Guidelines for Travel
Find Your Care
You receive customized, exceptional diabetes treatment and education in a caring environment. Call 310-825-7922 to connect with a diabetes specialist.
General Guidelines
What To Take When Traveling
Carry your diabetes care items in your carry-on bag, not checked in a luggage compartment. Always take double the amount of supplies you think you will need. Items below that are starred should be included in a “mini kit” that you should have readily available:
- Diabetes Medications*
- Vials and/or pens of your long and rapid acting insulins*
- Insulin syringes and/or pen needles* (pack twice as many as you think you may need)
- Glucose monitoring equipment* (meter and strips) – including extra batteries
- Non-perishable snacks*
- Glucose tablets or gel*
- Glucagon Emergency Kit
- A letter stating you have diabetes that specifies:
- Your need for daily injections and that you must carry a supply of medication and syringes
- Any allergies
- Your need for any special foods
(Note: FAA rules have changed in recent years and a letter may or may not be required.)
- Spare prescriptions for medications, syringes and insulin with dosing instructions*
- First-aid medication and supplies:
- Pepto-Bismol, Kaopectate, Imodium
- Dried soup mixes and powdered Gatorade to use if you get sick and need fluids*
- Medical Identification – bracelet or necklace (stating medical diagnosis, allergies and list of medications including insulin) – www.medicalert.org
Precautions
Medication storage - Keep insulin at a temperature range of 40 to 86 degrees Fahrenheit
- Do not pack insulin or medication with your luggage or in airline storage compartments. Airline storage compartments may reach temperature levels below 40 degrees Fahrenheit. If insulin freezes, it will lose effectiveness (although it will not change its appearance).
- Do not store insulin in a car or trunk unless it is stored in an insulated container.
- If the weather is extreme, consider putting your insulin in a wide mouth thermos that is initially rinsed with cold water.
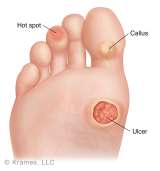
Bring a comfortable pair of walking shoes
- Stack heels and rubber soles are more comfortable than either extremely flat shoes or shoes with slender heels. Leather shoes breathe and hence do not cause your feet to perspire. Consider wearing well-fitted sneakers/athletic shoes with cotton socks. They provide support and a soft-walking surface.
Check your feet daily

- Examine your feet, especially the heels and soles every day.
- If there is redness, consider applying moleskin and discuss with your diabetes team.
- Any break in the skin requires further attention and discussion with your diabetes team.
Consider bringing or purchasing your meal before getting on the plane
- Airlines provide meals for purchase and often offer the choice to pre-order.
- Bring non-perishable snacks. Even the best of plans fail and you could end up stranded overnight in an airport or not liking the food choices that are available. Therefore, you should always have a ready source of food and medicine available. There are a variety of commercial products that travel well: blister packs of crackers and cheese, peanut butter snacks, instant cereal, etc. Consider dried soup mixes and powdered Gatorade to use if you get sick and need fluids.
If you need to avoid drinking the water:
In many countries, the water may be contaminated.
- The following beverages may be safe to drink: boiled water, hot beverages (such as coffee or tea) made with boiled water, canned or bottled carbonated beverages, beer, and wine. You can also purchase water purification bottles and pills in a travel or sport store.
- Ice may be made from unsafe water and should be avoided.
- It is safer to drink from a can or bottle of beverage than to drink from a container that may not be clean.
- In areas where water is contaminated, avoid all but bottled water – and do not brush your teeth with tap water.
- Avoid fresh fruits, fresh vegetables and salads (as these are washed in water). If you peel fruit yourself, it is generally safe.
Consult Your Healthcare Provider for Specific Individual Instruction on Dosage Adjustments
Medication
Always travel with your medications in your carry-on bag. Bring a written list of all prescribed medications in the event that you lose your medications during travel.
Insulin Pumps
Insulin Timing Adjustment
There have been reports of bubbles entering the system and unintended boluses occurring during airline descent and ascent. It is recommended you contact your pump manufacturer for specific directions for your pump or disconnect prior to ascent and descent and inspect tubing and reservoir. Any visible bubbles in the system should be removed prior to reconnecting the device.
Safety Tips
Learn how to obtain medical assistance in an emergency
- Learn enough of the language to request help.
- Hotels in every country have access to English speaking doctors.
- Many credit cards have an emergency service that will provide you with the names of English speaking doctors in many foreign countries.
- Call the U.S. Embassy or the Consulate for additional listings.
- Alert travel companions of the possibility of a low blood glucose. Teach them the signs and symptoms of low blood glucose and give them specific instructions for treating it if you are unable to do it yourself. Teach them how and when to administer Glucagon, if it has been prescribed.
Consider what impact you might experience from hot tubs/whirlpool, sauna or thermal baths
- Check with your diabetes team to see if you can safely use a hot tub or sauna. Individuals with neuropathy, heart disease, circulation problems, high blood pressure, and skin infections are at higher risk for complications.
Determine if you need special immunizations
- Obtain any immunizations needed at least one month before you leave. If they make you ill or you experience side effects, you’ll have time to recover before the trip.
- To find out if you need immunizations, contact the CDC for information:
(404) 332-4555 or http://www.cdc.gov/travel/index.htm or refer to The Yellow Book: The CDC Health Information for International Travel (an in-depth travel reference book published biennially by CDC.