Seromas and Hematomas in the Breast
By: Joshi Madhu, MD and Daniel Bradley, MD.
Seroma
Seromas in the breast are harmless fluid-filled pockets that can develop after surgery, trauma, or injury to the breast tissue. In breast surgeries, such as mastectomies and lumpectomies, the excision of breast tissue can lead to the accumulation of fluid within the resulting dead space left behind. Breast seromas can often be palpated on physical examination. Ultrasound and mammography can be used for definitive diagnosis and to determine its size and location.
On ultrasound, seromas will present as a fluid-filled collection, which is well-circumscribed and anechoic or hypoechoic in echogenicity. The fluid within the seroma may be simple in appearance or mildly complex, often exhibiting posterior acoustic enhancement. When direct pressure is applied with the ultrasound probe during imaging, the seroma may compress, causing a change in shape or size.
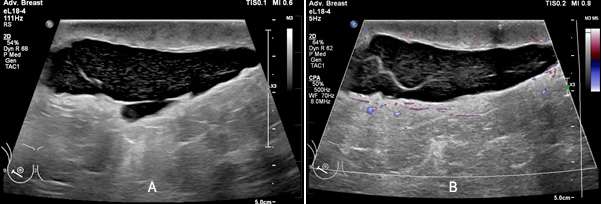
On mammogram, seromas often appear as well-defined masses that are found within or adjacent to a surgical site. When the breast is compressed during a mammogram, the fluid collection may slightly change in shape or size. This compression effect observed on mammograms may aid in distinguishing these fluid-filled structures from solid masses.
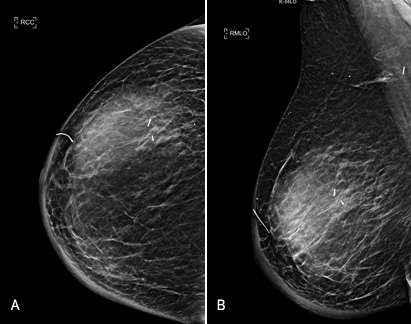
Management of breast seromas depends on the size and severity of symptoms of the seroma. Small seromas often resolve without intervention and may be monitored clinically. Larger or symptomatic seromas can be treated with aspiration, compression, drain placement, or in rare cases with surgical excision of the seroma cavity.
Hematoma
A hematoma is a localized collection of blood outside of blood vessels, that can lead to swelling, pain, and discomfort. Breast hematomas may occur for a variety of reasons including trauma, surgery, or anticoagulation. Trauma and surgery can cause the damage/rupture of blood vessels in the breast causing blood to pool at the site of injury. Individuals taking anticoagulants are at a higher risk of developing hematomas due to the blood-thinning effects of these drugs. In these patients even minor injuries causing prolonged bleeding and hematoma formation.
On ultrasound, hematomas can have variable appearance depending on the age of the blood products.
- Acute hematomas typically appear as hypoechoic fluid collections as acute blood products are less reflective to ultrasound waves compared to surrounding tissues. They may have well-defined or irregular borders depending on the integrity/composition of the surrounding tissue and typically have homogenous internal echogenicity. Color Doppler imaging may be useful in identifying an active bleed if a damaged vessel is visualized adjacent to a developing hematoma. Acute hematomas sometimes exhibit posterior acoustic enhancement.
- Chronic hematomas often appear more heterogeneous on ultrasound compared to acute hematomas because of the breakdown of blood components and the formation of fibrin. Chronic hematomas may form a fibrous capsule as the body attempts to encapsulate and contain the hematoma. Margins may be well circumscribed but may be partially indistinct due to the presence of internal echoes. Color Doppler imaging typically exhibits reduced vascularity as the body works to reduce blood flow at the site of a bleed. In contrast to acute hematomas, chronic hematomas may exhibit posterior acoustic shadowing due to the age of blood products within the hematoma which may produce internal echoes.
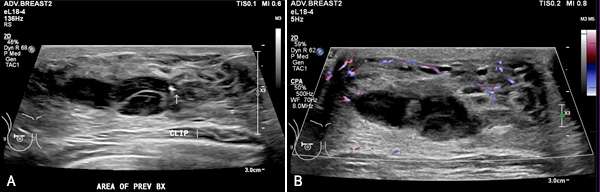
On mammogram, hematomas appear similar to other fluid collections and most commonly appear as a well-defined mass or region of increased density. Borders may be well circumscribed or ill-defined depending on acuity of the hematoma and the integrity of the surrounding tissue. In areas of chronic hematoma, small calcium deposits may develop and evolve into areas of fat necrosis. Similar to seromas, during compression a hematoma may change in shape on mammograms.
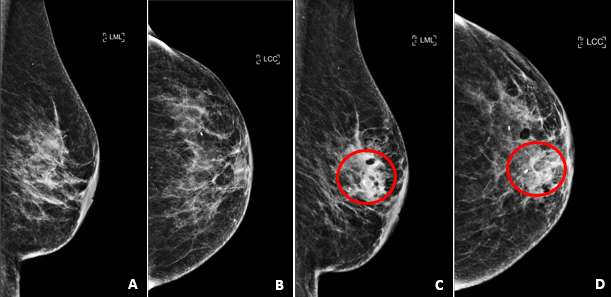
Management of breast hematomas depends on the severity of bleeding encountered at the time of injury and the size of the resultant hematoma. Bleeding associated with biopsy can be reduced with the use of lidocaine with epinephrine in order to constrict surrounding vessels. After biopsy, consistent and steady manual compression or a pressure bandage can aid hemostasis. In cases of arterial injury and/or prolonged bleeding, selective angiography and embolization versus surgical intervention can be considered.
References
- Mahoney MC, Ingram AD. "Breast Emergencies: Types, Imaging Features, and Management." AJR Am J Roentgenol. 2014 Apr;202(4):W390-9. DOI: 10.2214/AJR.13.11758. PMID: 24660738.
- Neal CH, Yilmaz ZN, Noroozian M, Klein KA, Sundaram B, Kazerooni EA, Stojanovska J. "Imaging of Breast Cancer-Related Changes After Surgical Therapy." AJR Am J Roentgenol. 2014 Feb;202(2):262-72. DOI: 10.2214/AJR.13.11517. PMID: 24450664.