Swallowing Disorders Program
UCLA's Swallowing Disorders Clinic provides expert personnel and state-of-the-art equipment for the diagnosis and treatment of swallowing disorders.
Swallowing problems (dysphagia) can occur at any point in the process of moving food, liquid, or saliva from the mouth through the throat (pharynx), into the esophagus and to the stomach. These problems may result in poor nutrition, dehydration or aspiration (accidental ingestion of food particles or fluids into the lungs).
Dysphagia reduces quality of life. Swallowing disorders are often accompanied by voice impairment (dysphonia) as well. The central goal of the Clinic is to provide comprehensive evaluation and management of dysphagia and related disorders and improve quality of life.
The program's guiding principles include fostering an environment for research, education, and training of future clinicians in the field of dysphagia and dysphonia.
Conditions Treated
- Dysphagia
- Swallowing problems after brain surgery
- Swallowing problems after head and neck surgery
- Swallowing problems after cervical spine surgery
- Swallowing problems after thoracic surgery
- Swallowing problems after stroke
- Swallowing problems from neurologic disease
- Swallowing problems from head and neck cancer
- Swallowing problems after chemoradiation therapy
- Chronic aspiration
- Esophageal stenosis
- Cricopharyngeal spasm (achalasia)
- Zenker's diverticulum
Symptoms of Abnormal Swallowing (Dysphagia)
Indications of a swallowing disorder may include:
- Inability to swallow or extensive time required to swallow
- Frequent choking on food
- Hesitancy in swallowing food
- Coughing during or immediately after eating or drinking
- Pain during swallowing
- Recurring pneumonia
- Unexplained weight loss
- Regurgitation
- Heartburn
Causes of Abnormal Swallowing (Dysphagia)
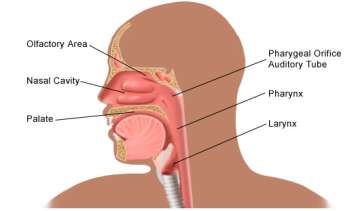
Patients may suffer from swallowing or voice difficulties for a number of reasons, including:
- Stroke or other forms of acute neurological damage
- Head and neck cancers
- Radiation therapy to the neck
- Heart surgery or other chest surgery, which may lead to vocal cord weakening or paralysis
- Trauma to the throat or larynx
- Tracheostomy tubes
- Degenerative neurological disorders such as dementia (including Alzheimer's disease), multiple sclerosis, Parkinson's disease, or Lou Gehrig's disease (amyotrophic lateral sclerosis)
- Pharyngeal and esophageal sacs and pouches (diverticulum) and narrowing (stenosis)
- Age-related changes
Diagnosis and Treatment
The Swallowing Disorders Program offers expert personnel devoted and an array of sophisticated diagnostic tools and treatment modalities.
Many diagnostic procedures that previously required sedation in an operating room can now be administered in the Clinic suite using topical anesthesia.
Procedures performed include:
- Fiberoptic endoscopic evaluation of swallowing: a fiberoptic flexible endoscope is inserted through the nose while the physician observes the patient's swallowing anatomy and function as food of various consistencies is swallowed. Swallow can be assessed without using x-rays.
- In-office transnasal esophagoscopy: this new procedure allows physicians to examine the entire swallowing apparatus -- from mouth to esophagus -- without sedating the patient. The procedure is quicker and safer than traditional esophagoscopy under sedation or general anesthesia. Biopsies can be taken as needed. Watch video on transnasal esophagoscopy
- Distal chip endoscopy: A video camera placed on the tip of the endoscope provides physicians with higher resolution, close-up images of the swallowing process and anatomy compared to traditional fiberoptic endoscopes.
- Vocal cord injection: Vocal fold paralysis leads to inadequate closure of the larynx during swallowing that causes choking during swallowing. UCLA physicians pioneered simple in-office vocal fold injection technique to improve laryngeal closure during swallowing so voice and swallowing capabilities can be immediately restored.
- In-office laryngoscopy with biopsy: Examination and biopsy of the pharynx, larynx, and esophagus can be performed in the clinic under topical anesthesia, rather than in an operating room under sedation.
- Behavioral swallowing therapy: Biofeedback and surface electromyography are offered to appropriate candidates. The clinic has extensive experience with swallowing therapy.
- Esophageal dilation: In cases of esophageal stenosis, the esophagus can be dilated in the clinic.
Operating room procedures:
- Management of upper esophageal sphincter dysfunction, including endoscopic dilations, cricopharyngeal myotomy, and Zenker's Diverticulectomy.
- Procedures for laryngeal weakness and paralysis including thyroplasty, arytenoid adduction, laryngeal reinnervation
- Surgery for esophageal stenosis
- Surgery for intractable aspiration such as tracheostomy, laryngeal diversion procedures, hypopharyngoplasty, laryngeal elevation surgery
Unique approach to Swallowing Disorders
The Clinic's unique approach involves evaluation of patients with swallowing problems by both an otolaryngologist and a speech pathologist as needed in the same premises. Usually, these specialists work in separate clinics, requiring the patient to seek care in multiple locations. A comprehensive surgical, medical, or rehabilitation management plan, tailored to the individual patient, is then developed without delay. Quick targeted referrals are set up with neurologists, gastroenterologists, and thoracic surgeons especially interested in the care of patients with dysphagia. Each patient receives a personalized treatment and monitoring regimen based on his or her medical and personal needs.
Our Expert Team
Program Physician:
Dinesh K. Chhetri, MD, is the Director of the Swallowing Disorders Program and is a nationally recognized expert on voice, airway, and swallowing disorders.
Program Speech Pathologist
Andrew Erman, M.A., C.C.C.-S.L.P.
Manager, Speech Pathology Clinic
Contact Information
Information, Referral, and Appointments: (310) 794-4225