UCLA Endocrinology Westlake Village
Find Your Care
We deliver effective, minimally invasive treatments in a caring environment. Call 310-267-7838 to connect with an expert in endocrine surgery.
Bringing comprehensive endocrine services to Westlake Village
An Interview with Drs. Yaroslav Gofnung, Deepashree Gupta & Masha Livhits
What is unique about the approach that UCLA Westlake Village takes to the diagnosis and treatment of endocrine conditions?

At UCLA Westlake Village, we bring the level of care that you would get at an academic medical center to a community clinic setting. We have 2 board certified endocrinologists (Drs. Gofnung and Gupta) and a surgeon at this clinic. Dr. Livhits, our surgeon, sees patients in-office for consultation and postoperative appointments. Our physicians and surgeons are highly trained and incredibly involved in the academic community. We enjoy staying involved in each other’s fields - surgeons are very much involved in the latest updates in the field of endocrinology and vice versa. Through staying updated with the latest findings and advancements in research, we strive to always provide the best care for our patients.
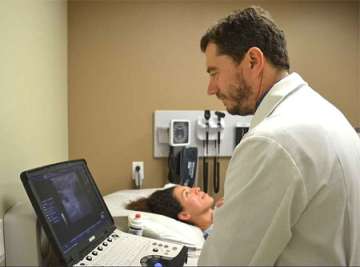
One of our top priorities is to make the process as easy as possible for patients. All of our services are centralized to cut down on travel time for patients and streamline the process (having all the records in the same place for example). Patients can get their bloodwork done at our onsite lab, which increases the turnaround time. Our onsite ultrasound facilities allow us to provide real time feedback to patients with thyroid and parathyroid conditions, rather than wait for the results a few days later from a radiologist.
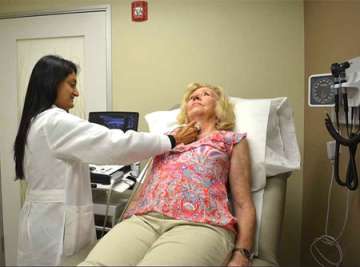
We have an onsite cytopathologist who examines biopsy samples as they are being collected and assesses adequacy on the spot. The benefits of having a microscope by the bedside can not be emphasized enough. We used to have to collect 5-6 samples, but now we typically only have to collect 2-3. This greatly reduces the chances that a biopsy will not be adequate (not have enough tissue to make a diagnosis) and has to be repreated. Drs. Gofnung, Gupta, and Livhits have extensive training and expertise in ultrasound and biopsy techniques. Dr. Gofnung has certification from the American Association of Clinical Endocrinologists (AACE) called ECNU (Endocrine Certification in Neck Ultrasounds), which is granted for attaining the highest standard in diagnostic ultrasonography of the neck and biopsy technique.
A major benefit of ultrasound is that it allows for a level of communication that is unparalleled by other forms of imaging. With bedside ultrasound, we discuss images with patients in real time. This gives patients an opportunity to ask questions and obtain answers right away. There are subtleties we can pick up on based on our thorough understanding of the patient’s background, details that may not stand out to an outside radiologist.
UCLA integrates the work of endocrinologists and surgeons. How has this medical-surgical overlap impacted your practice, as well as patient care? What unique services can UCLA provide to patients as a result?
UCLA is a one-stop shop. We are a multidisciplinary center that combines the expertise of surgeons, pathologists, and nuclear medicine specialists under one roof. If a patient comes to this office to see an endocrinologist, we can make an appointment to the endocrine surgeon in the same suite. Having this proximity allows us to improve patient care by increasing overall efficiency and allowing for collaboration on the spot. If a patient requires surgery, we coordinate care with the surgeon and discuss results together to formulate the best treatment plan.
We stay on the same page throughout the course of treatment, and this results in better patient outcomes. We have found that open communication between healthcare providers is essential, because it reduces the opportunity for confusion. One of the most detrimental things that happens in the physician-patient interaction is being told one thing from one physician, and being told the opposite from another. Understandably, this can be concerning. At our center, patients are getting the same message from every provider and can feel confidant that they are getting the right treatment.
How did you become interested in endocrinology / endocrine surgery?
Dr. Gofnung:
As an internal medicine resident, you get to rotate around different specialties, and one of my physician mentors was an endocrinologist. I really connected with how his approach was very cerebral to the patient. Endocrine is a thinking kind of field. Sometimes you get straightforward cases but sometimes not. It’s nice to be able to think through these puzzles and have that “aha” moment, and it’s satisfying to tie pieces together on a daily basis. There’s so many aspects of biology and pathophysiology that are interconnected, and we need to remain aware of this.
Another aspect that draws me to endocrinology is the human interaction. Prior to coming to UCLA, I noticed that patients with diabetes or other complicated chronic diseases were sometimes set aside. There’s a lot of care that is required for these patients, not just related to medicine. I enjoy being involved in the entire care of these patients.
Dr. Gupta:
My grandfather had uncontrolled type 2 diabetes and was dependent on dialysis. However, everything was preventable. I wanted to be in a field where I could help prevent so many devastating complications through the timely administration of care - both to the patient as a human being and to address their symptoms. Sometimes small modifications can prevent these life-threatening complications. I enjoy endocrinology because you get to take care of all aspects of a patient’s life. It is incredibly rewarding even though we’re dealing with chronic illness and frequently don’t have a quick turnaround. While you don’t get the same instant gratification as the ICU (Intensive Care Unit), it is wonderful being able to prolong a life without complications and to improve life quality.
Dr. Livhits:
As a surgeon, you can perform one operation that can meaningfully improve a patient’s life on a long-term basis. This immediate result is what drew me to the field of surgery. Many if not most endocrine surgery patients can be cured after a single operation. This includes hyperparathyroidism, early stage thyroid cancer, and most adrenal disorders. I have the satisfaction of developing a long-term relationship with my patients and see them doing well for many years after surgery. In addition, endocrine surgery includes a lot of medical endocrinology and I like being involved in the work-up, diagnosis, treatment decisions, and postoperative surveillance.
How has treatment of thyroid cancer changed over the years? Where do you see the field advancing in the future?
With the 2015 thyroid nodule and thyroid cancer guidelines, the trend has been towards “less aggressive treatment.” We have become more conservative with respect to whether or not to perform biopsies, the extent of surgery (removing half the thyroid, the whole thyroid, and the lymph nodes), and the use of radioactive iodine ablation after surgery.
Two things have helped us in providing just the right amount of treatment:
- Increased training of endocrinologists and endocrine surgeons. We have incorporated the use of Ultrasound into our standard of care, which allows us to make more accurate diagnoses. For example, if we see a low suspicion thyroid nodule, we can offer a more conservative approach rather than a blanket treatment such as a total thyroidectomy. The extent of treatment is tailored to each patient’s presentation, and we have found that individualizing care has not only maintained good outcomes but has also allowed patients to participate in their health care choices to make the best decisions.
- Advances in molecular marker testing, which is our second layer of genetic testing for nodules with an uncertain biopsy result. Based on the results of this test, we can observe nodules with a low risk for cancer and plan surgery for nodules with a high risk of cancer.
What advantages does ultrasound bring for thyroid nodules?
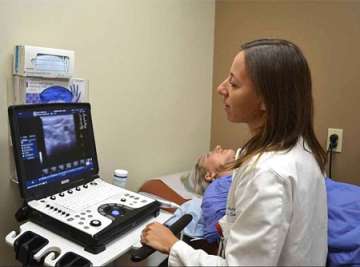
Ultrasound plays an essential role in guiding treatment for thyroid nodules and cancers. It allows us to analyze nodule characteristics, visualize the needle during biopsy, and assess for any spread of thyroid cancer in the neck.
The use of ultrasound reduces biopsy-related complications such as bleeding. By visualizing where the needle is at all times, we can also reduce the number of pricks required to obtain enough tissue for analysis.
One misconception patients and even other physicians have is that thyroid nodules are homogenous (the entire nodule is the same). Sometimes, only one part of a growth is malignant. This is why ultrasound is so useful during a biopsy. Ultrasound allows us to visualize where the abnormal portion of the nodule is, so that we can biopsy it and avoiding missing the cancer.
UCLA endocrine surgeons are uniquely trained in Ultrasound and always perform their own ultrasound prior to surgery. We have a dedicated ultrasound in our Westlake Village location that we use for all thyroid and parathyroid patients. Dr. Livhits will peform a preoperative ultrasound to assess for spread of cancer and discuss whether lymph node dissection will be required.
For prospective patients who are worried about their upcoming thyroid biopsy, what would you advise them?
Pain and discomfort are the biggest concerns we get, but most patients come out saying it was a lot better than they expected. The actual biopsy only lasts 5-10 seconds, with the bulk of the time spent on preparation and cleanup.
We understand that patients are placed in a vulnerable position during the biopsy, so we do everything we possibly can to minimize discomfort. We use local anesthetic to numb up the skin prior to biopsy. We use the thinnest needle possible (thinner than the needle used to draw blood).
What advantages do patients with hyperparathyroidism (overactive parathyroid gland) get by coming to the UCLA Westlake Village center?
Due to the availibility of laboratory testing and ultrasound on-site, we can make the diagnosis and often find the abnormal parathyroid gland on ultrasound. This allows us to expedite the treatment of hyperparathyroidism. We have 4D Parathyroid CT available when necessary to help us identify the abnormal parathyroid gland prior to surgery. All of our CT scans are read by our dedicated head and neck radiologists at UCLA.
Dr. Livhits routinely evaluates all four parathyroid glands during surgery and uses intraoperative parathyroid hormone monitoring (checking the parathyroid hormone level after the abnormal parathyroid gland has been removed) to achieve the best possible long-term cure rate.
Information for physicians: Our clinic has an open referral system. If a patient needs a thyroid biopsy, they do not require an official consult with us prior to the biopsy procedure. This helps increase access and speed to necessary services.