Medullary Thyroid Cancer
Find Your Care
We deliver effective, minimally invasive treatments in a caring environment. Call 310-267-7838 to connect with an expert in endocrine surgery.
What is Medullary Thyroid Cancer?
Medullary thyroid cancer (aka medullary thyroid carcinoma, MTC) is an uncommon type of thyroid cancer. The two more common types of thyroid cancer, papillary and follicular cancer, develop from the thyroid cells that make thyroid hormone. Medullary thyroid cancer develops from “parafollicular C” cells that produce and release calcitonin, a hormone that regulates calcium.
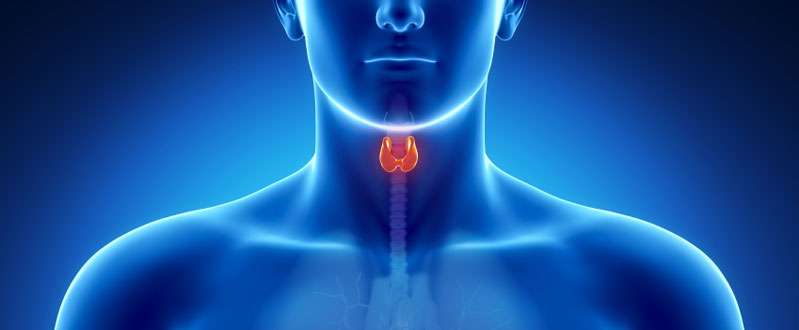
What are the Signs and Symptoms of Medullary Thyroid Cancer?
Most patients with medullary thyroid cancer experience no symptoms. Some patients may notice a new lump in the neck or throat. Rarely, patients may feel a lump in throat with swallowing, new hoarseness of voice, or new cough.
How is Medullary Thyroid Cancer Diagnosed?
Once a neck mass is suspected or found, the first step is to perform a high-quality neck ultrasound. Whenever possible, we perform our own neck ultrasound during the office visit. We use the ultrasound images to decide which patients would benefit from a thyroid biopsy. Sometimes, we decide no biopsy is necessary and choose to observe a thyroid nodule instead.
If a thyroid biopsy is recommended, a fine needle aspiration biopsy (FNA for short) is performed. For more information on FNA please see our video here or our webpage on FNA.

What is the Initial Management of a New Diagnosis of Medullary Thyroid Cancer
If the FNA confirms the diagnosis of medullary thyroid cancer, the following tests are needed:
- Calcitonin
- Carcinoembryonic Antigen (CEA)
- Genetic counseling
- Calcium
- [Select Cases] Metanephrines and normetanephrines (blood and/or urine)
The cells that make up medullary thyroid cancer usually produce calcitonin and/or CEA. Thus, calcitonin and CEA are tumor markers for medullary thyroid cancer. We use these tests to estimate the extent of disease, and guide how aggressive surgical management should be.
Up to 25% (1 in 4) cases of medullary thyroid cancer are familial, meaning it can be passed down by family members. Thus, it’s important to receive genetic counseling and consider genetic testing. In some cases, medullary thyroid cancer is passed down as part of a genetic syndrome. The other 75% (3 in 4) cases are sporadic, which are not inherited or passed down. The genetic test is a blood test that looks for a mutation in the RET gene.

How is Medullary Thyroid Cancer Treated?
Medullary thyroid cancer is primarily treated through surgery. The extent of surgery depends on the size of tumor, assessment of lymph nodes on the neck ultrasound, and results of blood tests above. In most patients, removal of the entire thyroid gland and surrounding lymph nodes is recommended. For a minority of patients, we may also recommend removal of the lymph nodes from the side of the neck the tumor is in.
When the tumor has been removed completely, no further treatments are needed. We monitor patients with calcitonin and CEA levels, as well as neck ultrasound.
Advanced cases are discussed at our multidisciplinary tumor board. In rare circumstances, patients may also need radiation therapy or targeted therapy.
Is Medullary Thyroid Cancer Curable?
Yes, medullary thyroid cancer is curable, especially when detected early. Following complete removal of medullary thyroid cancer, only 4% of patients will have a regrowth of the medullary thyroid cancer at 5-7 years after surgery.
Even in patients who are unlikely to be completely cured of disease, the disease is manageable and we have many treatment options at UCLA.
What is the Prognosis for Someone with Medullary Thyroid Cancer?
Prognosis varies across patients and depends on many factors. One major factor is how a patient responds after initial treatment with surgery.
When there is no trace of calcitonin or CEA in the bloodstream after an operation, 10-year survival is 95%. In that time frame, only 4% of patients will have a visible cancer regrowth.
When there is some detectable calcitonin or CEA after surgery, but all visible tumor has been removed, the 10-year survival is still 94.7%. However, about 37% of these patients will have visible cancer regrowth that requires additional surgery or treatment in the future.
When there is persistent disease that could not be removed surgically, the 10-year survival is 40%.
Read more on cancer.org and at liebertpub.com.
What is the Difference Between Papillary Thyroid Cancer and Medullary Thyroid Cancer?
Since medullary thyroid cancer originates from a different type of cell, it does not behave like the more common papillary thyroid cancer. Thus, there are three major differences in how medullary thyroid cancer is managed.
- Medullary thyroid cancer cells do not take up iodine, so radioactive iodine treatment is not effective against medullary thyroid cancer
- Medullary thyroid cancer cells do not produce thyroglobulin, but instead make calcitonin and carcinoembryonic antigen
- Sometimes we will remove normal appearing lymph nodes depending on the level of calcitonin and/or CEA before surgery
Is Medullary Thyroid Cancer Inherited?
Twenty five percent of medullary thyroid cancer diagnoses are inherited. Patients with an inherited form of medullary thyroid cancer usually have a mutation in the RET gene. This mutation causes the development of medullary thyroid cancer. A blood test for a mutation in the RET proto-oncogene can lead to an early diagnosis of MTC and surgery to remove it.
Two genetic syndromes are associated with medullary thyroid cancer are MEN-2A and MEN-2B.
MEN-2A (also known as Sipple syndrome or PTC syndrome) is rare, affecting 1 in 35,000 people. Patients with MEN2A have a high chance (90%) of getting medullary thyroid cancer. These patients are also at risk (30% to 50%) of developing pheochromocytoma, a cancer of the adrenal glands.
MEN-2B (also known as Wagenmann-Froboese or MEN3) affects 1 in 1,000,000 people. Although uncommon, MEN2B can sometimes be passed from parent to child. Patients with MEN2B are at greater risk of developing medullary thyroid cancer at a very young age, with a 50% chance of developing pheochromocytoma at some point in their life.
For more information, please visit Genetic Syndromes.
What Should I Expect After Surgery?
Recovery after thyroid surgery.
In addition to the standard monitoring, patients should undergo regular neck ultrasound and blood tests to check calcitonin and carcinoembryonic antigen (CEA) levels.