2D vs. 3D Tomosynthesis
by Iris Chen, MD, and James Chalfant, MD
2D Mammography
Breast cancer is the most common cancer diagnosed in women and the most common cause of death from cancer among women in the world (1). Since breast cancer may grow slowly or evolve without clinical symptoms, many breast cancers are discovered during routine breast screening (1). Methods of breast cancer screening include breast palpation and breast imaging, including mammography, ultrasonography, and magnetic resonance imaging (MRI). The same imaging modalities can also be used for the diagnostic evaluation of clinical symptoms.
A mammogram is a radiograph that uses the differential attenuation characteristics of tissue to evaluate for breast cancer. Studies have concluded that routine screening with mammography in average-risk women can reduce mortality associated with breast cancer, with estimates of 28-36% in temporal (pre- and post-intervention) studies, 25-38% in incidence-based studies, and 31-48% in pooled estimates from case control studies (1). The American College of Radiology recommends annual screening with mammography for all women beginning at age 40 with an average risk of developing breast cancer and continuing for women with a life expectancy of at least five to seven years as long as the patient is willing to undergo further workup, biopsy, and treatment if indicated (1). In addition, mammography is usually indicated for clinically significant symptoms in patients 30 years or older.
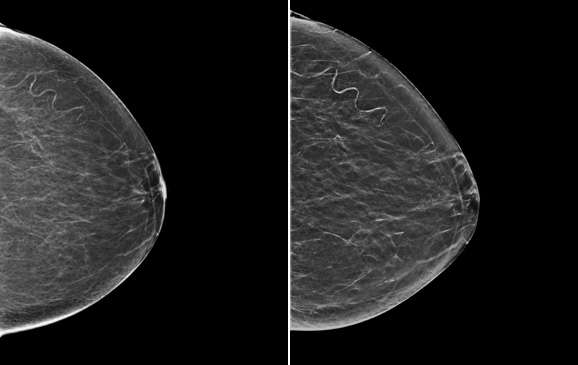
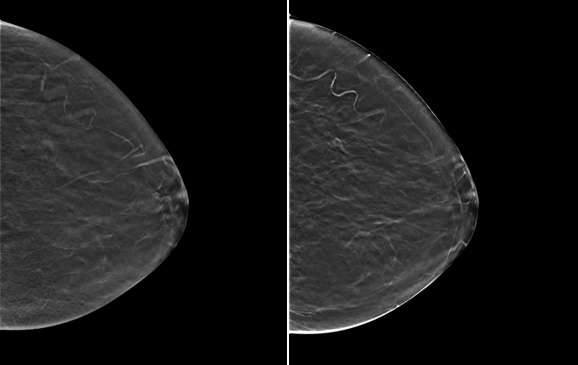
Traditionally, 2D mammograms have been performed, which offer a two-dimensional image of the breast. Screening mammograms are usually performed in two standard views, the craniocaudal (CC) and the mediolateral oblique (MLO) views. Additional diagnostic views including spot compression or variant angles may also be obtained. The differential attenuation characteristics of tissue allow for the identification of masses, calcifications, and other findings. For example, mammography can demonstrate suspicious microcalcifications that may otherwise not be palpable. Both screen film and, more recently, digital mammography formats have utilized 2D imaging.
Digital Breast Tomosynthesis
Digital breast tomosynthesis (DBT), colloquially known as 3D mammography, is a newer technology that was approved by the FDA in 2011. DBT acquires multiple mammographic projections serially along an arc and reconstructs this data via post-processing techniques into thin slice images to create a quasi-three-dimensional assessment of the breast. These reconstructed images result in partial blurring of features outside the selected plane. The multiple thin images allow radiologists to scroll through each image separately and attenuates the pitfall of superimposed breast tissue in a conventional 2D mammogram.
Multiple studies have shown that the combination of DBT and 2D mammography results in improved performance metrics when compared to 2D mammography alone. Some mammography units can also produce a synthetic 2D mammogram in post-processing of the DBT data, providing similar information to a conventional 2D mammogram without the additional image acquisition and associated radiation dose. A meta-analysis involving 42 studies and 2,606,296 patients evaluated breast cancer detection rate (CDR), invasive CDR, recall rate, and positive predictive value (PPV) in combined DBT and 2D mammography, combined DBT and synthetic 2D mammography, DBT alone, and 2D mammography alone. Combined DBT and 2D mammography and combined DBT and synthetic 2D mammography demonstrated a statistically significant higher CDR (6.36 per 1000 screened, P<0.001, and 7.40 per 1000 screened, P<0.001, respectively), higher invasive CDR (4.53 per 1000 screened, P=0.003, and 5.68 per 1000 screened, P<0.001, respectively), and higher PPV (10.0%, P=0.004, and 16.0%, P<0.001, respectively) compared to 2D mammography alone (CDR 4.68 per 1000 screened, invasive CDR 3.42 per 1000 screened, PPV 7.0%) (2). Combined DBT and synthetic 2D mammography demonstrated the lowest recall rate (42.3 per 1000 screened compared to 78.8 per 1000 screened for 2D mammography alone, P<0.001) (2). Because of these improved performance metrics, DBT is increasingly being incorporated into workflows as both a screening and diagnostic tool.
DBT usually requires increased interpretation time compared to a 2D mammogram (3). However, given the reduction in recall rates compared to 2D mammography, the utilization of DBT should reduce unnecessary further workup including additional imaging and biopsies and potential associated complications (2).
Radiation Dose
Both 2D mammography and DBT use low dose X-rays. In DBT, the X-ray tube rotates over a set angular range and a low dose radiograph of the breast is performed every few degrees. While DBT requires acquisition of more X-ray projections, each X-ray projection is achieved at a lower radiation dose than a single 2D mammographic projection. The resulting average absorbed dose to the glandular breast tissue is the summation of the absorbed doses in all the separate projections.
In a 2015 review examining the estimated radiation dose for DBT versus 2D mammography across multiple vendors, DBT ranged from a slightly lower radiation dose (DBT/2D mammography dose ratio 0.34-1.0) for 1-view DBT to slightly higher radiation dose (dose ratio 0.68-1.17) for 2-view DBT compared to 2D mammography alone (4). When DBT was combined with 2D mammography and compared to 2D mammography alone, radiation dose ratios ranged from 1.03-1.5 for 1-view DBT plus 2D mammography to 2.0-2.23 for 2-view DBT plus 2D mammography. However, this higher radiation dose can be reduced by approximately 45% when synthetic 2D mammography is used instead of 2D mammography, resulting in only a 19% higher dose compared to 2D mammography alone (with some vendors attaining even lower doses) (4). It is important to remember that radiation dose estimations are based off a breast phantom model, which approximates a breast in compression measuring 45 mm and composed of 50% glandular and 50% adipose tissue (4). In practice, dose can still vary greatly depending on breast density, thickness, and acquisition technique.
References:
- Narayan AK, Lee CI, Lehman CD. Screening for Breast Cancer. Med Clin North Am 2020;104(6):1007-1021. doi: 10.1016/j.mcna.2020.08.003
- Alabousi M, Wadera A, Kashif Al-Ghita M, Kashef Al-Ghetaa R, Salameh JP, Pozdnyakov A, Zha N, Samoilov L, Dehmoobad Sharifabadi A, Sadeghirad B, Freitas V, McInnes MD, Alabousi A. Performance of Digital Breast Tomosynthesis, Synthetic Mammography, and Digital Mammography in Breast Cancer Screening: A Systematic Review and Meta-Analysis. J Natl Cancer Inst 2021;113(6):680-690. doi: 10.1093/jnci/djaa205
- Caumo F, Zorzi M, Brunelli S, Romanucci G, Rella R, Cugola L, Bricolo P, Fedato C, Montemezzi S, Houssami N. Digital Breast Tomosynthesis with Synthesized Two-Dimensional Images versus Full-Field Digital Mammography for Population Screening: Outcomes from the Verona Screening Program. Radiology 2018;287(1):37-46. doi: 10.1148/radiol.2017170745
- Svahn TM, Houssami N, Sechopoulos I, Mattsson S. Review of radiation dose estimates in digital breast tomosynthesis relative to those in two-view full-field digital mammography. Breast 2015;24(2):93-99. doi: 10.1016/j.breast.2014.12.002