Cavernous Malformation
Find your care
Our expert team is skilled at treating complex cerebrovascular conditions and providing the finest and most comprehensive patient care. For help finding a neurosurgeon, call 310-825-5111.

Overview
What are cavernous malformations?
Cavernous malformations of the brain and spinal cord are clusters of thin-walled blood vessels that are filled with slow-moving or clotted blood. They are often describe as looking like a “mulberry.” Since they are fragile, they frequently leak small amounts of blood, creating the appearance of growth, and sometimes triggering inflammation in surrounding nervous tissues. Severe bleeding events from cavernous malformations, though rare, can also occur, and can result in neurologic dysfunction. Cerebral cavernous malformations (CCMs) are also known as “cavernous angiomas,” or simply “cavernomas.” They can appear as a single lesion or with multiple lesions, or be part of a genetic syndrome in which multiple CCMs are present.
What are the symptoms of a cavernous malformation?
Many people with CCMs never experience symptoms. The type and severity of symptoms varies according to the CCM’s location. Possible symptoms may include:
- Headaches
- Changes in hearing or vision
- Seizures
- Muscle weakness or paralysis
- Severe bleeding from a CCM is an important cause of hemorrhagic stroke. This is a serious condition that requires immediate medical attention.
Diagnosis
How are cavernous malformations diagnosed?
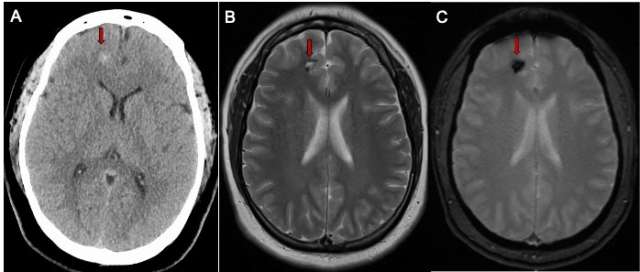
Whether the CCM has caused bleeding or not, the following advanced imaging (Figure 1) techniques may be used to diagnose it:
- Magnetic resonance imaging (MRI) scan can help locate the CCM and the area of affected brain or spinal cord.
- Computed tomography (CT) scan can assess any bleeding into the brain tissue.
Genetics
There are two forms of CCMs: sporadic and familial. The majority of cases are sporadic, in which there is usually only one CCM present on MRI. A patient with a single, sporadic CCM is not more likely to have a child with CCMs. Approximately 20% of cavernous malformation cases are familial, and the genes leading to CCMs may be passed from parent to children in an autosomal dominant pattern. Individuals with familial CCM are more likely to have multiple cavernous malformations. Genetic testing may be warranted if an individual has multiple CCMs and/or there are multiple family members with known CCMs.
Treatment
How are cavernous malformations treated?
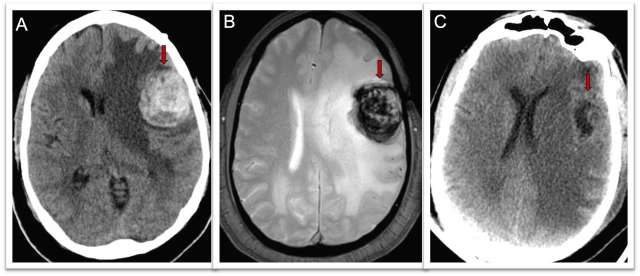
Treatment of a CCM depends on its location and the symptoms it causes (most commonly from bleeding events). Your doctor may recommend monitoring it with MRIs and treating symptoms with medications (Figure 2). If surgical treatment is necessary, the cerebrovascular surgeons at UCLA are expertly trained in this specialized procedure, and have performed a high volume of these surgeries. In each case, we aim to perform these surgeries in the most minimally-invasive way possible, removing the CCM with the least disruption of normal tissue.
Contact us
To schedule an appointment at the UCLA Cerebrovascular Program, please call 310-825-5111 or request a call back for an appointment.

Geoffrey Colby, MD, PhD

Jeremiah Johnson, MD
