Risk Stratification
Risk Stratification Before Elective Surgery
On this page:
Surgery Risk | Patient Medical Risk | Cardiac Risk | Pulmonary Risk | Renal Risk | Cognitive Dysfunction Risk | Risk of Difficult Pain Management
Risk factors that increase the likelihood of perioperative morbidity and mortality may include the patient’s underlying health problems as well as factors associated with each specific type of surgery. By combining risk scores for patient co-morbidity and the complexity of surgery, we can stratify overall risk and determine which patients should undergo more extensive preoperative evaluation.
If a patient who is scheduled for a non-emergency procedure is found to have medical conditions that are not under ideal control, this preoperative evaluation process can include optimization, or “prehabilitation”, so that the patient can be in the best possible health before surgery. This process may address blood pressure control, diabetes management, nutritional status, exercise tolerance, smoking cessation, and treatment of anemia, as examples.
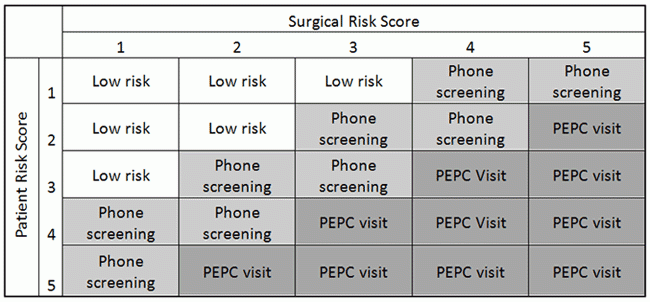
In the sections to follow, we outline a method of assigning a risk score to patient co-morbidity factors and surgical risk factors. We encourage referring physicians to send patients with risk scores of 7 or greater to our Preoperative Evaluation and Planning Center (PEPC) for an in-person visit and further evaluation. Patients with scores of 4 or less require no further screening, and will be interviewed by the physician anesthesiologist and the anesthesia team before surgery. Patients with intermediate risk scores may be referred for telephone screening by the PEPC staff.
Surgery Risk Stratification
The Surgical Risk Score assigns a numerical value to reflect the risk level associated with the procedure ranging from 1 (very low risk) to 5 (very high risk). These categories identify operations with increased potential for substantial blood loss or other intraoperative and postoperative risks.
| Surgical Risk Score | Surgery Types |
|---|---|
| 1- Very Low Risk | Procedures that usually require only minimal or moderate sedation and have few physiologic effects
|
| 2- Low Risk | Procedures associated with minimal physiologic effect
|
| 3- Intermediate Risk | Procedures associated with moderate changes in hemodynamics, risk of blood loss
|
| 4- High Risk | Procedures with possible significant effect on hemodynamics, blood loss
|
| 5- Very High Risk | Procedures with major impact on hemodynamics, fluid shifts, possible major blood loss
|
Patient Medical Risk Stratification
Pre-existing medical problems confer risk for perioperative complications, including cardiac decompensation, respiratory failure, acute kidney injury, and postoperative delirium or cognitive dysfunction.
| Patient Risk Score | Patient Characteristics |
|---|---|
| 1- Very Low Risk |
|
| 2- Low Risk |
|
| 3- Intermediate Risk |
|
| 4- High Risk |
|
| 5- Very High Risk |
|
Cardiac Risk Factors
Very high risk – score of 5:
- Unstable or severe angina
- Recent MI
- Decompensated CHF
- Severe valvular disease
Moderate risk – patients with two or more of the following conditions receive a score of 4, and three or more conditions a score of 5:
- History of ischemic heart disease
- Chronic, stable CHF
- History of stroke or TIA
- Insulin-dependent diabetes mellitus
- Renal disease with serum creatinine greater than 2 mg/dl
Pulmonary Risk Factors
Severe pulmonary disease – score of 5:
- COPD with FEV1 less than 50 percent of predicted
- Severe pulmonary hypertension
- Need for home oxygen therapy
Moderate pulmonary disease – score of 4:
- COPD with FEV1 between 50 and 70 percent of predicted
- Moderate pulmonary hypertension
- Obstructive sleep apnea
- Greater than 20 pack-year smoking history
Renal Risk
The most significant risk factor for postoperative renal failure is preexisting renal disease. Patients with GFR less than or equal to 60 ml/min or serum creatinine greater than 1.5 mg/dl are assigned a risk score of 3.
Cognitive Dysfunction Risk
High risk – score of 4:
- Current diagnosis of dementia or other cognitive disorder
- Bed-bound state
- Need for aid with activities of daily living
- Significant impairment of vision or hearing
Moderate risk – score of 3:
- Frailty
- Age greater than 70
- Unintentional weight loss
- Exhaustion
- Low physical activity
- Slowness
- Weakness
Risk of Difficult Pain Management
Postoperative pain control remains a key factor in length of stay, delay of intestinal motility after bowel resection, and patient satisfaction. Patients with chronic pain syndromes, high tolerance for opioids, or a history of substance abuse may be at high risk for difficult-to-manage postoperative pain.
We recommend that patients with any of the following risk factors be assigned a risk score of 5 and referred to PEPC phone screening for preoperative evaluation:
- Use of more than 6 doses per day of hydrocodone or hydromorphone
- Use of a long-acting or extended-release opioid such as Oxycontin
- Use of Suboxone
- History of complex regional pain syndrome (regional sympathetic dystrophy)
- History of substance abuse
- Intrathecal pump or spinal cord stimulator
References
- Tote, S. P., & Grounds, R. M. (2006). Performing perioperative optimization of the high-risk surgical patient. British journal of anaesthesia, 97(1), 4–11. doi:10.1093/bja/ael102
- Goodnough, L. T., Maniatis, a, Earnshaw, P., Benoni, G., Beris, P., Bisbe, E., … Szpalski, M. (2011). Detection, evaluation, and management of preoperative anaemia in the elective orthopaedic surgical patient: NATA guidelines. British journal of anaesthesia, 106(1), 13–22. doi:10.1093/bja/aeq361
- Fleisher, L. a, Beckman, J. a, Brown, K. a, Calkins, H., Chaikof, E., Fleischmann, K. E., … Yancy, C. W. (2007). ACC/AHA 2007 guidelines on perioperative cardiovascular evaluation and care for noncardiac surgery: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Writing Committee to Revise the 2002 Guidelines on Perioperative Cardiovascular Evaluation for Noncardiac Surgery): developed in collaboration with the American Society of Echocardiography, American Society of Nuclear Cardiology, Heart Rhythm Society, Society of Cardiovascular Anesthesiologists, Society for Cardiovascular Angiography and Interventions, Society for Vascular Medicine and Biology, and Society for Vascular Surgery. Circulation, 116(17), e418–99. doi:10.1161/CIRCULATIONAHA.107.185699
- Lee, T. H., Marcantonio, E. R., Mangione, C. M., Thomas, E. J., Polanczyk, C. a., Cook, E. F., … Goldman, L. (1999). Derivation and Prospective Validation of a Simple Index for Prediction of Cardiac Risk of Major Noncardiac Surgery. Circulation, 100(10), 1043–1049. doi:10.1161/01.CIR.100.10.1043
- Kalisvaart, K. J., Vreeswijk, R., de Jonghe, J. F. M., van der Ploeg, T., van Gool, W. a, & Eikelenboom, P. (2006). Risk factors and prediction of postoperative delirium in elderly hip-surgery patients: implementation and validation of a medical risk factor model. Journal of the American Geriatrics Society, 54(5), 817–22. doi:10.1111/j.1532-5415.2006.00704.x