Critical Care Medicine Fellowship
We invite applications every year for our ACGME-accredited clinical fellowship in Critical Care Medicine. The fellowship is a multidisciplinary training program on the leading edge of intensivist training, delivering exceptional experiences in education, clinical exposure, and leadership in the rapidly advancing field of critical care medicine. It is designed to take the fellows through increasing levels of experience and responsibility, and prepare them for board certification in Critical Care Medicine. The Fellowship Program Director is Marisa Hernandez-Morgan, MD, MPP, and the Associate Program Director is Scott Vandiver, MD, PhD.
Our graduates are highly competitive in today's challenging healthcare market. Recent fellows have accepted excellent positions at private and academic medical centers including the University of Southern California Keck Medical Center, Long Beach Memorial Medical Center, Kaiser Permanente Santa Clara Medical Center, the University of Utah Health Care, the University of Texas Southwestern Medical Center, Santa Rosa Medical Center, and Northwell Health in New York. Several of our recent graduates have chosen to remain with us at UCLA and our associated West Los Angeles VA Medical Center.
On this page:
- Program Overview
- How does our program stand apart from other critical care fellowships?
- Clinical Curriculum
- Didactic Curriculum
- Research and Quality Improvement
- Faculty
- Application Process
- Current Fellows
- Recent Alumni
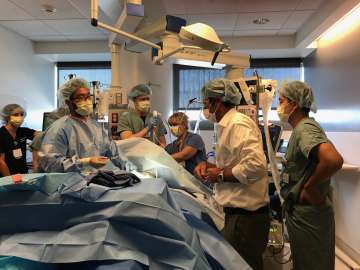
Program Overview
We are committed to the highest quality of training so that our fellows can become expert clinicians, educators, and leaders. Training takes place at the Ronald Reagan UCLA Medical Center and at the West Los Angeles Veterans Affairs Medical Center.
Ronald Reagan UCLA Medical Center (RRUMC) is a major medical center consistently ranked among the top hospitals in the U.S. It serves as a tertiary/quaternary referral center for Southern California, Arizona, Nevada, Hawaii, and other regions in the US and abroad. As a leading transplant center, RRUMC offers one of the largest multi-organ transplant programs on the west coast, providing services for heart, lung, liver, and kidney transplantations. In addition, UCLA is a Level I trauma center with a broad catchment area.
The West Los Angeles Veterans Affairs Medical Center (VAMC) is a major regional referral center for the veteran population. Patients are referred to the West LA VAMC from VA hospitals all over California for advanced surgical care in cardiothoracic, neurologic, and vascular surgery.
We currently offer five fellowship positions per year, and accept applications from qualified applicants with training backgrounds in anesthesiology, surgery, and emergency medicine.

How does our program stand apart from other critical care fellowships?
- Unparalleled clinical experience in one of the busiest transplant centers in the nation, combined with Level I trauma center experience and major referral center for Southwest USA, Hawaii, as well as many countries abroad.
- Extensive exposure to complex cardiac critical care, including a variety of mechanical circulatory support systems and adult congenital heart disease.
- Fellow-oriented educational program, where fellows are not considered solely as a necessary workforce required to “run the service”, and rotations focus on providing the best educational experience.
- Multidisciplinary team experience with strong teamwork among critical care faculty, surgical faculty, cardiology faculty, nurse practitioners, housestaff from many specialties, perfusionists, and pharmacists.
Clinical Curriculum
Our fellows rotate through several intensive care units during their training. Within the 12-month fellowship curriculum, fellows may choose six to eight weeks of non-ICU elective rotations from a broad range of ICU-associated subspecialty fields.

Cardiothoracic ICU (CTICU)
The CTICU rotation comprises the core of the fellowship. Our fellows oversee the medical management of cardiac surgical patients undergoing a vast variety of procedures including CABG, valve replacement, repair of adult congenital heart disease, mechanical circulatory support device implantation, and heart and lung transplantation. The CTICU is the only unit at UCLA to manage adult patients on veno-venous and veno-arterial extracorporeal membrane oxygenators (ECMO) during the bridge to recovery or bridge to transplantation process. The ICU team works closely with the cardiac surgical team, and directs the entire perioperative medical management of these highly complex patients. Fellows typically spend 12-16 weeks in the CTICU.
General Surgical ICU (SICU)
The SICU provides services to a diverse surgical patient population including trauma, general surgery, surgical oncology, vascular, thoracic, urologic, head-and-neck, orthopedic, and gynecologic patients. Fellows typical spend four to eight weeks on this rotation.
“Night Float”
On the "night float" rotation, our fellows care for CTICU and SICU patients at RRUMC. Typically, fellows spend 10-12 weeks on this assignment.
West Los Angeles VA SICU
At the West Los Angeles VA SICU, fellows care for a variety of surgical patients including patients recovering from cardiac, thoracic, vascular, neurosurgery, general surgery, and major head-and-neck operations. Fellows spend four to six weeks on rotation in the VA SICU.
Elective ICU Experience
Medical ICU (MICU)
The MICU at RRUMC is a 24-bed unit that takes care of complex patients with a variety of advanced disease processes, including pulmonary hypertension, end-stage lung disease, respiratory distress syndrome, and recovery after bone marrow transplantation. Fellows spend three to four weeks on the rotation under the supervision of MICU attending physicians.
Liver Transplant ICU
This ICU at RRUMC takes care of high-acuity patients with end-stage liver disease (ESLD), both pre- and post-liver transplantation. The experience provides fellows with broad exposure to patients with ESLD, emphasizing continuity throughout the full transplantation episode of care. Fellows typically spend three to four weeks in this unit, working in close collaboration with our liver transplant surgery team.
Neuroscience ICU (NSICU)
The NSICU at RRUMC provides state-of-the-art intensive care for a distinct patient population with complex neurological pathology including stroke, subarachnoid hemorrhage, traumatic brain injury, traumatic spinal cord injury, neuromuscular diseases, status epilepticus, and other neurologic critical illnesses. The Neuro ICU team utilizes a wide range of diagnostic modalities including continuous EEG, transcranial Doppler, brain oximetry, Xenon/computed tomography cerebral blood flow, microdialysis, and neuroimaging techniques. Fellows have the opportunity to rotate in the NSICU for one to two weeks.
Pediatric/Burn/Trauma ICU
Interested fellows may elect rotations in the Pediatric ICU at RRUMC, and the Burn and Trauma ICUs at the Los Angeles County and University of Southern California (LAC + USC) Medical Center.
Non-ICU Electives
Fellows have the opportunity to choose electives in non-ICU rotations, which can be organized according to the individual fellow's interests with the approval of the Fellowship Program Director. These include, but are not limited to:
- Advanced echocardiography training (critical care TTE and perioperative TTE/TEE)
- Blood bank
- Hematology
- Infectious disease
- Interventional pulmonology
- Interventional radiology
- Nephrology / renal replacement therapy consult
- Nutrition
- Palliative care
- Reading and research electives
Procedural Exposure and Training
Due to the high volume and complexity of patients in our ICUs, fellows gain experience with a variety of invasive diagnostic and therapeutic procedures, including:
- Placement of hemodialysis catheters, transvenous pacemakers, and pulmonary artery catheters
- Bronchoscopy
- Thoracentesis
- Paracentesis
- Tube thoracostomy
- Percutaneous tracheostomy
Didactic Curriculum
To balance a busy clinical service, we have developed a comprehensive didactic program to provide our fellows with state-of-the-art, evidence-guided lectures and journal clubs. During the first two weeks of their clinical rotations, fellows receive an intensive introductory lecture series that serves to orient them to the fundamentals of intensive care as well as to the particulars of the day-to-day operation of our ICUs. Besides daily bedside teaching, our didactic program includes:
Surgical ICU Journal Club:
These faculty-mentored, fellow-led, weekly group discussions, involving fellows, faculty, and residents, cover a variety of classic and recently published articles in critical care medicine.
Combined SICU/Trauma Surgery Journal Club:
This resident- and fellow-led monthly journal club is dedicated to review and analysis of important literature in the area of trauma critical care.
Surgical ICU Lecture Series:
These faculty-led, weekly in-depth lectures and interactive workshops cover a variety of critical care topics.
Combined ICU Lecture Series:
These are monthly lectures by members of the multidisciplinary ICU faculty (medicine, anesthesiology, surgery, and neurology).
Board Review:
This bi-monthly didactic session is dedicated to the review of topics and questions to assist with preparation for the Critical Care Medicine Board Examination. Fellows may also participate in our department’s “mock oral” board examinations in preparation for the ABA Applied Examination.
Echo/US Lecture Series:
These monthly lectures by critical care and cardiac anesthesiology faculty are dedicated to the theoretical foundation of echo and ultrasound technology. The didactic content complements hands-on training in echocardiography and point-of-care ultrasound (POCUS) provided during core ICU rotations and electives.
Critical Care M&M Conference:
The monthly SICU team M&M conferences cover case presentations and discussions to promote professionalism, ethical integrity, and transparency in assessing and improving patient care.
In addition, fellows are encouraged and given time to attend other didactic sessions that include Anesthesiology Grand Rounds, Surgery Grand Rounds, weekly cardiac anesthesiology lectures and TEE reviews, as well as quality improvement, research, risk management, and professionalism workshops.
Research and Quality Improvement
Our faculty are involved in a variety of clinical and translational research initiatives, and fellows are supported and encouraged to participate in research and quality improvement projects in many areas of critical care and perioperative medicine. Some of our ongoing projects include:
- Studies of injury and violence prevention in partnership with the Department of Health Services and the Department of Public Health (Dr. Dicker)
- Study of a novel angiotensin II agonist for vasodilatory shock – part of ATHOS investigators group (Dr. Boldt)
- Study of the effect of xenon on cerebral ischemia reperfusion following cardiac arrest (Dr. Boldt)
- “Gerofit” prehabilitation project – study of the use of structured prehabilitation in the elderly veteran population prior to surgery (Dr. Singh)
- Study of patient selection, risk assessment, and outcomes of multidisciplinary ECMO program (Dr. Gudzenko)
- Research study of perioperative factors on outcomes following lung transplantation (Dr. Gudzenko)
- Study of optimization of mechanical ventilation in interstitial lung disease (Dr. Ortiz)
- Development of new sepsis screening and triage tools, and sepsis bio-banking (Dr. Crager)
- Research on implementation of emergency critical care teams and the impact of the ED-ICU care model on patient outcomes and hospital operational efficiency (Dr. Crager)
- Development of and research in transitions of care and perioperative handoffs (Dr. Antongiorgi)
- Study of physician burnout in the perioperative setting (Dr. Antongiorgi)
Faculty
- Joseph Meltzer, MD, FASA - Medical Director, Cardiothoracic Intensive Care Unit, Professor of Clinical Anesthesiology
- Vadim Gudzenko, MD - Chief, Anesthesiology Critical Care Medicine
- Marisa Hernandez-Morgan, MD, MPP - Anesthesiology Critical Care Medicine Fellowship Program Director
- Scott Vandiver, MD, PhD - Anesthesiology Critical Care Medicine Fellowship Associate Program Director
- Brannon Altenhofen , MD
- Zarah Antongiorgi, MD
- David Boldt, MD, MS
- Sara Crager, MD
- Laleh Jalilian, MD
- Catherine Juillard, MD, MPH
- Ashie Kapoor, MD
- Catherine Lewis, MD
- George Lim, MD
- David Machado-Aranda, MD
- Jane Moon, MD
- Sirisha Rao, MD, MS
- Sumit Singh, MD
- Andrew Young, MD
Recent Alumni

Year | Fellow | Residency | Latest Employment |
|---|---|---|---|
2024-25 | Emma Huebner, MD | UCLA (Anes) | UW Medical Center - Montlake, Seattle, WA |
Andrew Lin, MD | Johns Hopkins University (EM) | USC Keck Medical Center, Los Angeles, CA | |
Nicole Shalit, MD | St. Elizabeth’s Medical Center (Anes) | Kaiser Permanente Los Angeles Medical Center, Los Angeles, CA | |
June Tong, MD | Harbor-UCLA Medical Center (Anes) | UT Houston, Houston, TX | |
Year | Fellow | Residency | Latest Employment |
2023-24 | Jason Batten, MD, MA (combined cardiothoracic anes) | Stanford University Hospitals and Clinics (Anes) | UCLA Medical Center, Los Angeles, CA |
Joshua Hubert, DO, MS | Tufts Medical Center (Anes) | Tufts Medical Center, Boston, MA | |
Nicholas Kalekas, DO | Loma Linda University Medical Center (Anes) | Valley Health System, St Rose Health System, HCA Hospitals, Las Vegas, NV | |
Sergey Progushev, MD | UCLA (Anes) | Northridge Hospital, Northridge, CA | |
Year | Fellow | Residency | Latest Employment |
2022-23 | Brannon Altenhofen, MD | UCLA (Anes) | UCLA Medical Center, Los Angeles, CA |
Jeanette Chin, MD | UT Southwestern Medical Center (Anes) | Kaiser Permanente, San Jose Medical Center, San Jose CA | |
Sean Hickey, MD | Mount Sinai NYC (EM) | Hackensack Meridian Health, Hackensack, NJ | |
Ashie Kapoor, MD | Sunrise Health GME (Anes) | UCLA Medical Center, Los Angeles, CA | |
Year | Fellow | Residency | Latest Employment |
2021-22 | Garry Dieter, MD | Virginia Mason Medical (Anes) | Providence Sacred Heart Medical Center, Spokane, WA |
Albert Lee, MD (combined cardiothoracic anes) | UCLA (Anes) | USC Keck Medical Center, Los Angeles, CA | |
Mohammad-Ali Shaikh, MD | UT Southwestern Medical Center (Anes) | UT Southwestern Medical Center, Dallas, TX | |
Year | Fellow | Residency | Latest Employment |
2020-21 | Krisztina Escallier, MD (combined cardiothoracic anes) | Washington University in St. Louis (Anes) | USC Keck Medical Center, Los Angeles, CA |
Kasey Grewe, MD (combined cardiothoracic anes) | Columbia University (Anes) | Santa Barbara Cottage Hospital, Santa Barbara, CA | |
Melanie Kusonruksa, MD | UCLA (Anes) | USC Keck Medical Center, Los Angeles, CA | |
James Madrian, MD | University of Iowa (Anes) | Providence Spokane Anesthesia Group & Sound Intensivist Group, Spokane, WA | |
Year | Fellow | Residency | Latest Employment |
2019-20 | Allison Ferreira, MD | UCLA (EM) | USC Keck Medical Center, Los Angeles, CA |
Vikram Fielding Singh, MD, JD (combined cardiothoracic anes) | UCSF (Anes) | Stanford University, Stanford, CA | |
Samuel Hong, MD | UCLA (Anes) | VA Greater Los Angeles Healthcare System, Los Angeles, CA | |
Eugene Won, MD | UCI (Surg) | Southwest Cardiothoracic Surgeons, Plano, TX | |
Year | Fellow | Residency | Latest Employment |
2018-19 | Marisa Hernandez-Morgan, MD, MPP (combined cardiothoracic anes) | UCSF (Anes) | UCLA Medical Center, Los Angeles, CA |
Joseph Seif, MD | UCLA (Anes) | Anesthesia Service Medical Group, San Diego, CA | |
Matthew Scott Vandiver, MD, PhD | Johns Hopkins University (Anes) | UCLA Medical Center, Los Angeles, CA | |
Year | Fellow | Residency | Latest Employment |
2017-18 | Jeffrey Kim, MD (combined cardiothoracic anes) | UCSF (Anes) | Kaiser Permanente Los Angeles Medical Center, Los Angeles, CA |
George Lim, MD | Mount Sinai NYC (EM) | UCLA Medical Center, Los Angeles, CA | |
Michael Wolfe, MD | MGH (Anes) | Hoag Hospital, Newport Beach, CA | |
Year | Fellow | Residency | Latest Employment |
2016-17 | John Michael Guthrie, MD | Mount Sinai NYC (EM) | Hoag Hospital, Newport Beach, CA |
Sirisha Rao, MD, MS | Yale University (Anes) | UCLA Medical Center/VA Greater Los Angeles Healthcare System, Los Angeles, CA | |
Andrew Young, MD | UCLA (Anes) | UCLA Medical Center, Los Angeles, CA | |
Year | Fellow | Residency | Latest Employment |
2015-16 | William Alexander Edwards, MD (combined cardiothoracic anes) | UCSF (Anes) | Kaiser Permanente Santa Clara Medical Center, Santa Clara, CA |
Joseph Guenzer, MD | University of Chicago (Anes) | University of Utah Health Care, Salt Lake City, UT |