Lap Band Removal
Find Your Care
Our bariatric surgeons use a range of treatments to help you reach weight loss goals and optimize your health. To learn more, call 310-206-0367.
What is the Lap Band?
The Lap Band, also known as the adjustable gastric band, involves an inflatable silicone band that is placed around the upper portion of the stomach to achieve weight loss. This creates a small stomach pouch above the band, leaving the rest of the stomach intact below it. Adjustments made to the band will increase or decrease the size of the passageway between the two parts of the stomach. The purpose is to slow down and limit how much food you can eat at any given time.
At UCLA, our surgeons do not perform Lap Band adjustments, but will evaluate for removal of the Lap Band. Patients who are interested in Lap Band removal as well as revision surgery to Gastric Bypass or Gastric Sleeve, may book a consultation to address all needs.

Kristen's Story - Weight Loss Surgery: Lap Band Revision*
Gastric Sleeve Revision from Lap Band
I have more energy than I've had my entire life!
View Kristen's Story
Disadvantages and Complications of Lap Band Surgery
Complications of Lap Band
Lap Band surgery is both minimally invasive and completely reversible. However, the majority of patients do not have good results from this procedure because of its many disadvantages and complications. Many studies have shown that more than half of the gastric bands are removed due to inadequate weight loss or complications after 7-10 years.
The common Lap Band complications include:
- Food Intolerance: Patients may develop difficulty swallowing, severe nausea and vomiting. Some even throw up multiple times a day.
- Heartburn or Reflux: Some patients may develop heartburn or esophagitis after Lap Band surgery.
- Band Slippage: This may cause severe pain/nausea and may require emergent surgical revision/removal of the gastric band.
- Band Erosion/Port Infection: This is a rare complication. Gastric Band erosion causes long-term port infection in most cases.
- Esophageal Dilation: With the restriction from the Gastric Band, the food may be stuck in the esophagus. In the long term, this may cause esophageal dilation.
- Inadequate Weight Loss: Even though the Gastric Band had reasonable initial weight loss, weight regain is much more common in Gastric Banding patients than patients who had gastric sleeve or gastric bypass surgery.
Because of these complications, we do not perform Lap Band surgeries at UCLA. If you are experiencing any of these problems due to your Lap Band, our surgeons specialize in both the removal and conversion of Lap Bands into other weight loss treatments. Learn more about bariatric surgery at UCLA >
National Trend of Lap Band Surgery
The Lap band once was the most popular bariatric procedure in United States in early 2010s. However, due to the inadequate weight loss, weight regain, and high long-term complication rate, the use of the Lap band has sharply decreased worldwide and in United States. Nowadays, the Lap band constitutes less than 10% of all bariatric procedures and the number of lap band procedures nationwide continues to go down every year. According to American Society of Metabolic and Surgery (ASMBS), about 35.4% of all bariatric procedures were Lap band in 2011. This number has decreased to 20.2% in 2012, 14% in 2013, 9.5% in 2014 and 5.7% in 2015.
Indications of Lap band removal:
- Inadequate Weight Loss or Weight Regain
- If a patient cannot lose enough weight (about 25-30% of excess their weight) or have significant weight regain, lap band removal and conversion to another more effective bariatric procedure may be indicated. This is the most common reason for lap band removal.
- Band Intolerance
- Symptoms of band intolerance can include excessive nausea and vomiting, difficulty swallowing and pain after eating.
- Band Infection
- Band or port infection indicates that the band may have eroded into the stomach. If the infection is not responsive to antibiotic treatment, further workup and likely band removal is recommended.
- Band Slippage
- Slippage can occur when the Lap band moves down the stomach and creates a bigger pouch above the band. This can be treated, sometimes with removing the fluid from the band or surgical reposition. However, band removal may be necessary in some cases.
- Severe Heartburn
- Some patients may develop new heartburn symptoms after lap band procedure. If the heartburn symptoms are severe, this may lead to esophagitis (inflammation of the esophagus). For patients with severe heartburn symptoms that do not respond to anti-acid medications, lap band removal may relieve the symptoms.
- Esophageal Dysmotility, Dilation or Esophagitis
- With long-term use of lap band, some patients may develop esophageal dilation (expansion of tissue), dysmotility (lack of movement) or esophagitis (inflammation). Fluid removal or lap band removal may be required for patients with severe symptoms.
Laparoscopic Lap Band Removal
Most lap band removal procures can be done laparoscopically. This is a relatively easy and safe operation depending on existing complications.
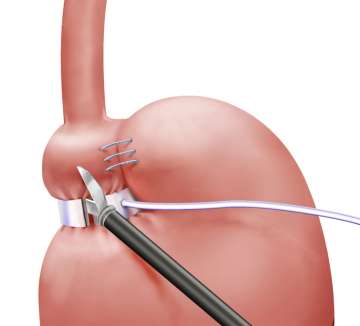
The steps of a lap band removal surgery are as follows:
- Insert laparoscopic instruments through small incisions. In most cases, the surgeon can use the old incision.
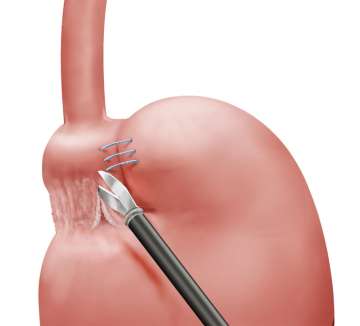
- Cut the scar tissue around the band.
- Cut the tubing and band.
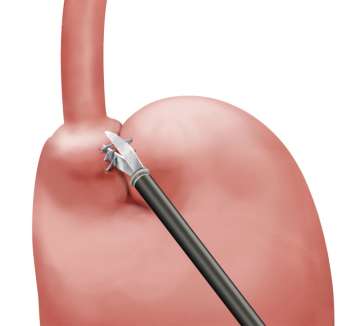
- Pull out the band from around the stomach.
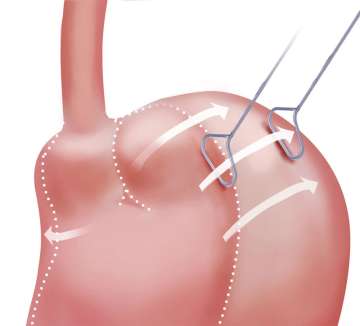
- During the initial operation, the upper part of the stomach (fundus) is usually sutured to the part of the stomach above the band to prevent band migration. Some general surgeons tend to leave the adhesions and those sutures in place during the Lap Band removal surgery. However, it is very important to remove those sutures and lyse the adhesions. This will restore the original anatomy of the stomach and make subsequent or later revision surgery much easier.
- After removing the gastric band, removal or incision of the perigastric capsule (dense scar tissue around the upper part of the stomach or esophagus) will reduce the chance of obstruction after surgery.
- The subcutaneous port is removed
- For patients who want to convert to a more effective bariatric procedure, the surgeon may proceed with the sleeve gastrectomy or gastric bypass surgery following the removal of gastric band or perform a revision three months later.
Lap Band Conversion to Sleeve Gastrectomy and Gastric Bypass
If you have an intolerance and/or complication to the gastric band, such as nausea, vomiting, dysphagia, slippage, or erosion, removal of your band offers immediate symptom relief. However, without converting to another bariatric procedure, many patients regain weight after Lap Band removal. At UCLA, we offer minimally invasive gastric bypass or sleeve gastrectomy surgery, 3 months after Lap Band removal surgery.
The advantages of conversion to Gastric Sleeve (or Gastric Bypass) include:
- Better Quality of Life: It is very rare to have nausea or vomiting after gastric sleeve surgery. Patients also feel less hungry after gastric sleeve surgery and many patients lose their hunger sensation.
- Significant Weight Loss Difference: In the long term, patients have much greater weight loss with gastric sleeve than with Lap band.
- Low Complication Rate: The long-term complication rate of the gastric sleeve is extremely low, while more than half of Lap Band Surgery patients need to have their gastric band removed at some time point.
Contact Us
To schedule a consultation with UCLA Bariatric Surgery in Los Angeles, California, call us at 310.206.0367 or fill out our online form.
*Weight loss results can vary depending on the individual. There is no guarantee of specific results. Read full disclaimer.