Outcomes in endocrine surgery
Find Your Care
We deliver effective, minimally invasive treatments in a caring environment. Call 310-267-7838 to connect with an expert in endocrine surgery.
Parathyroid, Thyroid, Adrenal Surgery Outcomes - UCLA in Los Angeles, CA
Outcomes in endocrine surgery | Outcome studies specific to endocrine surgery | UCLA study on endocrine surgery outcomes | Surgeon experience, length of hospitalization, and the cost of endocrine surgical care | Outcomes in parathyroid surgery | Outcomes in adrenal surgery | Potential shortcomings of the UCLA study on endocrine surgery outcomes | What are the implications of the UCLA study and others? | References
Outcomes in endocrine surgery
What are surgical outcomes?
The growing field of surgical outcomes research examines the end results of surgical care, with the ultimate aim of improving the level of service provided to patients who undergo surgery for various diseases. Here are some examples of questions posed by surgical outcomes studies:
- Does a new type of cancer operation lead to prolonged survival?
- Does a new type of cancer operation reduce the risk of disease recurrence?
- What is the frequency of complications following surgery of the pancreas?
- Does surgeon experience influence the frequency of complications?
For additional background information, please see our page on health care quality and safety >
Outcome studies specific to endocrine surgery
We have already discussed the positive relationship between surgical volume (the number of operations performed at a given hospital or by a given surgeon) and outcomes. A small number of studies have examined the volume-outcomes relationship in endocrine surgery, and we will review those here.
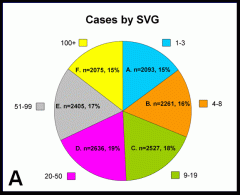
Figure 1.
- Distribution of cases (endocrine operations, Panel A),
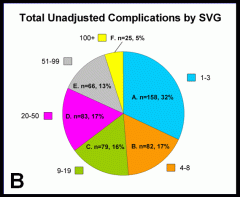
- complications (Panel B),
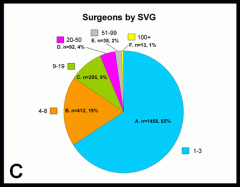
- and surgeons (Panel C) according to surgeon volume group (SVG).
- The number of cases performed by each surgeon volume group is indicated by the colored squares.
- Though cases were evenly distributed between groups, complications and surgeons were significantly skewed (see main text).
In 1998, Sosa and associates studied more than 5000 thyroid operations performed in the state of Maryland (1) . They found that surgeons performing more then 100 thyroid operations per year had significantly lower overall complication rates, including lower rates of recurrent laryngeal nerve injury and wound complications, when compared to lower volume surgeons.
Recurrent laryngeal nerve injury leading to hoarseness is almost certainly the most worrisome possible complication of thyroid or parathyroid surgery. The rate of permanent nerve injury varies from 0-11% in the scientific literature. One of the largest studies addressing this specific complication was carried out by Dralle and associates in 2004 (2) . They examined 16,500 thyroid operations and 30,000 nerves at risk. They found that repeat (or “re-do”) operations on the thyroid and thyroid cancer operations were associated with a higher risk of nerve injury. Low volume surgeons had higher nerve injury rates.
Importantly, the nerve monitor device did not reduce the likelihood of recurrent laryngeal nerve injury. This finding reinforces established knowledge that protection of the nerve remains a function of surgeon skill.
UCLA study on endocrine surgery outcomes
One of the most comprehensive studies on outcomes in endocrine surgery was published by Stavrakis, Ituarte, Ko, and Yeh from UCLA in 2007 (3) . Our study examined 14,000 operations on the thyroid, parathyroids, and adrenal glands performed in the states of New York and Florida in the year 2002. The report was the first to encompass both inpatient and outpatient operations, the latter of which make up a growing proportion of endocrine procedures. Surgeons were categorized into six surgeon volume groups (SVG) in the following manner:
- Group A: 1-3 endocrine operations per year
- Group B: 4-8 endocrine operations per year
- Group C: 9-19 endocrine operations per year
- Group D: 20-50 endocrine operations per year
- Group E: 51-99 endocrine operations per year
- Group F: 100 or more endocrine operations per year
The categories were chosen to split the total number of operations evenly between the six groups, with each surgeon volume group responsible for about 2300 operations (Figure 1).
Several things can be learned by looking at the three pie charts in Figure 1:
- Group A (lowest volume) surgeons were responsible for 15% of all operations and 32% of all complications.
- Group F (highest volume) surgeons were responsible for 15% of all operations and 5% of all complications.
- About half of all endocrine operations are performed by surgeons performing fewer than 20 such procedures per year.
- Two-thirds of surgeons performing at least one endocrine operation per year are in the lowest volume group.
- Surgeons performing 100 or more endocrine operation yearly comprise only 1% of all surgeons studied.
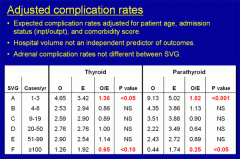
The table in Figure 2 shows complications rates that have been adjusted for factors that might make a given operation more risky (examples include advanced patient age, cancer, obesity, and bleeding disorders). Figure 2 shows that:
Figure 2. Adjusted complication rates for thyroid and parathyroid surgery according to surgeon volume group.
The lowest volume surgeons (1-3 endocrine operations per year) had a higher complication rate than average, whereas the highest volume surgeons (100+ endocrine operations per year) had a lower complication rate than average. This effect was most prominent for parathyroid surgery.
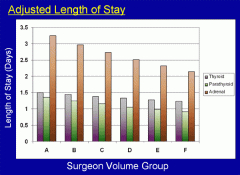
Figure 3. Length of hospitalization following thyroid, parathyroid, and adrenal surgery according to surgeon volume group.
Patients treated by more experienced surgeons tend to leave the hospital earlier after surgery.
- Patients treated by Group A (lowest volume) surgeons are more likely than average to experience complications (such as bleeding or nerve injury).
- Patients treated by Group F (highest volume) surgeons are less likely than average to experience complications.
- There is a fairly wide “middle ground” of surgeons performing 4-99 endocrine operations yearly. These surgeons have average complication rates.
Surgeon experience, length of hospitalization, and the cost of endocrine surgical care
In the present era of rising health care costs, economic outcomes of surgical care must also be examined. Figure 3 depicts our data on length of stay following endocrine surgery, and Figure 4 shows the total charges accrued during hospitalization. Along the bottom, we once again have categorized the data by surgeon volume group. Several things can be learned from examining these graphs:
- Increasing surgeon experience is associated with shorter length of hospitalization and reduced cost across all types of endocrine operations
- The beneficial effect of surgeon volume on economic outcomes is most pronounced with adrenal operations and parathyroid operations
- Among endocrine operations, those involving the adrenal gland are associated with the greatest length of stay and cost
These economic figures should be important to patients and insurers alike. Contrary to commonly held beliefs, treatment received at a specialty center is actually less expensive than that received at a non-specialty center. Patients recover more quickly and leave the hospital sooner after treatment by experienced surgeons.
Why does this make sense? Because the most costly aspect of surgical care arises from the need to manage complications. Avoidance of complications yields a win-win-win scenario with respect to patient outcomes, recovery time, and the overall cost of care. Specialty centers are also likely to have developed sophisticated systems of care that create standards of practice and reduce the likelihood of medical errors.
Outcomes in parathyroid surgery
Our study specifically and systematically examines outcomes in parathyroid surgery. To our knowledge, it is the first and only analysis of parathyroid surgery on this scale. In our assessment of both clinical and economic outcomes for various endocrine operations, parathyroid surgery was found to be the most sensitive to surgeon volume. Patients undergoing parathyroid surgery by the lowest volume surgeons were almost eight times more likely to experience complications than those treated by the highest volume surgeons (Figure 2).
Outcomes in adrenal surgery
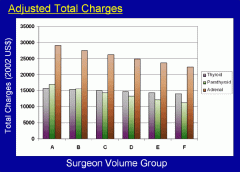
Figure 4. Total hospital charges during hospitalization for thyroid, parathyroid, and adrenal surgery according to surgeon volume group.
Surgical care provided by more experienced surgeons tends to be less costly. View larger image >
It is well known that adrenal diseases, such as pheochromocytoma, primary hyperaldosteronism ( Conn ’s syndrome), adrenal Cushing’s syndrome, and adrenocortical carcinoma, are often very complex and challenging to treat. Major physiologic changes arise from imbalances in adrenal hormones before surgery, during surgery, and after surgery.
Not surprisingly, adrenal surgery is associated with complication rates in the 15-20% range (3, 4) . Thus far, no clear relationship between surgeon volume and complication rates has been identified for adrenal surgery, suggesting that adrenal outcomes may largely be a function of the nature of disease. That said, the UCLA study demonstrated that surgeon experience in endocrine surgery was still associated with shorter hospitalization following adrenal surgery (Figure 3). Our conclusion was that experienced endocrine surgeons may be more skilled in effectively managing a certain number of inevitable complications that arise in the treatment of adrenal diseases.
Potential shortcomings of the UCLA study on endocrine surgery outcomes
We utilized state-level data from New York and Florida in 2002 for several reasons. These are highly populated states with well-maintained health care databases, particularly regarding outpatient surgery. There is often a 5-year lag time for a given year’s data to become available to researchers. These factors may limit the generalizability of our findings to the rest of the country, and to the health care landscape in 2008. The study is also limited by coding bias, meaning that we are dependent on state health administrators to accurately classify operations and complications. This process is prone to certain types of errors, which causes a degree of uncertainly in our results.
What are the implications of the UCLA study and others?
- In agreement with prior outcomes studies in the field (5) , we find that most common operations for endocrine disease are performed by surgeons who do not have a specific focus in endocrine surgery.
- This remains true despite the fact that experienced endocrine surgeons are consistently demonstrated to have better outcomes when compared to lower volume surgeons.
- Surgeons performing 100 or more endocrine operations yearly achieve optimal outcomes with respect to complication rates, length of hospitalization, and the cost of care.
- Surgeon experience appears to exert the greatest influence on outcomes of parathyroid surgery.
- From a health services standpoint, racial and economic inequality remain the most important barriers to achieving high quality care across the board. In keeping with findings by other researchers (6) , we found that patients treated by the lowest volume surgeons were the most likely to be non-white and to lack commercial insurance. For these disadvantaged groups, access to health care remains a critical issue.
References
- Sosa JA, Bowman HM, Tielsch JM, Powe NR, Gordon TA, and Udelsman R. The importance of surgeon experience for clinical and economic outcomes from thyroidectomy. Ann Surg, 228: 320-330, 1998.
- Dralle H, Sekulla C, Haerting J, Timmermann W, Neumann HJ, Kruse E, Grond S, Muhlig HP, Richter C, Voss J, Thomusch O, Lippert H, Gastinger I, Brauckhoff M, and Gimm O. Risk factors of paralysis and functional outcome after recurrent laryngeal nerve monitoring in thyroid surgery. Surgery, 136: 1310-1322, 2004.
- Stavrakis AI, Ituarte PH, Ko CY, and Yeh MW. Surgeon volume as a predictor of outcomes in inpatient and outpatient endocrine surgery. Surgery, 142: 887-899; discussion 887-899, 2007.
- Gallagher SF, Wahi M, Haines KL, Baksh K, Enriquez J, Lee TM, Murr MM, and Fabri PJ. Trends in adrenalectomy rates, indications, and physician volume: A statewide analysis of 1816 adrenalectomies. Surgery, 142: 1011-1021; discussion 1011-1021, 2007.
- Saunders BD, Wainess RM, Dimick JB, Doherty GM, Upchurch GR, and Gauger PG. Who performs endocrine operations in the United States? Surgery, 134: 924-931; discussion 931, 2003.
- Sosa JA, Mehta PJ, Wang TS, Yeo HL, and Roman SA. Racial disparities in clinical and economic outcomes from thyroidectomy. Ann Surg, 246: 1083-1091, 2007.