric patients. Consistently ranked as the best eye care center in the Western United States by U.S. News & World Report and Ophthalmology Times, the JSEI offers a full range of services. We provide preanesthetic evaluation and care during anesthesia and recovery for all types of ophthalmic surgical procedures in patients from newborns through the elderly, with anesthetic techniques that promote rapid recovery.
Intensive Care Medicine
Three intensive care rotations are available for our CA-1 through CA-3 residents, including the Cardiothoracic and Liver Transplant ICUs at RRUMC and the Surgical ICU at the VA. staffed by UCLA anesthesiology faculty.
UCLA Simulation Center
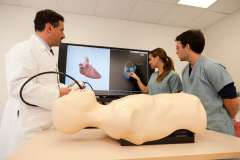
All residents have the opportunity to train on the Human Patient Simulators at the UCLA Simulation Center. Established in 1996 by Dr. Randolph Steadman of our department, the UCLA Simulation Center was the first in Southern California to provide simulation-based training to medical students and residents. This has now become a standard for medical education, surgical training, and healthcare team training. Residents benefit from simulator experience at least four times during their first month of training in anesthesiology, and multiple times throughout their residency for practice in handling critical incident scenarios.
The residency training program in anesthesiology at UCLA provides a diverse and challenging clinical experience. The links below demonstrate examples of typical resident clinical experiences: