Ultrasound-MRI Fusion for Targeted Diagnosis of Prostate Cancer
Introduction
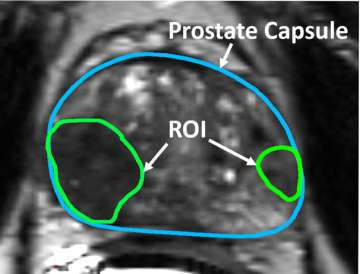
Prostate cancer is the most prevalent cancer in men with ~175,000 confirmed cases per year leading to ~30,000 deaths. Widespread adoption of PSA testing has led to a trend of overdiagnosis with many clinically insignificant lesions considered for treatment. More recently, the development of advanced MRI techniques has facilitated localization of cancerous regions within the prostate (Figure 1), however, accurate biopsies are required to assess the clinical significance of the MRI visible lesion. In addition, there is evidence that MRI underestimates the extent of the cancerous tissue, thus, precision biopsies may improve our ability to quantify the true size of the cancerous lesion. Ultimately our goal is to combine the information provided by both MRI and biopsy to better inform treatment selection.
Figure 1: MRI showing regions of interest (ROI) suspicious for prostate cancer
Ultrasound-MRI Fusion Biopsy with the Artemis Device
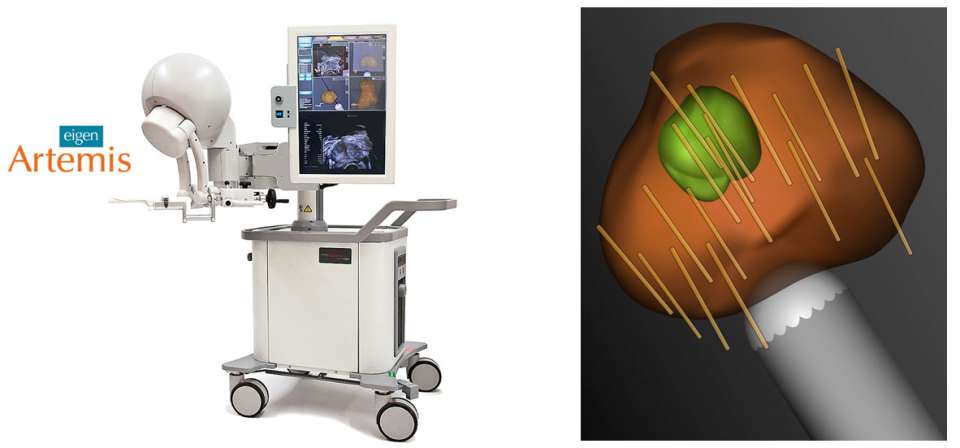
Conventional biopsies are performed in a systematic manner in which tissue samples are acquired throughout the prostate. Consequently, cancerous lesions are frequently missed due to the inability to accurately target the biopsy to regions that are suspicious for cancer. At UCLA we have collaborated with Eigen Corp. in the development of the Artemis device which is capable of targeted biopsy. The Artemis device consists of 3 main parts: a tracking arm, a monitor, and a work station (Figure 2 left). In brief, a conventional ultrasound unit is used to image the prostate trans-rectally. The tracking arm attaches to the ultrasound probe, allowing a capture of the scanned prostate by the processor. From the ultrasound feed, a 3D reconstruction of the prostate is created on the monitor in a near-realtime manner (Figure 2 right). MRI identified regions of interest are then fused with the real-time ultrasound which enables accurate targeting of biopsy needles to the relevant tissue. In addition, systematic biopsy may be taken to assess other regions for cancer.
The Artemis device is now routinely used at UCLA for diagnosing prostate cancer as summarized in the video below.
Current Research
- Cancer Staging – To date we have performed over 4,000 targeted biopsies and by analysis of this data we hope to improve cancer staging and treatment selection.
- Focal Therapy Eligibility - Focal therapy has emerged as method of treating the cancerous lesion while sparing surrounding healthy tissue. It offers an effective treatment for prostate cancer with substantially fewer side-effects than conventional treatments such as radical prostatectomy and radiation therapy. By combing MRI and targeted biopsy data we seek to identify patients that may be treated with focal therapy.
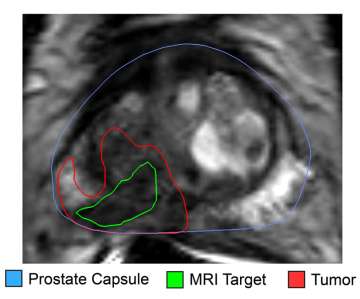
- Treatment Planning – Hight Intensity Focused Ultrasound, Cryotherapy and Focal Laser Ablation are all promising modalities for focal treatment of prostate cancer. We are developing treatment planning techniques for all of these modalities with the aim of improving treatment outcomes and better informing the appropriate treatment modality on a case by case basis. To do so it is essential to quantify the true extent of the cancer which is not possible with MRI alone (Figure 3).




Selected Publications:
Zhang, Z., Wu, H. H., Priester, A., Magyar, C., Afshari Mirak, S., Shakeri, S., ... & Reiter, R. E. (2020). Prostate microstructure in prostate cancer using 3-T MRI with diffusion-relaxation correlation spectrum imaging: validation with whole-mount digital histopathology. Radiology, 192330.
Nassiri, N., Margolis, D. J., Natarajan, S., Sharma, D. S., Huang, J., Dorey, F. J., & Marks, L. S. (2017). Targeted biopsy to detect Gleason score upgrading during active surveillance for men with low versus intermediate risk prostate cancer. The Journal of urology, 197(3), 632-639.
Priester, A., Natarajan, S., Khoshnoodi, P., Margolis, D. J., Raman, S. S., Reiter, R. E., ... & Marks, L. S. (2017). Magnetic resonance imaging underestimation of prostate cancer geometry: use of patient specific molds to correlate images with whole mount pathology. The Journal of urology, 197(2), 320-326.
Filson, C. P., Natarajan, S., Margolis, D. J., Huang, J., Lieu, P., Dorey, F. J., ... & Marks, L. S. (2016). Prostate cancer detection with magnetic resonance‐ultrasound fusion biopsy: the role of systematic and targeted biopsies. Cancer, 122(6), 884-892.
Priester, A., Natarajan, S., Le, J. D., Garritano, J., Radosavcev, B., Grundfest, W., ... & Huang, J. (2014). A system for evaluating magnetic resonance imaging of prostate cancer using patient-specific 3D printed molds. American journal of clinical and experimental urology, 2(2), 127.
Sonn, G. A., Chang, E., Natarajan, S., Margolis, D. J., Macairan, M., Lieu, P., ... & Marks, L. S. (2014). Value of targeted prostate biopsy using magnetic resonance–ultrasound fusion in men with prior negative biopsy and elevated prostate-specific antigen. European urology, 65(4), 809-815.
Sonn, G. A., Natarajan, S., Margolis, D. J., MacAiran, M., Lieu, P., Huang, J., ... & Marks, L. S. (2013). Targeted biopsy in the detection of prostate cancer using an office based magnetic resonance ultrasound fusion device. The Journal of urology, 189(1), 86-92.
Marks, L., Young, S., & Natarajan, S. (2013). MRI–ultrasound fusion for guidance of targeted prostate biopsy. Current opinion in urology, 23(1), 43.
