Arteriovenous Malformations (AVM)
Find your care
Our expert team is skilled at treating complex cerebrovascular conditions and providing the finest and most comprehensive patient care. For help finding a neurosurgeon, call 310-825-5111.
What is an arteriovenous malformation (AVM)?
An arteriovenous malformation is a tangled mass of abnormal blood vessels that connect arteries directly to veins in the brain or spinal cord. Normally, those systems are separated – the arteries carry blood from the heart through the brain tissue, and the veins then move it back to the heart under low pressure. Blood flows rapidly through an AVM because of these abnormal vessels and connections between arteries and veins. This causes significant stress on the blood vessels and the surrounding brain tissue that can result in rupture of the vessels, bleeding in the brain, seizures and other neurological symptoms.
What are the symptoms of an AVM?
AVMs often create no symptoms and go undiagnosed until they cause bleeding. Symptoms that can indicate the presence of an AVM include:
- Seizures
- Headaches
- Dizziness
- Hearing a "bruit"—an audible whooshing sound caused by the blood flow in the vein
- Cognitive dysfunction
How is an AVM diagnosed?
At UCLA, our neurosurgeons use the most advanced technology and latest imaging systems to diagnose AVMs quickly and accurately. In many cases, an AVM is discovered once it has ruptured, but we do everything possible to diagnose and manage them before this happens. During your examination, your expert team may use the following imaging techniques to locate and assess your AVM:
- Magnetic resonance imaging (MRI) scans are used to identify and locate an AVM.
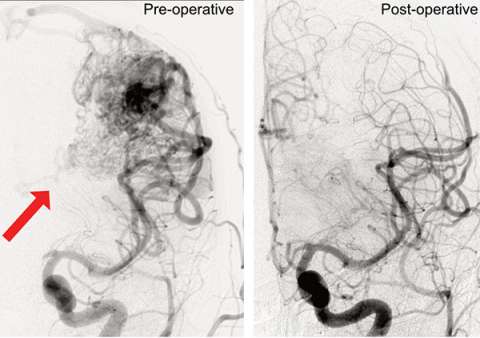
- Cerebral angiography provides the most accurate images of the blood vessels and arteries affected by the AVM. This is the gold-standard imaging study for analyzing blood vessels of the brain. It can be used to find even very small AVMs that are missed on other types of imaging studies.
How is an AVM treated?
Once it's been evaluated, your AVM will be graded based on its size, location and blood flow pattern — the higher the grade, the more difficult it is to treat. At UCLA, a multidisciplinary team of neurovascular experts will meet to review your case and create a customized treatment plan. We typically treat AVMs using strategies that include some combination of:
- Microsurgical resection: During this open surgery procedure, the neurosurgeon removes the AVM from the brain or spinal cord. At UCLA, we use the most modern surgical techniques to safely remove AVMs and help protect brain function. We also use 3-D virtual reality before surgery to map out a patient’s precise anatomy and advanced imaging systems during surgery to guide the procedure.
- Stereotactic radiosurgery: These minimally invasive techniques (Gamma Knife®, CyberKnife®, LINAC and proton beam therapy) can be used to treat AVMs in critical locations. During the procedure, we deliver a concentrated dose of radiation to the AVM. Within about two years, the vessels of the AVM gradually close off, reducing the risk of hemorrhage.
- Endovascular embolization: This minimally invasive technique is performed by inserting a catheter through the groin and directly into the vessels that supply blood to the AVM. A liquid that solidifies in the blood vessel and cuts off blood flow to the AVM is injected through the catheter. The cerebrovascular team at UCLA is actively involved in research and testing of new liquid embolic treatments.
- Genetic research: Our researchers are studying what role familial genetics and sporadic gene alterations might play in AVMs and how they develop. This research may help identify potential alternative treatment options.
- Clinical trials: At UCLA, we are one of only a few neurovascular centers in the country enrolling patients in medical trials for the treatment of AVMs. Patients will be evaluated for newer treatments and clinical trials as appropriate.
Contact us
To schedule an appointment at the UCLA Cerebrovascular Program, please call 310-825-5111 or request a call back for an appointment.

Geoffrey Colby, MD, PhD

Jeremiah Johnson, MD
