More than 50 million Americans experience allergies. In most cases, the reaction involves mild and localized symptoms, such as sneezing, redness or itchiness. But for about one in 50 people, the allergy will cause a life-threatening reaction called anaphylaxis.
During anaphylaxis — also called allergic or anaphylactic shock — your immune system releases a flood of chemicals that cause your body to go into shock. The most common triggers for anaphylaxis are:
- Food: Approximately 32 million Americans are diagnosed with food allergies — that’s 1 in 10 adults and 1 in 13 children.
- Insect stings: Insect allergies cause at least 100 deaths a year in the United States.
- Medicines: Severe drug reactions affect 10% of the world’s population, with allergies to penicillin being the most common.
Even if you don’t have severe allergies, you likely know or may encounter someone who does. That’s why it’s important to familiarize yourself with basic information about allergies and anaphylaxis. Here’s what you should know:
1. How to recognize the signs of an allergic reaction and anaphylaxis
Symptoms of an anaphylactic reaction can begin anywhere from five to 30 minutes after contact with the allergen. The signs usually affect multiple parts of the body and may include:
- Breathing trouble, with possible wheezing or coughing
- Chest tightness
- Hoarse voice
- Itchy, red rash with hives
- Passing out or feeling faint
- Stomach cramping, nausea or vomiting
- Swelling (in throat or other areas of the body)
2. When to use an epinephrine injector (such as EpiPen® or AUVI-Q®)
The first-line treatment for anaphylaxis is epinephrine (adrenaline). Epinephrine reverses the life-threatening symptoms by relaxing airway muscles and tightening blood vessels. Anyone with known, serious allergies is typically prescribed an auto-injector which delivers epinephrine through a needle during a severe allergic reaction.
For an epinephrine injection to work, it should occur at the first sign of a serious allergic reaction. Even if you aren’t sure whether an allergic reaction warrants epinephrine, it’s better to use it right away. According to the American College of Allergy, Asthma & Immunology, the benefits of epinephrine far outweigh the risk if the dose isn’t needed. An unnecessary dose may cause an increase in heart rate and blood pressure, but epinephrine is metabolized quickly so the effects won’t last long.
3. How to use an auto-injector
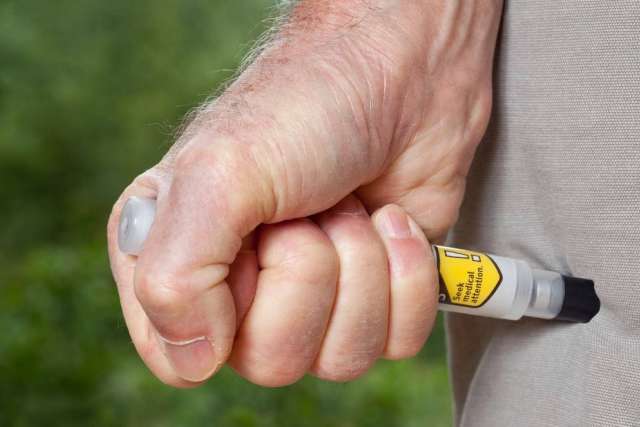
Even if you don’t have allergies, you may need to use an auto-injector on someone else. After removing any safety caps from the device, hold it in your fist, press up against the middle of the outer side of the thigh of the person having a reaction and press the button to inject. Inject it right through clothing when necessary.
Hold the device in place for up to 10 seconds — the exact time required and other specific instructions should be printed on the package.
4. What to do after you give a shot of epinephrine
Some liquid may remain in the device after injection — that’s normal. It doesn’t mean you didn’t give a full dose, and you should not try to use the extra solution. Immediately after giving an injection, call 911 or get the person in anaphylactic shock to the emergency room. Don’t wait, because the effects of the medicine can wear off and result in a second reaction.
If after 15 minutes the symptoms still persist or if a second reaction occurs, you may need to inject another dose of epinephrine — but that requires a second device. Used epinephrine injectors need to be disposed of properly so that pets, children and others cannot access them. Give them to the emergency responders or emergency room personnel to discard.
Reach out to your primary care physician if you have more questions about allergies and anaphylaxis. If you have allergies, UCLA Health offers allergy and immunology specialists who can help you manage your condition.