Carotid Stenosis
Find your care
Our expert team is skilled at treating complex cerebrovascular conditions and providing the finest and most comprehensive patient care. For help finding a neurosurgeon, call 310-825-5111.
Overview
What is carotid stenosis?
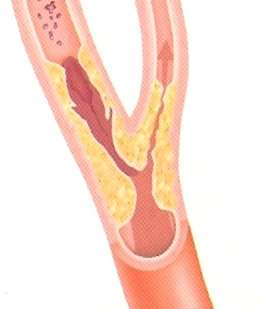
Carotid stenosis is a medical condition in which the carotid artery, typically in the neck, is narrowed. This happens most often because of plaque buildup inside the artery, called atherosclerosis. As the carotid artery atherosclerotic plaque builds, the artery becomes narrower and less blood is able to flow into the brain (Figure 1). Additionally, blood clots can develop on or near the plaque leading to a strokes. Depending on the situation, carotid stenosis may be treated with medical management, Carotid Endarterectomy or Carotid Stenting procedures.
What are the symptoms of carotid stenosis?
Carotid stenosis causes transient ischemic attacks (TIAs). These “mini-strokes” result from a temporary disruption of blood flow into the brain. They cause stroke-like symptoms, but don’t result in permanent damage or loss of function. Carotid stenosis can also cause strokes (and people who experience TIAs are at a higher risk of later developing a stroke), so pay attention to the warning signs.
Carotid Stenosis can lead to a stroke - it is important to know and recognize the most common signs of a stroke and call 911 immediately if you or someone around you experience them. Symptoms of a stroke usually appear suddenly, and the sooner you get treatment, the better the outcome. These symptoms include:
- Weakness, numbness or paralysis – often on one side of the body
- Drooping on one side of the face
- Difficulty speaking or understanding speech
- Dizziness
- Loss of balance or coordination or difficulty walking
- Sudden vision changes in one eye (for example, a black shade)
- Loss of consciousness
When to see a doctor urgently
Seek urgent medical attention if you notice any signs or symptoms of a stroke or TIA, even if they come and go or disappear.
To remember the signs of a stroke, think "FAST" and do the following:
- Face. Ask the person to smile. Does one side of the face droop?
- Arms. Ask the person to raise both arms. Does one arm drift downward? Or is one arm unable to rise? If so, call 911.
- Speech. Ask the person to repeat a simple phrase. Is his or her speech slurred or strange? If so, call 911.
- Time. If you observe any of these signs, call 911 or emergency medical help immediately as time is critical.
Call 911 or your local emergency number immediately. Don't wait to see if symptoms go away. The longer the time before stroke treatment, the greater the chance of brain damage and disability.
Risk Factors
What puts someone at risk of developing carotid stenosis?
The risk factors for developing atherosclerosis include, but are not limited to:
- High blood pressure
- High cholesterol
- Smoking
- Diabetes
- Obesity
- Unhealthy diet
- Lack of exercise
Diagnosis
How is carotid stenosis diagnosed?
If you experience a TIA, our team of cerebrovascular specialists will use a variety of advanced imaging techniques to help determine if carotid stenosis is the cause. These include:
- Carotid Doppler ultrasound is widely used for evaluating carotid vascular disease. The velocity of the flow of blood through the carotid artery is used to determine the degree of plaque buildup in the artery.
- Magnetic resonance angiography (MRA) is a noninvasive procedure that uses various magnetic resonance imaging (MRI) techniques to produce images of the insides of the blood vessels.
- Computed tomography angiography (CTA) is a noninvasive test that uses injected contrast dye and CT scanning to identify narrowing of the blood vessels.
- Cerebral and cervical angiography is a procedure where a small catheter is inserted into the blood vessels of the body to inject contrast dye to provide the most detailed images of the blood vessels of the neck and brain. This procedure also assesses blood flow through the vessel.
Untreated carotid stenosis
Once a patient has experienced a stroke or TIA from carotid stenosis, the risk of having another stroke is about 25% in next two years without treatment. This is a high risk. The stroke risk of a patient with asymptomatic carotid narrowing is much lower. In general, the narrower the artery, the higher the risk of stroke.
Treatment
When to operate on carotid stenosis?
Each patient’s situation is unique, and a multidisciplinary team of neurovascular experts will meet and review your case to develop a customized treatment plan. Management recommendations are different for patients who have no symptoms related to the carotid stenosis (asymptomatic patients) compared to patients who recently had symptoms related to the carotid artery stenosis, such as a TIA or stroke. Each situation is unique. Some general guidelines are as follows:
- Medical Management: This refers to management of risk factors (for example, hypertension, diabetes, hyperlipidemia) with medication and lifestyle modification. This often includes use of an anti-platelet medication or anticoagulation medication (blood thinner). This treatment plan is often recommended if the carotid artery stenosis is less than 60% for asymptomatic patients or less than 50% for patients who have had recent symptoms related to the artery narrowing.
- Carotid Surgery or Stenting: Carotid artery endarterectomy (surgery to remove the plaque) and stenting have been shown to be beneficial in symptomatic patients with stenosis measuring above 70% and modestly beneficial in patients with symptoms and carotid stenosis measuring 50-69%. It best to operate within 2 weeks of symptoms occurring. Asymptomatic patients have been shown to benefit from surgery when the artery stenosis is 60% or greater. However, treatments are continuously being developed and tested in trials to update these basic guidelines.
How is carotid stenosis treated?
At UCLA, a multidisciplinary team of neurovascular experts will meet to review your case and create a customized treatment plan. Treatment may include:
- Medical Management (options include):
- Aspirin or other antiplatelet medications
- Anticoagulant medication (blood thinners)
- Blood pressure control medications
- Cholesterol-fighting medications
- Diabetes control
- Increased physical activity
- Weight loss
- Intervention to help patients stop smoking.
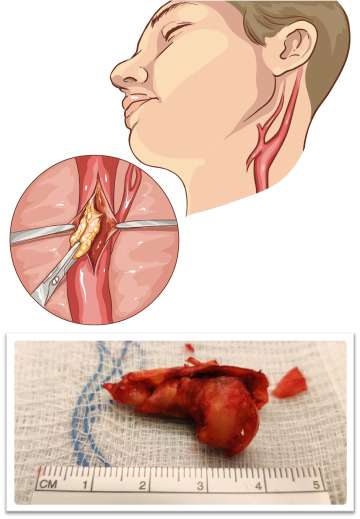
- Carotid Endarterectomy: This procedure is used to surgically open the carotid artery in the neck, remove the plaque, and re-construct the artery to improve blood flow and prevent future strokes (Figure 2). This is considered the standard surgical treatment for carotid stenosis needing operative treatment. Among patients with greater than 70% blockage, performing carotid endarterectomy surgery reduces the rate of stroke over the next two years by 17% and the risk of major stroke or death by 10.6% compared to medical management.
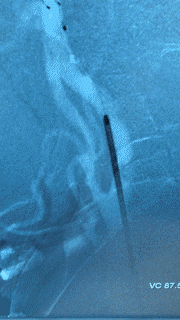
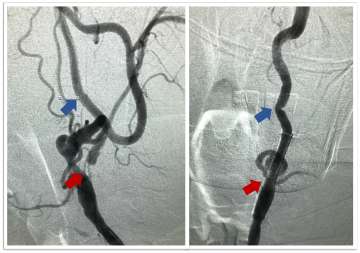
- Carotid Artery Stenting: This is a newer endovascular procedure performed from the inside of the blood vessels to open the stenosis. The surgeon uses small tubes and wires inserted into the wrist or groin arteries, navigated to the carotid artery in the neck. An umbrella is positioned above the narrowing to catch any debris and a stent is delivered to dilate the region of stenosis and hold the vessel open, improve flow and prevent future strokes (Figures 3 and 4).
Latest Research
CREST 2 is a national and international clinical trial comparing treatment of asymptomatic carotid stenosis (narrowing of 70% or more) with either carotid endarterectomy, carotid stenting, or medical management. The goal of this study is to improve our understanding of when it is best to treat asymptomatic carotid stenosis with carotid endarterectomy surgery, carotid stenting surgery or intensive medical management.
At UCLA Health neurosciences, we employ highly specialized multidisciplinary health care teams, and in addition to innovative cutting-edge care, we provide support services for patients and their families to help navigate their time in our clinics and hospitals.
Contact us
To schedule an appointment at the UCLA Cerebrovascular Program, please call 310-825-5111 or request a call back for an appointment.

Geoffrey Colby, MD, PhD

Jeremiah Johnson, MD
