Nelson's Syndrome
Find your care
We treat pituitary tumors using the latest innovations in minimally invasive procedures. To connect with an expert in the pituitary tumor program, call 310-825-5111.
Nelson's syndrome is a rare disorder that occurs in some patients with Cushing's disease patients as a result of removing both adrenal glands. In Nelson's syndrome, the pituitary tumor continues to grow and release the hormone ACTH.
This invasive tumor enlarges, often causing visual loss, pituitary failure and headaches. One key characteristic of Nelson's disease is dark skin pigmentation, resulting from the skin pigment cells responding to the release of ACTH.
Nelson's Syndrome: Expert Care in Southern California
The UCLA Pituitary Tumor Program offers comprehensive management of Nelson's syndrome. Our physicians have years of experience in diagnosing, treating and managing pituitary conditions and treat a high volume of patients. Our sophisticated diagnostic equipment, team approach and minimally invasive surgical procedures make our program one of the best in the United States.
Use these links to explore more about Nelson's syndrome:
Nelson's Syndrome: Physiology
Nelson's syndrome can develop as a result of a specific treatment (bilateral adrenalecomy) for the pituitary disease called Cushing's disease. The harmful effects of Cushing's disease are due to the excessive amount of the hormone cortisol produced by the adrenal glands.
To treat Cushing's disease, your doctor may recommend removing the adrenal glands, during a procedure called a bilateral adrenalectomy. The procedure will stop cortisol production and provide relief. However, the procedure does not treat the actual tumor. Rapid growth of the pituitary tumor can occur.
In about 15-25 percent of patients who had a bilateral adrenalectomy, Nelson' syndrome develops within one to four years.
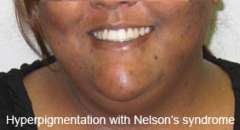
Nelson's Syndrome: Symptoms
The most obvious symptom of Nelson's syndrome is the darkening of the skin color (hyperpigmentation).
Macroadenomas
Macroadenomas are large pituitary tumors. Large tumors can compress surrounding structures, primarily the normal pituitary gland and optic (visual) pathways, causing symptoms. The symptoms that result from the compression are independent of the effects of excess growth hormone secretion.
This may result in vision problems:
- Vision loss. This occurs when macroadenomas grow upward into the brain cavity, compressing the optic chiasm.
- A loss of the outer peripheral vision, called a bitemporal hemianopsia
-

When severe, a patient can only see what is directly in front of them.
- Many patients do not become aware of their visual loss until it is quite severe.
-
- Other visual problems can include:
- Loss of visual acuity (blurry vision), especially if the macroadenoma grows forward and compresses an optic nerve.
- Colors not perceived as bright as usual
Pituitary Failure or Hypopituitarism
Increased compression of the normal gland can cause hormone insufficiency, called hypopituitarism. The symptoms depend upon which hormone is involved.
Nelson's Syndrome: Diagnosis
Most patients with Nelson's syndrome have undergone a bilateral adrenalectomy for the treatment of Cushing's disease
Diagnostic testing includes:
- Hormone testing. Typically, the blood ACTH levels are very elevated. Learn more about hormone testing at the UCLA Pituitary Tumor Program.
- MRI imaging. Magnetic resonance imaging (MRI) scan of the pituitary gland can detect the presence of an adenoma, a pituitary tumor.
Nelson's Syndrome: Treatment Options
Treating Nelson's syndrome effectively requires an experienced team of experts. Specialists at the UCLA's Pituitary Tumor Program have years of experience managing the complex coordination and care for treatment of Nelsons' syndrome.
Treatment options include:
Surgery for Nelson's Syndrome
Surgical removal of the pituitary adenoma is the ideal treatment; however, it is not always possible. Surgical removal requires advanced surgical approaches, including delicate procedures involving the cavernous sinus.
If surgery is required, typically the best procedure is through a nasal approach. Our neurosurgeons who specialize in pituitary tumor surgery are experts in the minimally invasive expanded endoscopic endonasal technique. This procedure removes the tumor while minimizing complications, hospital time and discomfort. This advanced technique requires specialized training and equipment.
Very large tumors that extend into the brain cavity may require opening the skull (craniotomy) to access the tumor. Our surgeons are also experts in the minimally invasive "key-hole" craniotomy, utilizing a small incision hidden in the eyebrow.
Radiation Therapy for Nelson's Syndrome
Radiation therapy can be effective in controlling the growth of the tumor. However, if you received radiation therapy in the past, additional radiation may not be safe.
Our Pituitary Tumor Program offers the latest in radiation therapy, including stereotactic radiosurgery. This approach delivers a highly focused dose of radiation to the tumor while leaving the surrounding brain structures unharmed (with the exception of the normal pituitary gland).
One consequence of radiation treatment is that it can cause delayed pituitary failure. This typically occurs several years after treatment, and continued long-term follow-up with an endocrinologist is important. You may require hormone replacement therapy.
Medical Therapy for Nelson's Syndrome

Medical therapies for the treatment of Nelson's syndrome are currently limited, but include:
- Somatostatin-analogs (SSAs). These medications are typically used to treat acromegaly. A small number of Nelson's syndrome patients may respond.
- Cabergoline. This medication is typically used to treat prolactinomas; you may require a very high dose.
- Temozolomide. This is a type of chemotherapy used to treat primary brain tumors called glioblastoma.
If you require medication to treat Nelson's syndrome, our endocrinologists will monitor you closely.
Contact Us
To schedule an appointment with one of our physicians at the Pituitary Tumor Program, please call (310) 825 5111.