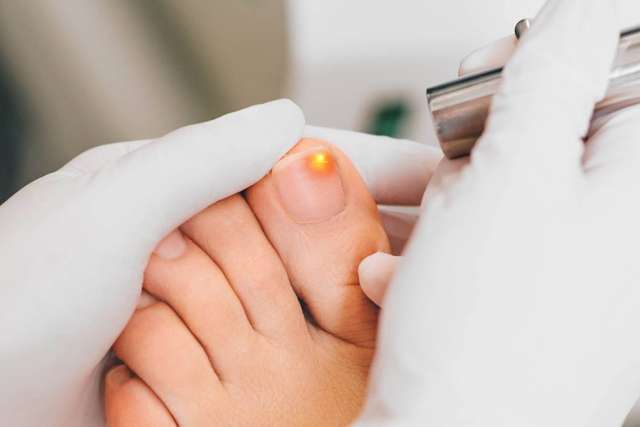
White or yellow spots under the tips of a fingernail or toenail may be the beginning of a common condition known as onychomycosis — nail fungus. If left untreated, nail fungus can cause your nail to discolor, become thick or start to break down. Nail fungus may spread to other nails as well.
By whatever name you call it, it’s a condition that can become especially obvious in the summer, when you swap close-toed shoes for sandals.
Risk factors for nail fungal infections
Toenail fungal infections are more common than fingernail fungal infections. And, while anyone is a potential candidate for toenail fungus, it’s most common in older adults. As we age, blood flow is reduced, which slows nail growth. This could result in dry and brittle nails that crack, creating an entry point for fungi.
You may also be more prone to onychomycosis if you:
- Have a history of athlete’s foot (the fungus can spread to the nail bed)
- Sweat profusely, creating a breeding ground for fungus
- Walk barefoot in warm, damp areas that others use, such as gym showers and swimming pools where fungi can live
- Have nail or skin injuries or conditions that cause changes that allow the fungus to enter the nail bed
- Have diabetes or circulation problems that impact your immune response and nail health
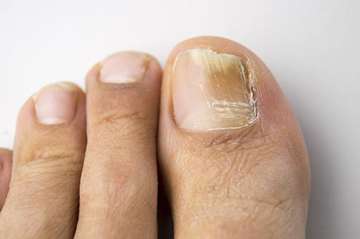
When to see your doctor about nail infections
A mild case of onychomycosis may not be bothersome or require treatment. But as the condition worsens, you may experience:
- Thickened nails
- Discoloration, often yellow-brown or whitish coloring (a darker color could indicate that debris is building up under the nail bed)
- Change in nail texture, such as brittle or crumbling nails
- Change in the shape of your nailbed
- Odor ranging from mild to foul
If you notice any of these symptoms, you can try remedies such as:
- Over-the-counter products: Several antifungals are available without a prescription. File your nails then soak them in warm water. Dry the nail thoroughly before applying the medicated creams or ointments.
- Nail grooming: Keeping your nails trimmed can reduce pain and pressure from debris and nail buildup.
If the condition worsens, reach out to your primary care doctor or a dermatologist. To diagnose nail fungus, your doctor likely will take a sample of debris, nail or surrounding skin and send it to a laboratory.
Nail fungus treatments
There are several treatment options available for nail fungal infections, so it’s important your doctor correctly identifies the fungus that is creating the problem. Effectively treating fungal infections can take time, and repeat infections are common. Though nail fungal infections are difficult to resolve, it is possible. However, your nail may never look as healthy as it did before the infection.
There are two primary methods for treating nail fungus:
Medications
Your doctor may prescribe one or a combination of the following antifungal medications:
- Oral medications: Taking an antifungal medication by mouth dramatically increases the likelihood that the newly growing nail is free of infection. Over time, the infected nail is replaced as a healthy nail grows in. This treatment can take up to three months, depending on how fast the nail grows. Depending on your health and the medication your provider selects, you may need follow-up testing to prevent organ damage.
- Medicated nail polish or creams: Medicated nail creams and polishes can be used to treat the infection. Some medications are applied daily, others weekly. As with non-prescription-strength antifungal creams, these work best when you soak, dry and keep your nails trimmed. You may need to continue the process for a year or more.
Nail removal
Nail removal is typically a last resort if treatments aren’t effective for severe infections. Your doctor likely will refer you to a dermatologist or another specialist for this treatment. The specialist can use a chemical to dissolve the nail or remove the nail surgically in the clinic. The nail will not grow back.
Prevent new or repeat nail infections
Reduce your risk of infection by avoiding situations where fungi can spread. Also, consider these tips:
- Wear foot covers in locker rooms, public showers and on pool decks. These warm, moist areas are breeding grounds for fungi.
- Discard any footwear you used before you were infected since fungus can live in shoes and re-infect you after your treatment is over. You can also use an ultraviolet shoe sanitizer to disinfect footwear.
- Change socks daily or when feet get sweaty to prevent fungi from growing.
- Wear quality, well-fitting shoes. Shoes that are too tight or those with a non-breathable material can create the right environment for fungi to grow.
- Prevent fungus from growing in shoes by allowing damp shoes to completely dry out before you wear them or by putting antifungal powder in your shoes.
- Practice nail hygiene. Make it harder for fungi to get under the nail by keeping your feet clean and dry and your nails trimmed. Make sure nail scissors and clippers are sanitized and not shared.
- Treat athlete’s foot immediately since it can spread to your nailbed.
- Moisturize your hands and feet since fungus can enter through small skin cracks that occur with dry skin.
If you have nail fungal symptoms or want more information about nail fungus prevention or treatment, contact your primary care physician.