TSHoma (Thyrotropinoma)
Find your care
We treat pituitary tumors using the latest innovations in minimally invasive procedures. To connect with an expert in the pituitary tumor program, call 310-825-5111.
A pituitary tumor that secretes a hormone called thyroid-stimulating hormone (TSH) is called a thyrotropinoma (or sometimes a TSHoma). An excess of amount of thyroid hormone causes hyperthyroidism, which can be a serious medical condition.
TSHoma: Expert Care in Southern California
The UCLA Pituitary Tumor Program offers comprehensive management of TSHoma. Our physicians have years of experience in diagnosing, treating and managing pituitary conditions. Because thyrotropinomas are so rare, representing just one percent to two percent of all pituitary adenomas, patients are often misdiagnosed for years. Many patients end up undergoing treatments to destroy the thyroid.
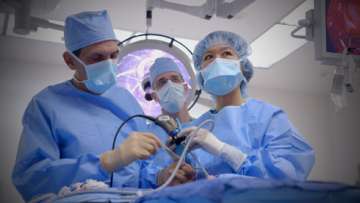
That is why it is so important to come to a recognized pituitary tumor center for proper, accurate diagnosis and treatment.
Use these links to explore more about TSHoma:
TSHoma: Symptoms
Often, patients experience the typical symptoms of hyperthyroidism. Sometimes, patients will experience mild symptoms or even none at all.
Symptoms of hyperthyroidism include:
- Nervousness
- Irritability
- Increased perspiration
- Heart racing
- Hand tremors
- Anxiety
- Difficulty sleeping
- Thinning of the skin
- Fine, brittle hair
- Muscular weakness
- More frequent bowel movements
- Weight loss
- In women, lighter and less frequent menstrual flow
TSHoma Symptoms: Thyroid Storm
Thyroid storm is a rare but severe complication of hyperthyroidism, requiring prompt treatment and hospitalization. Thyroid storm may occur when a thyrotoxic patient becomes very sick or physically stressed.
- Symptoms can include:
- Increase in body temperature to over 40 degrees Celsius (104 degrees Fahrenheit)
- Tachycardia
- Arrhythmia
- Vomiting, diarrhea
- Dehydration
In addition to hyperthyroidism, you may experience symptoms including:
- Diffuse goiter
- Menstrual disturbances
- Breast milk production (galactorrhea)
TSHoma: Macroadenomas
Rarely, patients with thyrotropinomas experience tumor mass effect, caused by large pituitary tumors (macroadenomas). In addition to the severe hormonal effects related to hyperthyroidism, the large tumor can compress adjacent structures leading to:
-

Vision loss. This occurs when macroadenomas grow upward into the brain cavity, compressing the optic chiasm.
- A loss of the outer peripheral vision, called a bitemporal hemianopsia
- When severe, a patient can only see what is directly in front of them.
- Many patients do not become aware of their visual loss until it is quite severe.
- Other visual problems can include:
- Loss of visual acuity (blurry vision), especially if the macroadenoma grows forward and compresses an optic nerve.
- Colors not perceived as bright as usual
Pituitary Failure or Hypopituitarism
Increased compression of the normal gland can cause hormone insufficiency, called hypopituitarism. The symptoms depend upon which hormone is involved.
- Reduction of sex hormones, luteinizing hormone (LH) and follicle-stimulating hormone (FSH).
- In men, this can lead to a low testosterone level, causing decreased sexual drive and impotence.
- In some cases, there can be loss of body and facial hair.
- In women, this can lead to infertility.
- Large pituitary tumors can slightly elevate blood prolactin levels. Doctors think this occurs because of compression of the pituitary stalk, the connection between the brain and pituitary gland. It is called the "stalk effect."
- In premenopausal women, this can lead to reduction or loss of menstrual periods and/or breast milk production (galactorrhea).
- Prolactin levels are only slightly elevated, as opposed to prolactinomas in which the prolactin level is usually very high.
More severe hypopituitarism can lead to hypothyroidism or abnormally low cortisol levels, which may be life threatening. Symptoms of severe hypopituitarism include;
- Loss of appetite
- Weight loss or weight gain
- Decreased mental function
- Dizziness
- Headache
TSHoma: Diagnosis
Your doctor will conduct a physical examination and ask you about your symptoms and medical history.
Diagnostic procedures include:
- Hormone testing
- Imaging scans
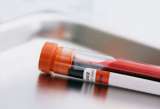
Hormone Testing for TSHoma
We use hormone tests to determine if there are elevated levels of thyroxine (T4) and thyrotropin (TSH). A neuro-endocrinologist, specializing in pituitary tumors, may be required in complex cases. Learn more about hormone testing at the UCLA Pituitary Tumor Program.
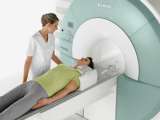
MRI Imaging
Your doctor may order a magnetic resonance imaging (MRI) of the pituitary gland to detect any tumors. We use a special MRI pituitary protocol in order to best visualize the tumor. Occasionally, a computed tomography (CT) scan may be used.
TSHoma: Treatment Options
Managing thyrotropinomas can be challenging. The most effective treatments involve the care and expertise of a multidisciplinary team, with close collaboration between the neurosurgeon and the endocrinologist. Surgery is usually needed, and the hyperthyroidism must be carefully managed prior to and during surgery to prevent serious complications.
Treatment options include:
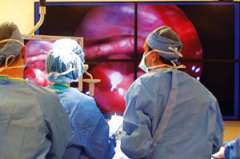
Surgery for TSHoma
Surgically removing the tumor, or tumors, offers the best chance for a cure. The neurosurgeons at UCLA's Pituitary Tumor Program perform a high volume of pituitary surgeries each year. Our surgeons practice the latest surgical techniques, such as the expanded, endoscopic endonasal approach allowing us to surgically remove tumors that were previously considered unresectable (unable to be removed surgically).
The success of the surgery depends on a number of factors, including the expertise and experience of the operating surgeon:
- If the tumor has invaded beyond the confines of the sella (the space where the normal pituitary gland sits), the chance for a cure is lower.
- The first surgery offers the greatest chance of cure; the cure rate with a second or third surgery is much lower.
Invasive and very large tumors may require additional therapy, including removal of the thyroid gland or stereotactic radiation of the pituitary tumor.

Medical Management of TSHoma
Anti-thyroid drugs are drugs that inhibit the production of thyroid hormones. These medications may take weeks to become effective. The dosage may also change over a period of months, until the optimal dosage is obtained. You will need to have regular doctor visits and blood tests to monitor the drug's effectiveness.
Examples of anti-thyroid medication include:
- Methimazole
- Propylthiouracil
- Beta blockers
- Beta blockers are typically used to treat high blood pressure but can help reduce rapid pulse associated with the sensation of palpitations, and decreasing tremor and anxiety.
- These drugs do not treat hyperthyroidism or any of its long-term effects.
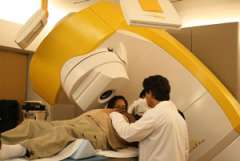
Radiation Therapy for TSHoma
Some tumors cannot be removed surgically, and may not respond to medications. Radiation therapy can be effective in controlling the growth of these tumors.
We use an advanced radiation therapy technique called stereotactic radiosurgery. This carefully sculpted radiation beam is able to deliver a high dose of radiation to the target. The surrounding brain structures receive only a fraction of the radiation and are typically unharmed, with the exception of the pituitary gland.
A consequence of radiation treatment is that it can cause delayed pituitary failure. This typically occurs several years after treatment. It is important that you continue your follow-up care with an endocrinologist, who can monitor your progress and any changes. You may require hormone replacement therapy.
Contact Us
To schedule an appointment with one of our physicians at the Pituitary Tumor Program, please call (310) 825 5111.